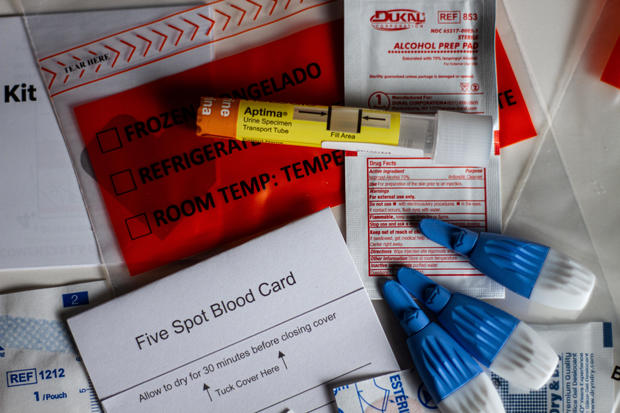
Everything You Need to Know About Getting Tested for STIs
We treat sexually transmitted infections differently from other infections. If your friend has a cold, you say, “Oh, that sucks,” not, “Gross, you should have been more careful!”
If there’s a virus going around, you get a pamphlet explaining what it is and how not to catch it — not shamed for being unclean. Rather than waiting until they’re teenagers and telling them not to hang out with certain people, we vaccinate children to keep them safe from certain diseases.
But in many people’s minds, sexually transmitted infections — STIs for short, and formerly known as STDs — are different. Unfortunately, because of their association with sex, they’re often seen as much scarier and more shameful.
RELATED: Here’s How Not to Get an STI
As a result, people tend to approach their sexual health in backwards or unproductive ways by being blissfully ignorant until it’s too late. That said, protecting yourself from STIs isn’t super complex, and unlike other infections, there are cheap and easy ways to find out if you’re affected.
AskMen spoke with a handful of sexual health experts to get the info on what you need to know about STI tests, from how they work to why they’re important to why guys often tend to avoid taking them.
What Is an STI Test?
“A STI test is done to check if you have a sexually transmitted infection, such as chlamydia, trichomoniasis, gonorrhea, HPV, HIV, herpes, or syphilis,” says Dr. Janet Brito, a sex therapist based in Hawaii.
However, not all tests are the same. Depending on what you’re getting tested for, with many tests checking for multiple infections at once, the test may take a different form. Common ways to check for STIs are “via a blood sample, a swab, or a urine analysis,” adds Brito.
Why Getting Tested Is Important
If you’ve never been tested before, you might not be entirely clear on why getting tested fairly regularly is important.
“If you are sexually active, especially if you are engaging in unprotected sexual activity, participating in high risk sexual behavior (i.e have multiple partners), starting a new relationship, noticing any symptoms (i.e. foul discharge, burning during urination, bumps, or sores around or on genital area, pain, itching, inflammation), it is best to get a STI test to rule out any possible infections and to avoid any health complications that may arise and that could be treated early on,” says Brito.
“It is also important to get tested even when you do not have symptoms,” she adds, “as some STIs may be asymptomatic” — meaning you might not see the signs until you’ve already passed it on to someone else — or worse, multiple people.
Beyond just treating symptoms as to also avoid infecting other people, knowing your STI status is important to ensure your STI doesn’t develop into something worse if untreated.
“It is important to discuss your sexual health practices with your doctor, especially if you are engaging in anal sex,” notes Brito. “An anal pap smear can help to screen for HPV as well. Not receiving proper care for STI symptoms may result in more complicated health challenges, like infertility or cancer.”
How Often You Should Get Tested
As for how often you should get tested, there’s no one single answer.
It becomes more important in certain specific circumstances, particularly if you notice potential symptoms, and/or when you’re about to start sleeping with a new partner.
“The CDC guidelines about how often to get tested are ambiguous because there’s no magic bullet,” explains Lauren Weiniger, cofounder of an app called SAFE, which allows users to privately show their verified STI status on their phone and get tested. “It depends on your lifestyle, and your risk tolerance. The guidelines vary from three to six months, but some people choose to get tested every two weeks.”
Why Some Guys Avoid Getting Tested
However, if you’re most guys — particularly straight guys, who often have fewer partners than their queer counterparts — you’re most likely not getting tested every two weeks.
You might not be getting tested every three to six months, either. In fact, some guys have never gotten tested, regardless of their sexual history. There are a few reasons why that might be the case.
“Some guys may not get tested because they do not know to get tested (i.e. do not have enough comprehensive sex education around the benefits of getting tested),” says Brito. They could also skip getting tested because they “don’t have any symptoms that they are aware of.”
Perhaps the most pressing issue, however? Guys avoiding getting tested “due to stigma and shame around sexuality and the issue of STIs,” as Brito puts it. “This worry may prevent guys from getting tested and seeking help.”
