How might we moderate the rare but very real risk of headbanging?
If you search for heavy metal in the National Library of Medicine database, most of what you find is on heavy metal contamination in fish, which “makes it difficult to establish clearly the role of fish consumption on a healthy diet” and perhaps helps to explain the quintupling of odds of autoimmune diseases, such as juvenile arthritis. But searching for the hazards of heavy metal also pops up entries on the “risks from heavy metal music.” In this study, researchers were talking about traumatic injuries from slamming around “during a moshing session,” but you’re more likely to get injured at an alternative rock concert. (Check out some of the artists below and at 0:50 in my video The Dangerous Effects of Heavy Metal Music.)
Certainly, music-induced hearing loss is a serious problem, but that can result from any loud music. Clinical recommendations include the “80–90 rule”—no more than 80% of the maximum volume on personal listening devices for no more than 90 minutes a day. That’s not what the science shows, however. “Do not exceed 60% of the maximum volume” may be more evidence-based, but researchers figure teens would just ignore that, so they came up with more “acceptable” advice.
I assumed I’d see a lot of satanic panic nonsense from the 1980s, when “parents bereaved by suicide…accused Heavy Metal groups of promoting suicidal behaviours and…proceeded to sue musicians.” What kind of evidence did the parents present? There has been “little scholarly research” published until the “The Heavy Metal Subculture and Suicide” paper that tried to correlate the number of statewide heavy metal magazine subscriptions to youth suicide rates. Seriously?
It got really wild, though, when researchers called psychiatric institutions, pretending to be parents worried because their son started listening to heavy metal music, even though they made it clear that their son didn’t exhibit any symptoms of mental illness, didn’t do drugs or drink alcohol, and was doing fine at school. Ten of the twelve facilities believed the son required psychiatric hospitalization. Imagine what that would do to a kid! Researchers found that, decades later, metalheads “were significantly happier in their youth and better adjusted” than their peers.
