If anything defines America’s current obesity-drug boom, it’s this: Many more people want these injections than can actually get them. The roadblocks include exorbitant costs that can stretch beyond $1,000 a month, limited insurance coverage, and constant supply shortages. But before all of those issues come into play, anyone attempting to get a prescription will inevitably confront the same obstacle: their body mass index, or BMI.
So much depends on the simple calculation of dividing one’s weight by the square of their height. According to the FDA, people qualify for prescriptions of Wegovy and Zepbound—the obesity-drug versions of the diabetes medications Ozempic and Mounjaro—only if their BMI is 3o or higher, or 27 or higher with a weight-related health issue such as hypertension. Many who do get on the medication use BMI to track their progress. That BMI is the single biggest factor determining who gets prescribed these drugs, and who doesn’t, is the result of how deeply entrenched this metric has become in how both doctors and regular people approach health: Low BMI is good and high BMI is bad, or so most of us have come to think.
This roughly 200-year-old metric has never been more relevant—or maligned—than it is in the obesity-drug era. BMI has become like the decrepit car you keep driving because it still sort of works and is too much of a hassle to replace. Its numerous shortcomings have been called out for many years now: For starters, it accounts for only height and weight, not other, more pertinent measures such as body-fat percentage. In June, the American Medical Association formally recognized that BMI should not be used alone as a health measure. Last year, some doctors called for BMI to be retired altogether, echoing previous assertions.
The thing is, BMI can be an insightful health metric, but only when used judiciously with other factors. The problem is that it often hasn’t been. Just as obesity drugs are taking off, however, professional views are changing. People are so accustomed to seeing BMI as the “be-all, end-all” of health indicators, Kate Bauer, a nutritional-sciences professor at the University of Michigan, told me. “But that’s increasingly not the way it’s being used in clinical practice.” A shift in the medical field is a good start, but the bigger challenge will be getting everyone else to catch up.
BMI got its start in the 1830s, when a Belgian astronomer named Adolphe Quetelet attempted to determine the properties of the “average” man. Using data on primarily white people, he observed that weight tended to vary as the square of height—a calculation that came to be known as Quetelet’s index.
Over the next 150 years, what began as a descriptive tool transformed into a prescriptive one. Quetelet’s index (and other metrics like it) informed height-weight tables used by life-insurance companies to estimate risk. These sorts of tables formed “recommendations for the general population going from ‘average’ to ‘ideal’ weights,” the epidemiologist Katherine Flegal wrote in her history of BMI; eventually, nonideal weights were classified as “overweight” and “obese.” In 1972, the American physiologist Ancel Keys proposed using Quetelet’s index—which he renamed BMI—to roughly measure obesity. We’ve been stuck with BMI ever since. The metric became embedded not only in research and doctor’s visits but also in the very definitions of obesity. According to the World Health Organization, a BMI starting at 25 and less than 30 is considered overweight; anything above that range is obese.
But using BMI to categorize a person’s health was controversial from the start. Even Keys called it “scientifically indefensible” to use BMI to judge someone as overweight. BMI doesn’t account for where fat is distributed on the body; fat that builds up around organs and tissues, called visceral fat, is linked to serious medical issues, while fat under the skin—the kind you can pinch—is usually less of a problem. Muscularity is also overlooked: LeBron James, for example, would be considered overweight. Both fat distribution and muscularity can vary widely across sex, age, and ethnicity. People with high BMIs can be perfectly healthy, and “there are people with normal BMIs that are actually sick because they have too much body fat,” Angela Fitch, an assistant professor at Harvard Medical School and the president of the Obesity Medicine Association, told me.
