[ad_1]
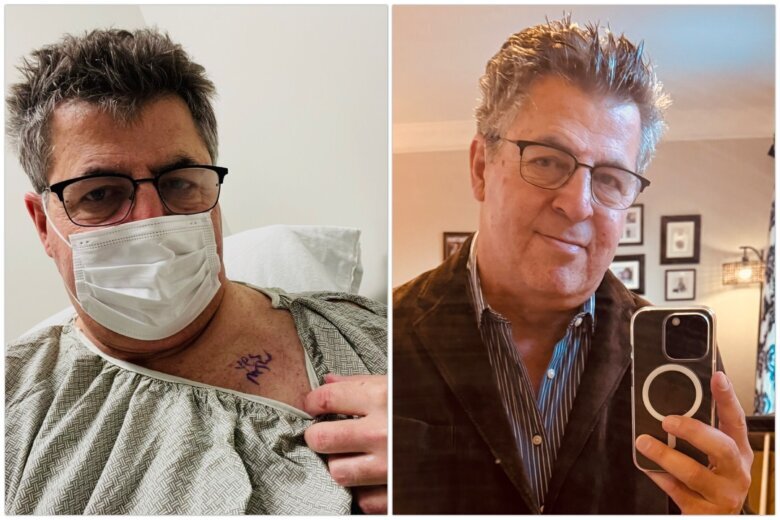
During the first three years of Augenstein’s lung cancer journey, he’s been happy to be able to share things he has been learning along the way.
In my first 25 years at WTOP, my reports about lung cancer were primarily stories about famous people who died from the deadliest and second-most common cancer in the U.S. — until I was diagnosed with Stage 4 lung cancer exactly three years ago.
Since then, most of my lung cancer stories have been about living.
Within six months of being diagnosed with Stage 4 non-small cell lung cancer just before Thanksgiving 2022, after great results with one-pill-a-day targeted therapy that shrank cancerous tumors and lymph nodes in both lungs, I became eligible for a robotic-assisted lung lobectomy.
Since then, I’ve had no evidence of disease, and have remained cancer-free since May 2023, while continuing to take my daily pill.
Giving thanks? Indeed.
During the first three years of my journey, I’ve been happy to be able to share things I’ve been learning along the way.
First, is the importance of newly diagnosed cancer patients getting biomarker testing, and waiting for the results before beginning treatment.
Biomarker testing involves testing biopsied lung tissue — often taken during a bronchoscopy — to try to learn the exact cell mutation that caused a patient’s cancer.
“The importance of testing is if they have that mutation, then the treatment is very different, and the patient outcomes are also much better,” thoracic medical oncologist Ram Subramanian with Inova Schar Cancer Institute in Fairfax County, Virginia, told me.
In my case, I was diagnosed with EGFR-positive lung cancer, which has several targeted treatments available, and generally limits the side effects of treatment compared to chemotherapy.
Despite having no evidence of cancer now, I (and my doctors) wouldn’t say that I’m “cured,” since I was originally diagnosed after cancer had spread from the original site in my left lung.
In 2025, life with lung cancer can be similar to life with other chronic diseases, including diabetes or heart disease.
The key is aggressive surveillance, which in my case involves low-dose CT scans every four months, as well as brain MRIs and liquid biopsies twice a year. If something suspicious were to show up on one of these scans, it would likely be early-stage, which could be removed with surgery or targeted by radiation.
“No evidence of intracranial metastasis” — good news in my twice-yearly brain MRI as part of aggressive surveillance, since I’ve been cancer-free for two years after dx of stage 4 #lungcancer. (Admit I had to ask whether gown ties in front or back) pic.twitter.com/uJSbaAH0gv
— Neal Augenstein (@AugensteinWTOP) July 11, 2025
And, while the American Lung Association’s 2025 State of Lung Cancer report shows the five-year survival rate for lung cancer in the U.S. has risen to 29.7%, which represents a 26% improvement over the past five years, research continues to enable earlier detection, including the use of artificial intelligence.
Lung cancer patients in the D.C. region are lucky — there are a large number of clinical trials in Virginia, Maryland and the District, offering new options and hope for patients and their families.
Personally, while I’ve been lucky to not have any recurrences in my first three years living with cancer, I often discuss trials with my thoracic oncologist Amin Benyounes, who is the co-leader at the Inova Schar Cancer Institute’s Phase One Program.
Benyounes said many patients considering enrollment in a clinical trial worry about the unknown: “Will this make me feel worse, will it make me feel sick, could it hurt more than it would help? Will my kids or my partner have to bear the burden of me feeling sick?”
With clinical trials affording the possibilities for longer survival with fewer side effects, some patients ask, “What if I get my hopes up, and it doesn’t work?”
According to Benyounes: “My answer to that is usually, ‘We have to take things one step at a time.’”
That’s the same guidance he gave me when I began my cancer journey, three years ago.
Get breaking news and daily headlines delivered to your email inbox by signing up here.
© 2025 WTOP. All Rights Reserved. This website is not intended for users located within the European Economic Area.
[ad_2]
Neal Augenstein
Source link