Some studies were strange. Do Parkinson’s patients walk better listening to The Beatles’ “Yellow Submarine” or Metallica’s “Master of Puppets”? (See below and at 2:32 in my video.)
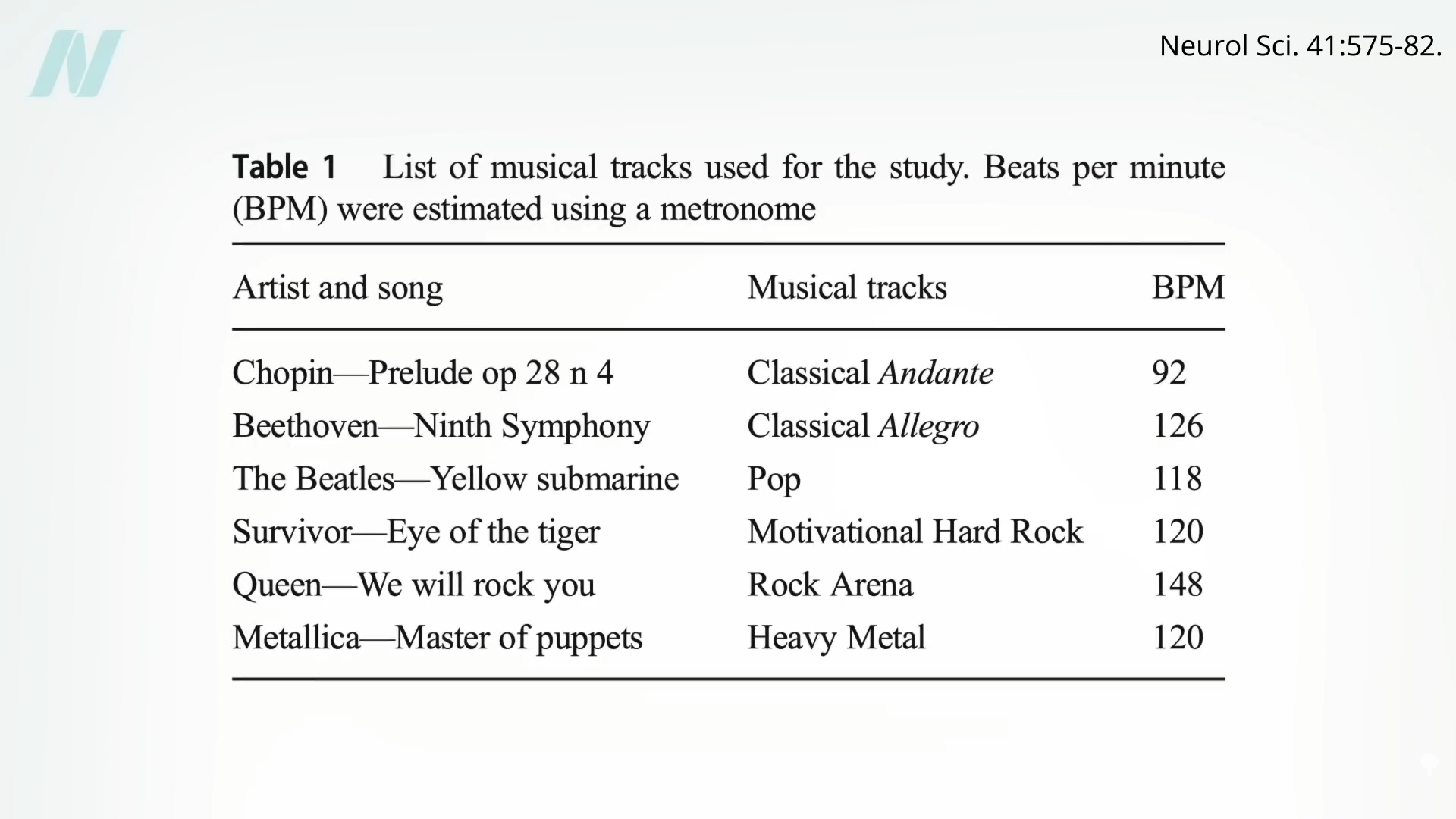

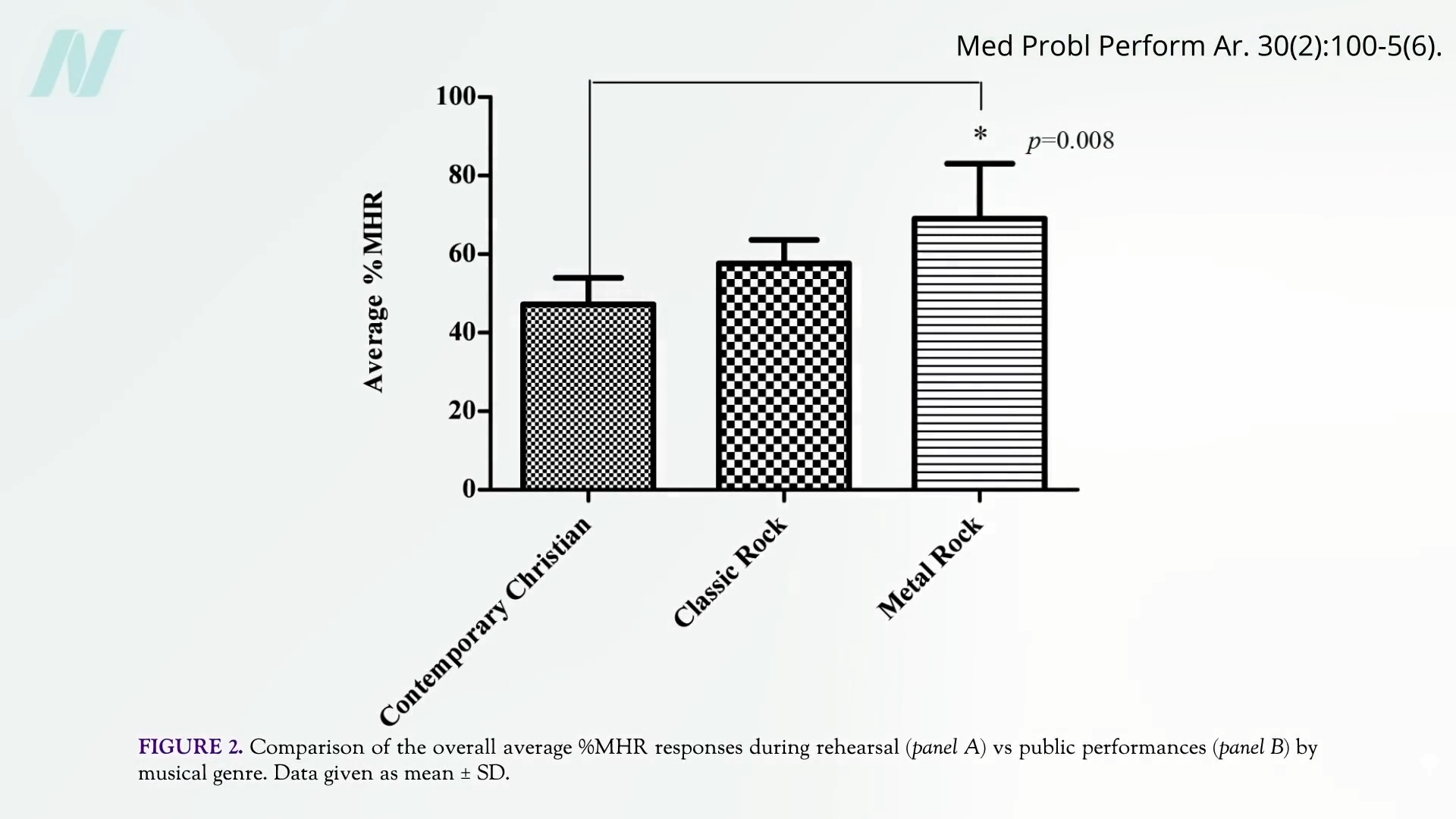
Others were pretty nondescript. Heavy metal musicians exhibit a higher heart rate than those performing “contemporary Christian,” which isn’t so surprising, as you can see here and at 2:40.
Some others were kind of cute, like one that investigated the influence of music on promoting patient safety during surgery—veterinary patients, that is. Kittens got spayed with little earphones on their heads. It turns out that “Adagio for Strings” may be more relaxing than AC/DC.
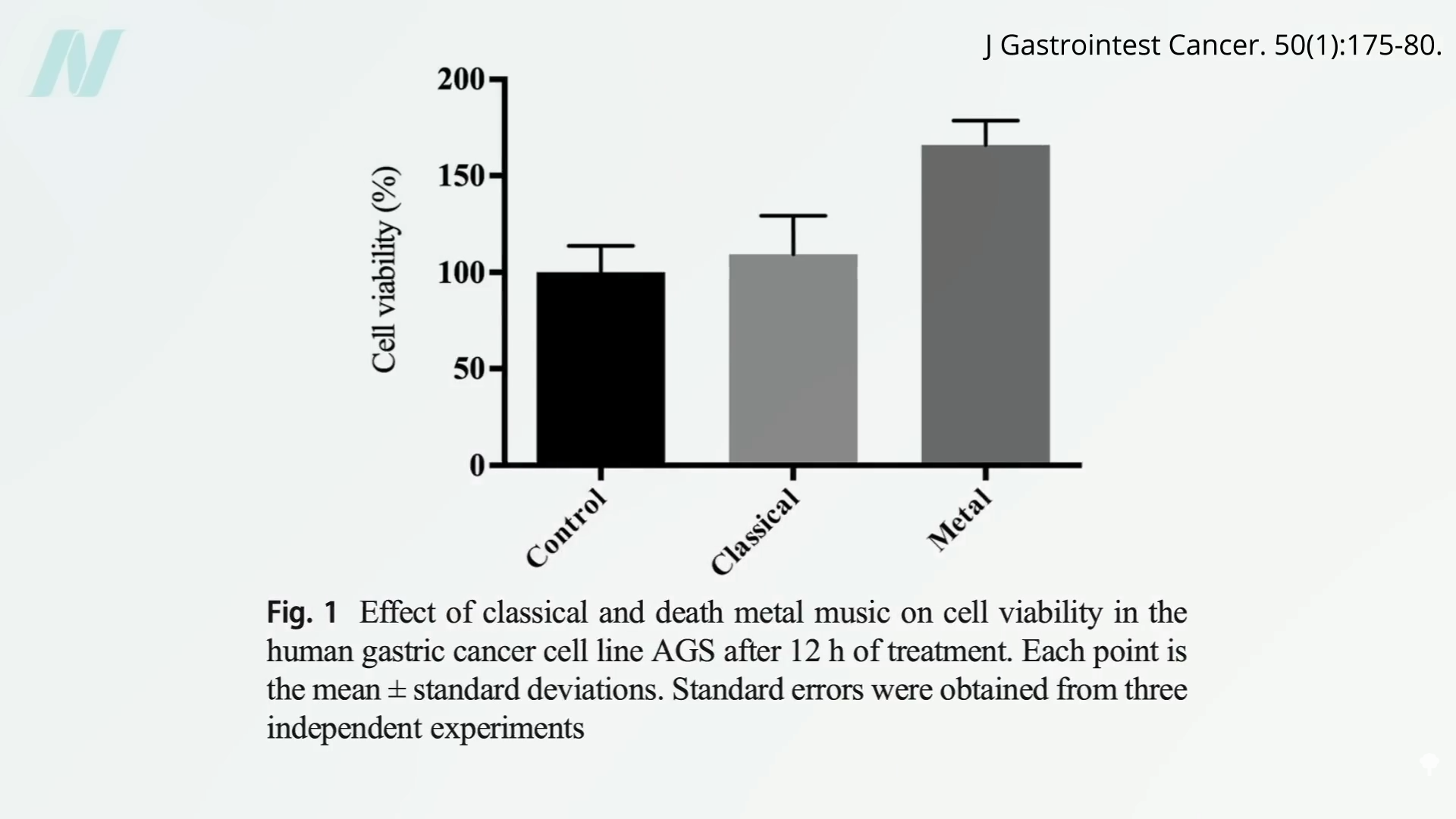
A review on music therapy for human patients warned: “Caution should be exercised…when guiding patients in selecting their music. ‘Chaotic music, such us [sic] hip-hop and