For all its flaws, BMI is actually useful at the population level, Fitch said, and doctors can measure it quickly and cheaply. But BMI becomes troubling when it is all that doctors see. In some cases, the moment when a patient’s BMI is calculated by their doctor may shape the rest of the appointment and relationship going forward. “The default is to hyper-focus on the weight number, and I just don’t think that that’s helpful,” Tracy Richmond, a pediatrics professor at Harvard Medical School, told me. Anti-obesity bias is well documented among physicians—even some obesity specialists—and can lead them to dismiss the legitimate medical needs of people with a high BMI. In one tragic example, a patient died from cancer that went undiagnosed because her doctors attributed her health issues to her high BMI.
But after many decades, the medical community has begun to use BMI in a different way. “More and more clinicians are realizing that there are people who can be quite healthy with a high BMI,” Kate Bauer said. The shift has been gradual, though it was given a boost by the AMA policy update earlier this year: “Hopefully that will help clinicians make a change to supplement BMI with other measures,” Aayush Visaria, an internal-medicine resident at Rutgers Robert Wood Johnson Medical School who researches BMI’s shortcomings, told me.
Physicians I spoke with acknowledged BMI’s flaws but didn’t seem too concerned about its continued use in medicine—even as obesity drugs make this metric even more consequential. BMI isn’t a problem, they said, as long as physicians consider other factors when diagnosing obesity or prescribing drugs to treat it. If you go to a doctor with the intention of getting on an obesity drug, you should be subject to a comprehensive evaluation including metrics such as blood sugar, cholesterol levels, and body composition that go “way beyond BMI,” Katherine Saunders, a clinical-medicine professor at Weill Cornell Medicine, said. Because Wegovy and other drugs come with side effects, she told me, doctors must be absolutely sure that a patient actually needs them, she added.
But BMI isn’t like most other health metrics. Because of its simplicity, it has seeped out of doctor’s offices and into the mainstream, where this more nuanced view still isn’t common. Whether we realize it or not, BMI is central to our basic idea of health, affecting nearly every aspect of daily life. Insurance companies are notorious for charging higher rates to people with high BMI and lowering premiums for people who commit to long-term weight loss. Fertility treatments and orthopedic and gender-affirming surgery can be withheld from patients until they hit BMI targets. Workplace wellness programs based on BMI are designed to help employees manage their weight. BMI has even been used to prevent prospective parents from adopting a child.
The rise of obesity drugs may make these kinds of usages of BMI even harder to shake. Determining drug eligibility by high BMI supports the notion that a number is synonymous with illness. Certainly many people using obesity drugs take a holistic view of their health, as doctors are learning to do. But focusing on BMI is still common. Some members of the r/Ozempic Subreddit, for example, share their BMI to show their progress on the drug. Again, high BMI can be used to predict who has obesity, but it isn’t itself an obesity diagnosis. The problem with BMI’s continued dominance is that it makes it even harder to move away from simply associating a number on a scale with overall health, with all the downstream consequences that come along with a weight-obsessed culture. As obesity drugs are becoming mainstream, “there needs to be public education explaining that BMI by itself may not be a good indicator of health,” Visaria said.
In another 200 years, surely BMI will finally be supplanted by something else. If not much sooner: A large effort to establish hard biological criteria for obesity is under way; the goal is to eliminate BMI-based definitions once and for all. Caroline Apovian, a professor at Harvard Medical School, gives it “at least 10 years” before a comparably cheap or convenient replacement arises—though any changes would take longer to filter into public consciousness.” Until that happens, we’re stuck with BMI, and the mess it has wrought.



