[ad_1]
Let’s discuss the safety and efficacy of various weight-loss methods, ranging from Botox and corsets to siphons and tapeworms.
A moderately obese person doing moderately intense physical activity, like biking or brisk walking, would burn off approximately 350 calories an hour, but most drinks, snacks, and other processed junk are consumed at a rate of about 70 calories (293 kJ) per minute. Therefore, it only takes five minutes to wipe out a whole hour of exercise.
Enter the AspireAssist siphon assembly.
It’s a percutaneous gastrostomy device, meaning surgeons cut a hole in a person’s stomach and tunnel a fistula out through the abdominal wall. So, after each meal, the person can attach a suction gadget to the hole and directly drain out their stomach contents, as you can see below and at 0:47 in my video Extreme Weight-Loss Devices.
This means you could gorge on donuts, spew them out through the hole in your stomach, then gorge on more donuts. Have your cake, and eat it, too…and two, three, and four times!
It seems to be the quintessential American invention, straight from the land that brought us Jell-O salads, spray cheese, and deep-fried Snickers bars. Patients do lose weight, perhaps in part because the fistula may interfere with the relaxation of the stomach wall during a meal. The process also requires drinking lots of water and thoroughly chewing food, both of which may help with weight loss by increasing hydration and slowing the eating rate. Patients also started making healthier choices to avoid the unpleasant sight of gastric aspirate from unhealthy foods. (The tubing is clear, and, evidently, fried foods look particularly gross as they are pumped out.)
All patients need to take supplemental potassium, since it’s sucked out in stomach juices. Otherwise, they risk becoming potassium-deficient (a common complication in bulimia), but most side effects are just minor wound complications. Serious adverse effects, like abdominal abscesses, are rare. The big selling point is that the siphon device doesn’t change the gastrointestinal tract’s anatomy. That seems like a low bar, but in today’s Wild West world of weight-loss procedures, you can’t take anything for granted. Take the duodenal-jejunal bypass liner, for example.
Gastric bypass surgery works in part by cutting out a portion of the small intestine so it’s no longer in the flow of food, thereby helping to prevent the absorption of calories. Instead of major surgery, how about just dropping down a couple of feet of plastic tubing to line the intestinal walls? The problem with the EndoBarrier is that it has to be anchored in the digestive tract. This is accomplished with 10 barbed hooks that cause lacerations, accounting for the majority of the 891 adverse effects reported in 1,056 patients—nearly 9 out of 10 people. Severe penetrating trauma, resulting in esophageal perforation or liver abscesses, is rarer (occurring in only about 1 in 27 patients).
Concern has been raised about the “palatability” of the AspireAssist stomach pump, but the most cringeworthy endoscopic procedure I discovered in my research was intestinal “resurfacing.” Why cover the inside of your intestines with plastic to prevent absorption when you can just “thermally ablate the superficial duodenal mucosa”? In other words, have your intestinal lining burned off—or rather, “resurfaced.”
Surgeons have tried injecting Botox into the stomach walls of obese individuals, hoping it would partially paralyze their gastric muscles, slow stomach emptying, make people feel fuller longer, and lose weight. It didn’t work.
Researchers in Sweden tried randomizing people to wear corsets for 12 to 16 hours a day, seven days a week, for nine months. And it didn’t work. The study participants just didn’t wear the corsets—they were “perceived as uncomfortable.” Duh.
“Sanitized tapeworms” have evidently been widely advertised as a weight-loss remedy since back in the early 1900s. The fact that living tapeworms have been discovered during bariatric surgery operations suggests that infesting yourself with parasites may not be particularly effective either.
Speaking of disgusting strategies, how about disgust itself? A study entitled “Harnessing the Power of Disgust: A Randomized Trial to Reduce High-Calorie Food Appeal Through Implicit Priming” tried using subliminal messages to ruin people’s appetite. Just before showing images of healthy foods, researchers briefly flashed happy images—such as a group of kittens—for 20 milliseconds. That’s too quick to consciously register, but the hope was to plant a positive imprint on the brain. Before showing images of high-calorie foods like ice cream, they flashed negative scenes, like a cockroach on a pizza slice, vomit in a dirty bathroom, and a burn wound. Apparently, it worked! Subjects subsequently reported a reduced desire to eat high-calorie foods, though this wasn’t tested directly. The researchers concluded that subliminal revulsion might be “a successful tactic to combat the onslaught of food cues that promote unhealthy eating….”
The rest of the world looks on, bemused by American machinations, penning commentaries like “Don’t Let Them Eat Cake! A View from Across the Pond.” A paper in the journal Obesity Surgery entitled “What Are the Yanks Doing?” reviewed “The U.S. Experience with Implantable Gastric Stimulation,” inserting electrodes into the muscular layer of the stomach wall. When that didn’t work, colon electrical stimulation was tried.