metal, is not healing to human cells.’” That even had three citations, though two of them don’t say anything and the third is a nursing newsletter merely quoting someone’s opinion. I did some digging, and it turns out that stomach cancer cells like metal. If you play them Cannibal Corpse versus Beethoven, 12 hours of death metal increases their growth in a petri dish, as you can see below and at 3:28 in my video. (That’s so metal.)
But who puts headphones on their stomach? Or their chests, for that matter? In one study, Mozart killed off one type of breast cancer cell line but not another; in another study, only Beethoven’s 5th Symphony seemed to work, and Mozart flopped when the petri dishes were surrounded by speakers. How does this stuff even get published?
Anyway, the true danger from heavy metal is headbanging. “Headbanging is a contemporary dance form consisting of abrupt flexion–extension movements of the head to the rhythm of rock music, most commonly seen in the heavy metal genre.” Although the “number of avid aficionados is unknown…some fans might be endangered by indulging excessive headbanging.” Despite headbanging generally being “considered harmless,” several health complications have been attributed to this practice, including ripping your carotid artery, rupturing your lung, whiplash injury, neck fracture, or subdural hematoma. One man reported headbanging at a Motörhead concert, and all that “brisk forward and backward acceleration and deceleration forces” might have ruptured his bridging veins and caused him to bleed into his skull.
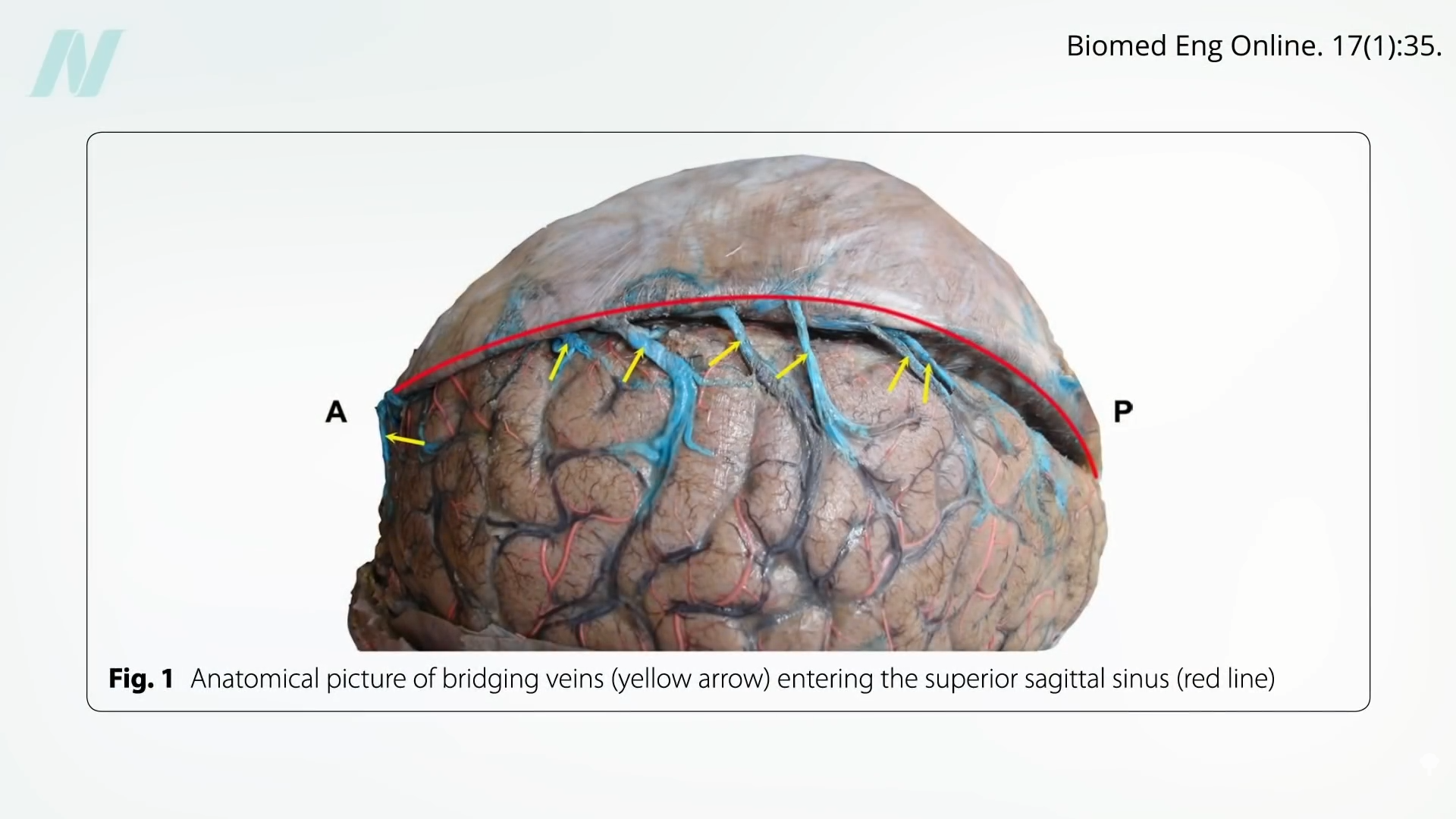
As shown here and at 4:47 in my video, bridging veins bridge the gap between the brain and the covering that lines the inside of our skull, and if the veins tear, blood can build up under our skull and compress our brain.
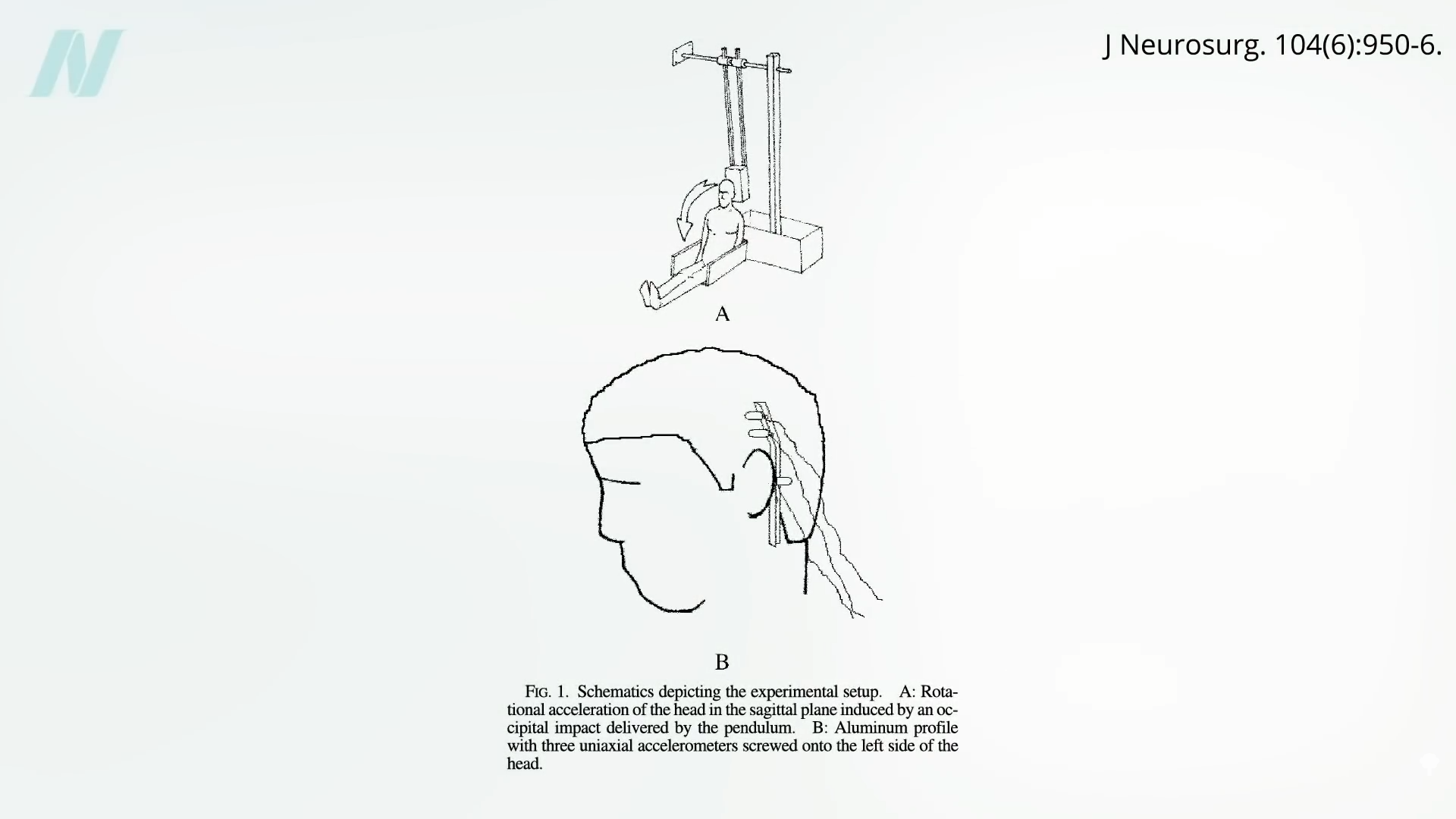
This bridging vein rupture has been demonstrated on headbanging cadavers (another very metal study). See below and at 5:02 in my video. It’s been likened to a “pseudo shaken-baby syndrome” in adults.
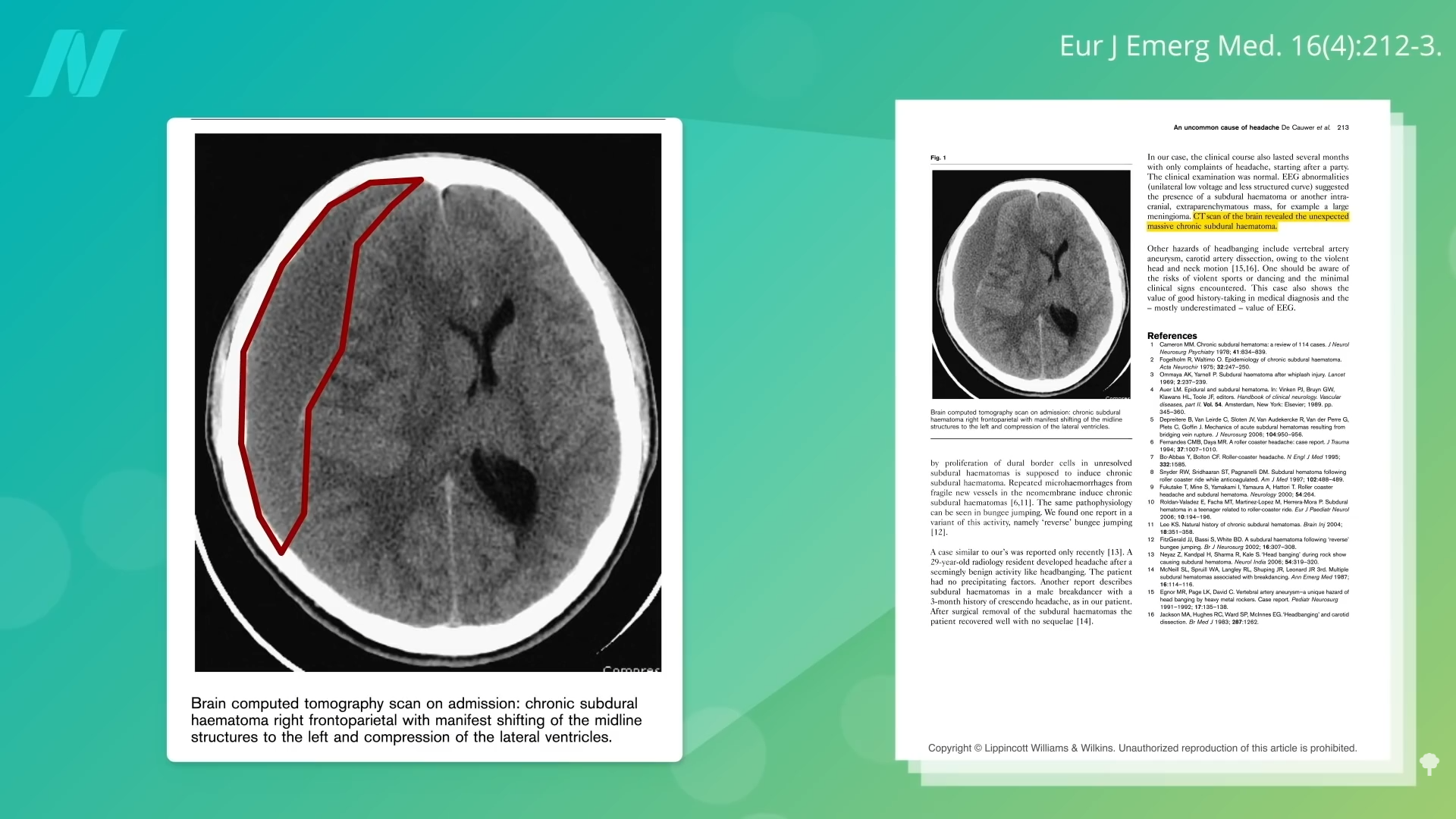