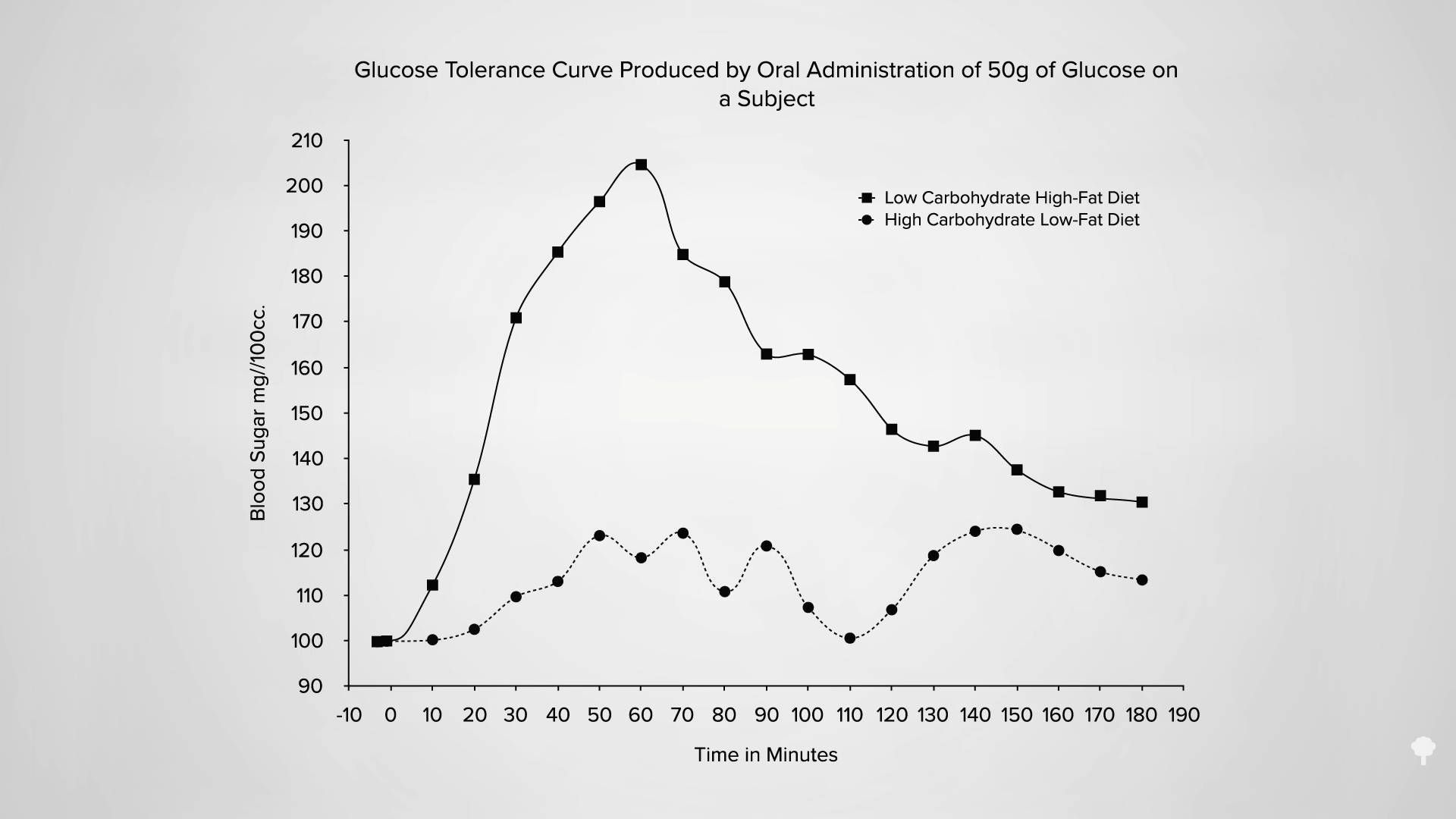
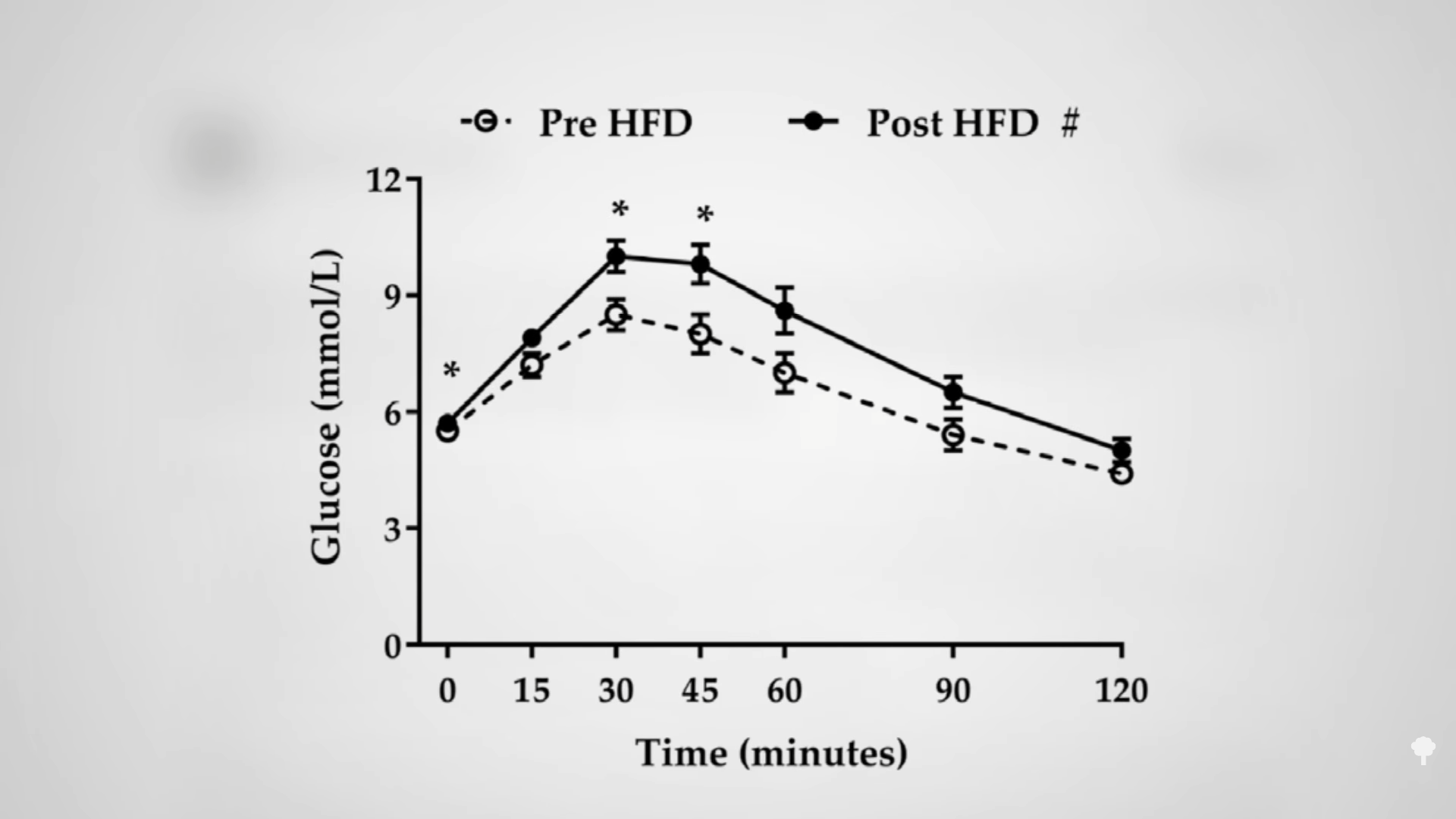
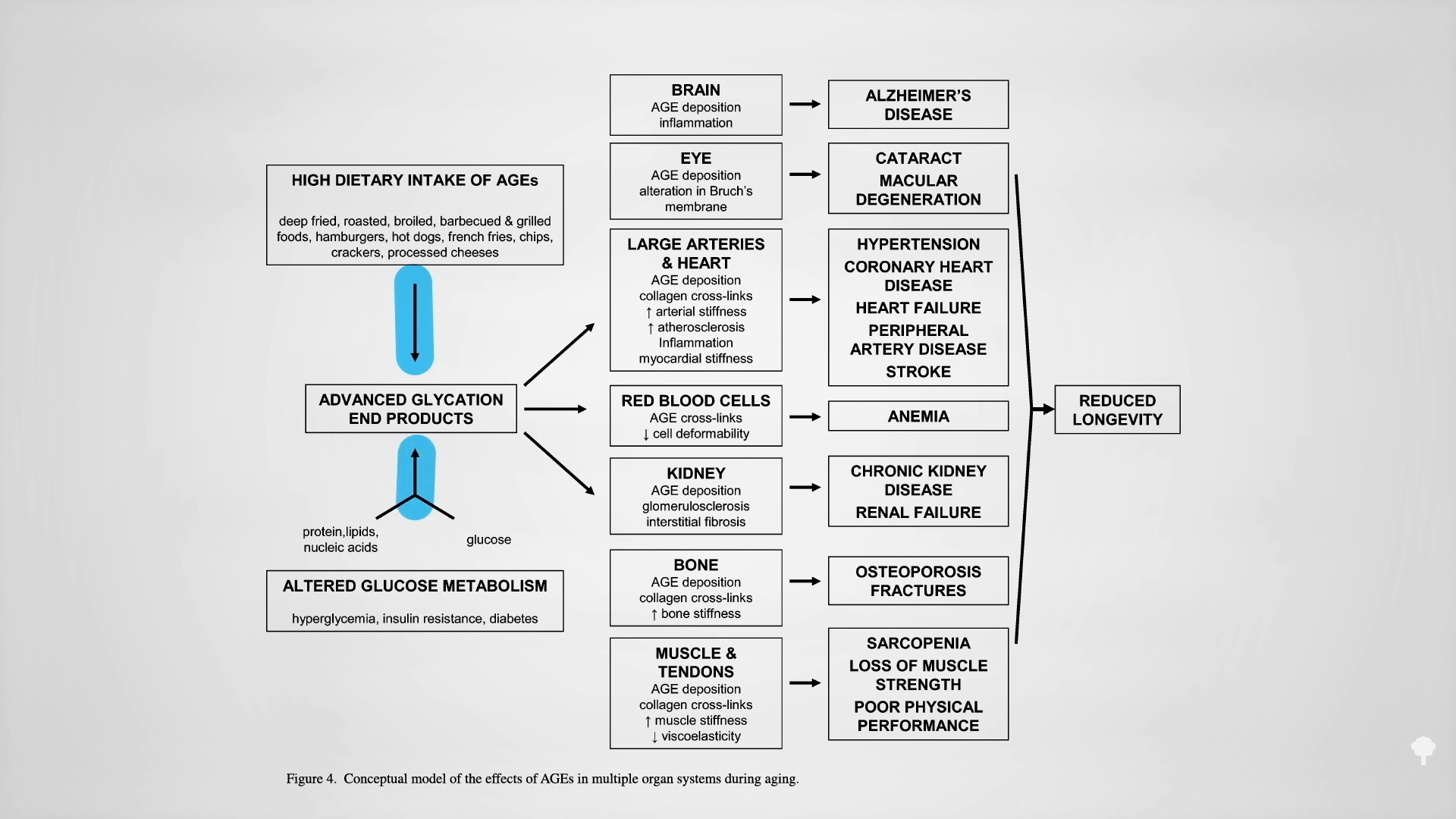