Even more shocking were studies like “Repetitive electric brain stimulation reduces food intake in humans.” Though placing deep-brain electrodes is considered a complication-prone operation, scientists have long pondered whether “placing an electrode somewhere in the brain could make people eat less.” Holes were drilled through the skulls of five obese individuals, and wires were pushed into their brains for “electrostimulatory exploration.” Once the researchers poked around and found spots where they were able to elicit convincing hunger responses, they sent in enough juice to fry out electro-coagulatory lesions. It seemed to work in cats and monkeys, but the researchers found that burning holes in people’s brains did not result in weight loss in obese humans. Thankfully, as I explained in my book How Not to Diet, healthy, sustainable weight loss isn’t brain surgery.
Doctor’s Note
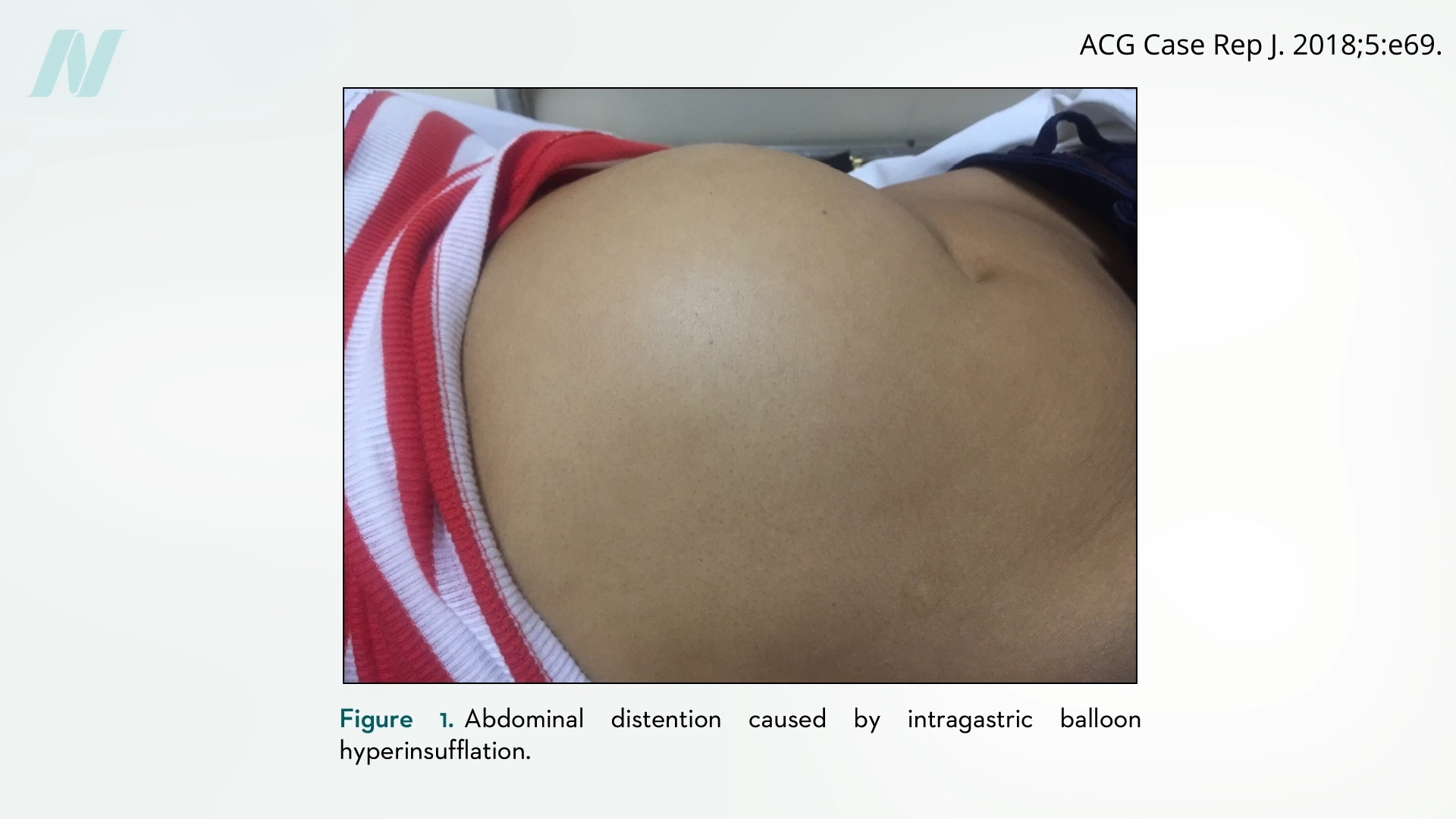
Check out Is Gastric Balloon Surgery Safe and Effective for Weight Loss?.
What about drugs? See Are Weight Loss Pills Safe? and Are Weight Loss Pills Effective?.
So, what’s the best way to lose weight? I wrote a whole book about it! How Not to Diet is focused exclusively on sustainable weight loss. Borrow it from your local library or pick up a copy from your favorite bookseller. (All proceeds from my books are donated to charity.) To whet your appetite, take a peek: Trailer for How Not to Diet: Dr. Greger’s Guide to Weight Loss.
For more on this topic, check out related posts below.
[ad_2]
Michael Greger M.D. FACLM
Source link