The researchers conclude that their “case serves as evidence in support of Motörhead’s reputation as one of the most hardcore rock’n’roll acts on earth,” but I think the real takeaway is that a potentially dangerous complication like subdural hematoma can result from “a seemingly benign activity like head banging.” And some of the brain bleeds can be massive. One man complained of a “headache after headbanging at a party.” Why? As you can see in his CT scan below and at 5:35, circled in red is all blood, squishing over his brain. Amazingly, he survived; another man didn’t, headbanging and losing his life to a fatal subdural hemorrhage.
We can tear more than just veins. There are two sets of arteries that tunnel into the skull—the carotid arteries in the front and the vertebral arteries in the back—and we can tear both sets. A 15-year-old boy “indulged in headbanging” and ripped his carotid artery, which led to a massive stroke. He presented as half-paralyzed and unable to speak, and he died in a coma within a week.
What about the vertebral arteries in the back? They’re wedged into our skull, rendering them susceptible to shearing forces from extremes of neck motion, and that’s exactly what appeared to happen when a heavy metal drummer tore the wall of the artery. All of this is really rare, probably afflicting less than one in a thousand or so. What can metalheads do to reduce their risk? “To prevent injury due to such head-banging, the range of head and neck motion should be reduced, slower-tempo music should replace heavy metal rock, the frequency of head-banging should be only on every second beat, or personal protective equipment should be used”—like a neck brace?
“Little formal injury research has been conducted on the worldwide phenomenon of head banging,” so researchers constructed “a theoretical head banging model” with enough physics terms to make any nerd happy: “angular displacement,” “sinusoidal motion in the sagittal plane,” and “amplitude of the displacement curve.” The study participants? Headbangers. The control group? That’s easy with easy listening music.
The head injury curves and neck injury curves, based on headbanging tempo and angular sweep, are shown below and at 7:23.