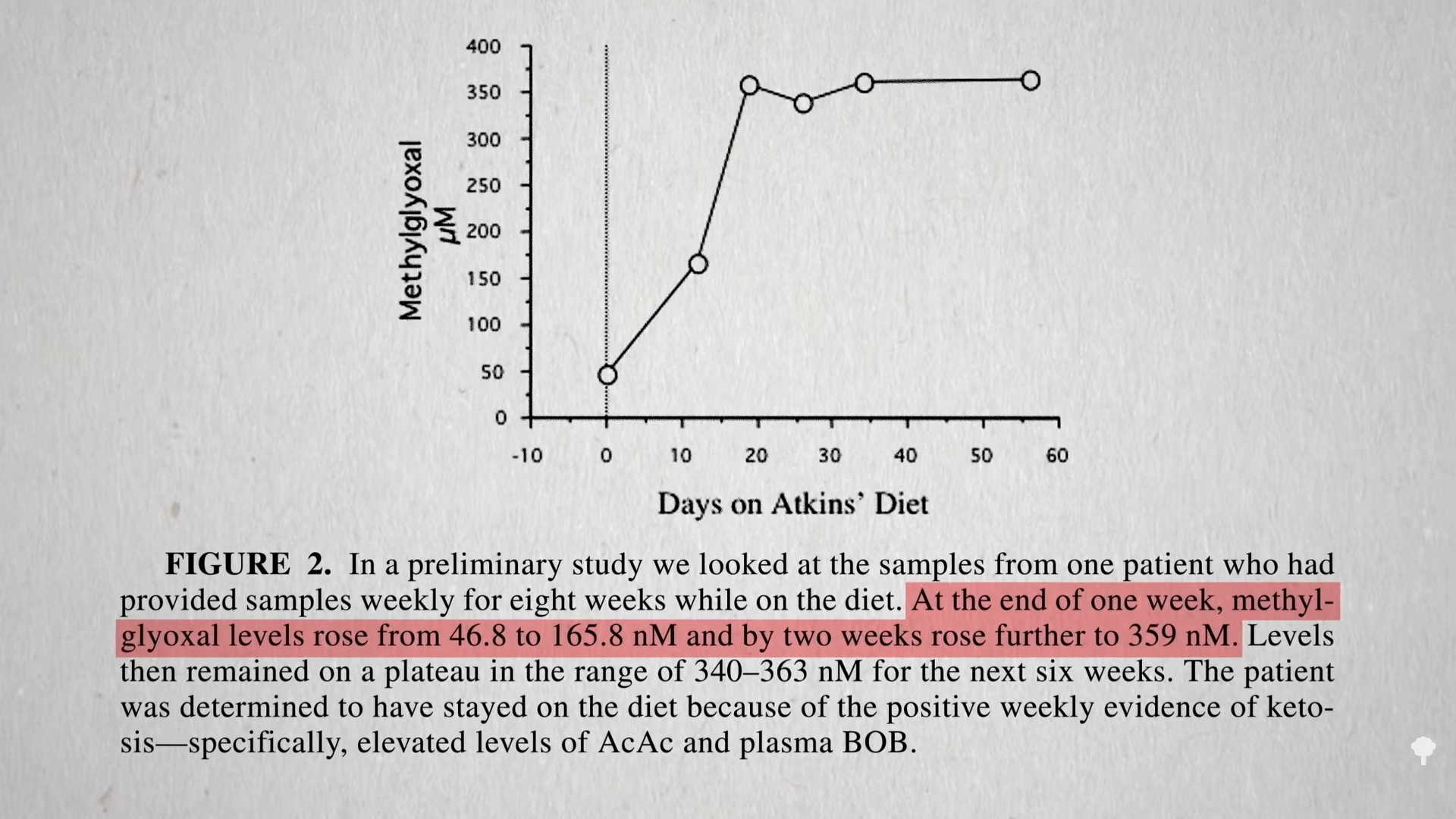
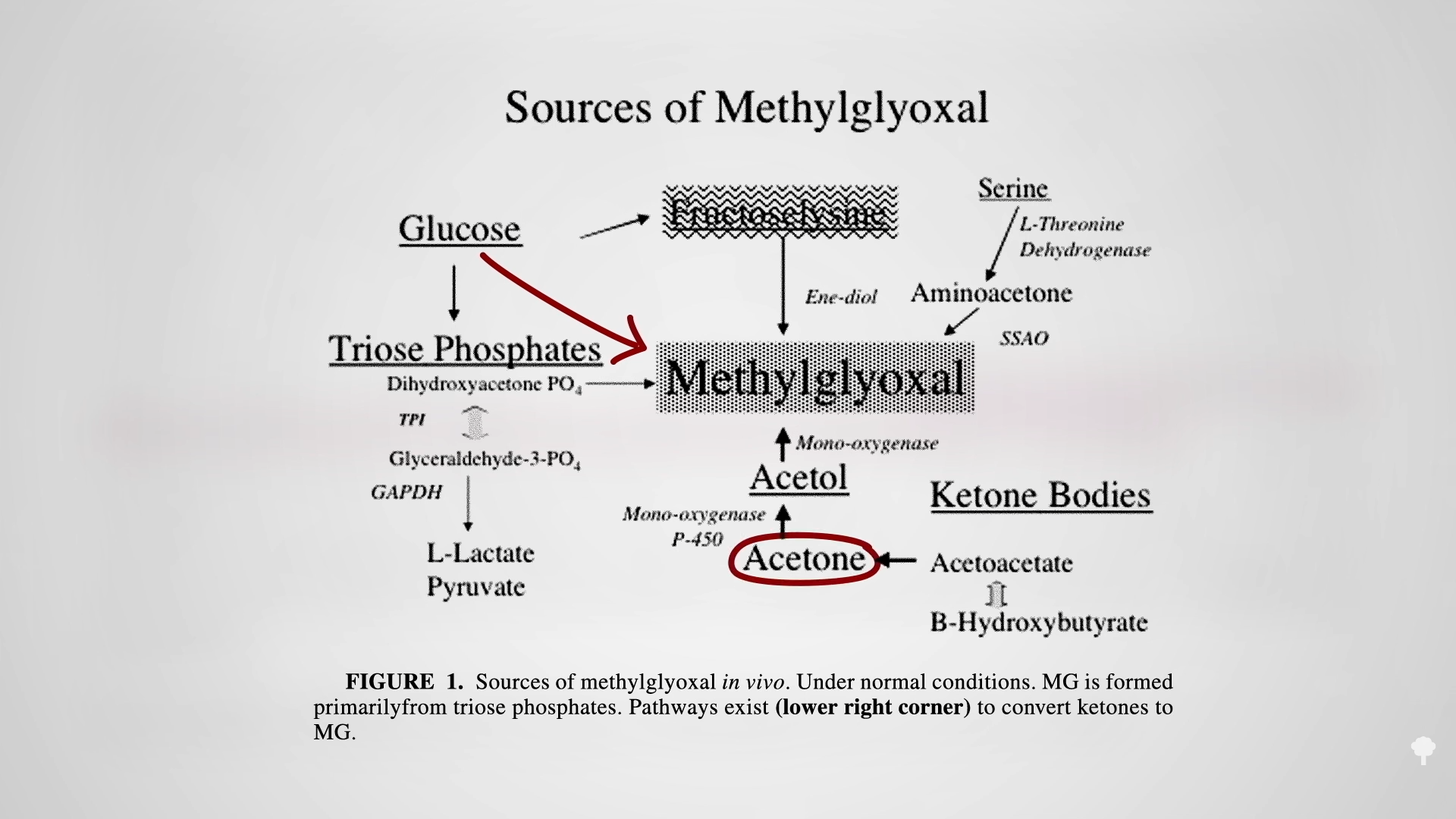
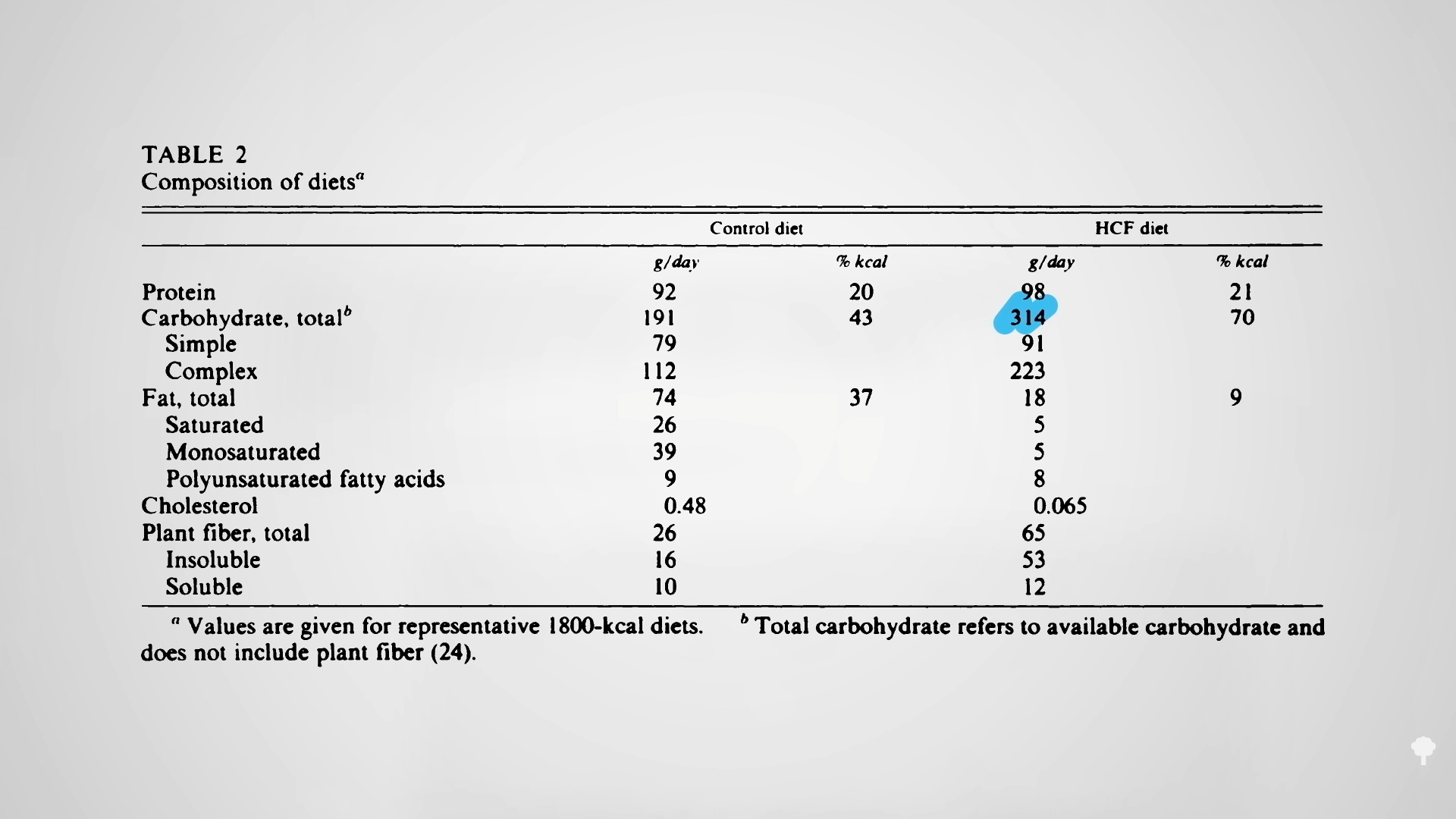 The irony doesn’t stop there. One of the reasons people with diabetes suffer such nerve and artery damage is due to an inflammatory metabolic toxin known as methylglyoxal, which forms at high blood sugar levels. Methylglyoxal
The irony doesn’t stop there. One of the reasons people with diabetes suffer such nerve and artery damage is due to an inflammatory metabolic toxin known as methylglyoxal, which forms at high blood sugar levels. Methylglyoxal