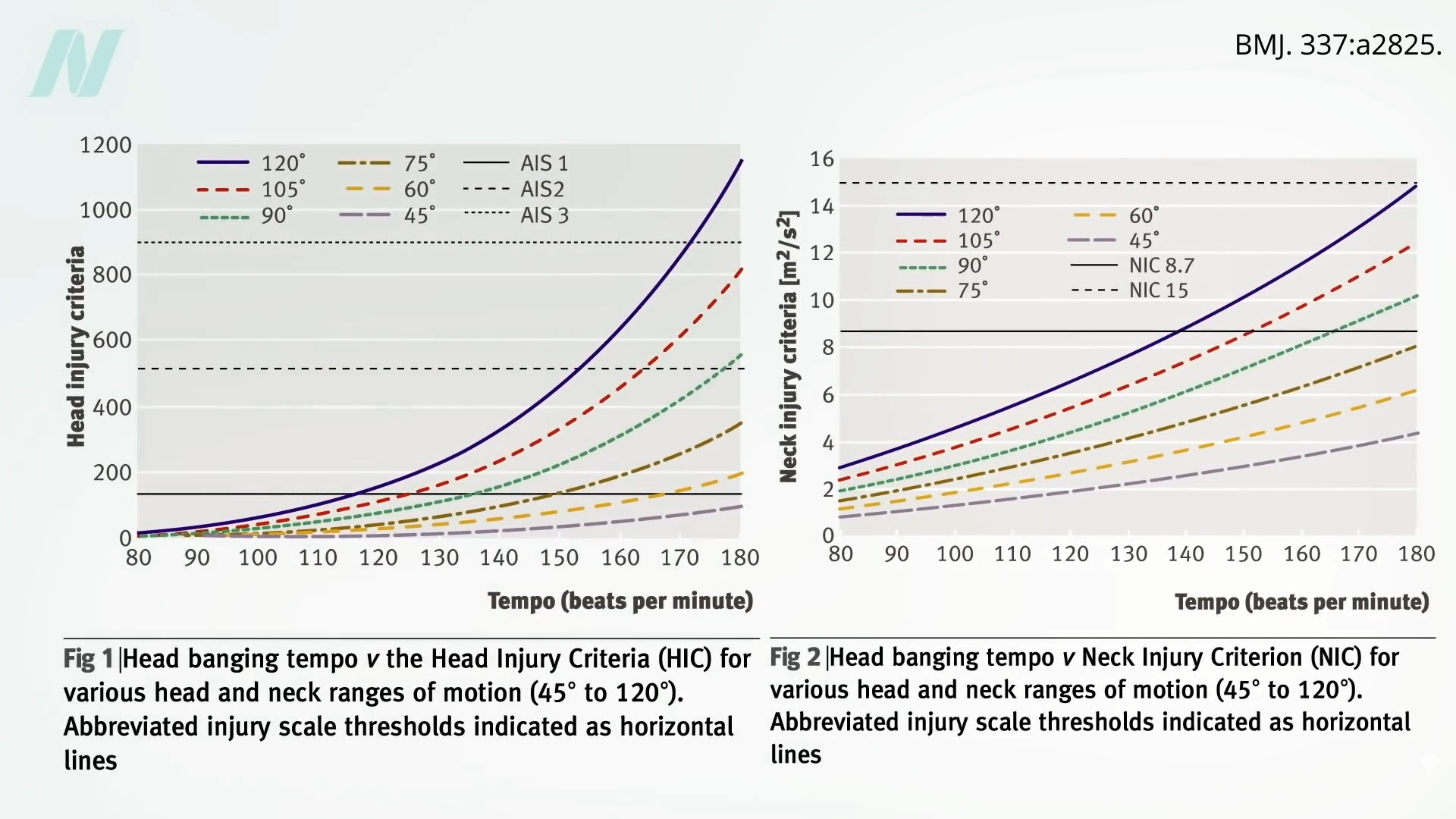
“An average head-banging song has a tempo of about 146 beats per minute, which is predicted to cause mild head injury when the range of motion is greater than 75º,” so something like what’s seen below and at 7:34 in my video.

The researchers conclude: “To minimise the risk of head and neck injury, head bangers should decrease their range of head and neck motion, head bang to slower tempo songs by replacing heavy metal with adult-oriented rock, only head bang to every second beat, or use personal protective equipment.”
“Unfortunately, it is difficult, if not impossible, to change the habits of heavy metal aficionados.” Maybe what we need are metal-studded neck braces.
Doctor’s Note
What about the healing potential of music? Check out Music as Medicine and Music for Anxiety: Mozart vs. Metal.
Michael Greger M.D. FACLM
Source link









 Medically-supervised fasting has
Medically-supervised fasting has “
“