In order to help combat that, demystifying STI tests could be useful — so keep reading to find out what they’re like, how they work and how to get one done.
The Different Kinds of STI Tests, Explained
While it might be convenient to take a test that checks for all the different STIs at once, no such test exists (not yet, at least).
In countries with universal healthcare like Canada, the United Kingdom, Australia and others, syphilis tests are typically covered in whole or in large part.
However, in the United States, you might need private insurance in order to pay for an STI test, and depending on which insurance you have and where you go to get tested, your STI test may or may not be covered. If you’re unsure, it’s best to look into it before showing up.
That being said, here’s a breakdown of some common STIs and what it’s like to get tested for them:
Chlamydia
Chlamydia is a bacterial infection that typically presents no symptoms. However, when it does, the results are not pleasant.
RELATED: How to Diagnose and Treat Chlamydia
Men who come down with chlamydia symptoms often experience burning sensations when they urinate, testicle pain, scrotum swelling and even discharge a secretion from the penis.
Luckily, once it’s diagnosed, it’s easily treatable with antibiotics.
How the Chlamydia Test Works
The test for chlamydia is typically an analysis of either a urine sample or a swab of the genital area.
How Long It Takes to Get Results
A standard amount of time to get results back for a chlamydia test is 7 to 10 days. Often, clinics will only contact you if you test positive — meaning if you don’t hear back, you’re in the clear.
Gonorrhea
Like chlamydia, most people with gonorrhea won’t experience symptoms. However, when those symptoms do occur, they include burning sensations, sensitive or broken skin on the genitals and a milky-white discharge of pus.
RELATED: How to Diagnose and Treat Gonorrhea
Yes, the infection is so named because gonorrhea means “flow of seed” in ancient Greek — doctors at the time mistook the discharge for semen.
Gonorrhea is also treated with antibiotics, but over time, some strains of the infection have become increasingly resistant to the drugs. It’s led to a version called “super gonorrhea,” which is more difficult, but not impossible, to cure.
How the Gonorrhea Test Works
Like the chlamydia test, the test for gonorrhea is an analysis of either a urine sample or a swab of the genital area.
How Long It Takes to Get Results
Like chlamydia, gonorrhea tests typically take 7 to 10 days to hear back, and again, if you test negative, you may not be contacted at all.
HIV
HIV (human immunodeficiency virus) is the most serious disease that’s sexually transmitted, as it can morph into AIDS, a disease that has historically been quite deadly.
Although recent medical advances, such as the development of PReP treatments, have made HIV much less likely to have fatal consequences, knowing your HIV status is still of paramount importance.
How the HIV Test Works
HIV tests are done on a blood sample, meaning either a syringe will be used to draw some blood from your arm, or a finger prick will be performed.
How Long It Takes to Get Results
Some centers offer rapid HIV test results, where you can discover your result in a matter of minutes. However, taking a normal HIV test could mean it’ll take days to weeks to get results.
Herpes
There are two different types of herpes: HSV-1 and HSV-2, which can both produce sores around the mouth and genitals — sores that themselves are infectious.
RELATED: How to Diagnose and Treat Genital Herpes
Herpes can also leave you with a rash in the genital region, as well as an unpleasant fever. T at the moment, but it can be treated using antiviral medications. If left untreated, however, herpes can have serious effects on various other parts of the body, so taking it seriously is hugely important.
How the Herpes Test Works
The test for herpes differs depending on whether you’re presenting symptoms or not. If no symptoms are present, a blood test is done. If there are symptoms, in addition to the blood test, you’ll get a swab of the affected area done.
How Long It Takes to Get Results
Depending on the type of test, it can take between 1 and 14 days to get results from a herpes test.
Syphilis
Syphilis is a bacterial infection that can have devastating health consequences if left untreated.
After the first stage — painless sores appear on or around the genitals but then recede — people with syphilis will begin experiencing an infectious skin rash, intense cold symptoms and even hair loss.
RELATED: How to Diagnose and Treat Syphilis
If it’s still left untreated, the third stage of syphilis involves the disease spreading to various other parts of the body, including the brain, where it can cause serious and wide-ranging damage. However, if syphilis is treated before it begins to progress to the second stage, it’s relatively easy to cure, often requiring just a single shot of penicillin.
How the Syphilis Test Works
A syphilis test is done using either a blood sample or a sample of fluid from a syphilis sore, if symptoms are present.
How Long It Takes to Get Results
Getting your syphilis test results back can take between three and five days.
HPV
HPV, which stands for human papillomavirus, is a very common virus; nearly 80 million people are currently infected in the United States. In fact, HPV is so common that nearly all men and women get it at some point in their lives.
Most of the time, the virus goes away on its own, but some strains of HPV can lead to cervical cancer if not found and treated.
“You could possibly be carrying a cancer-causing strain without knowing it,” says Engle. “There isn’t much you can do other than use condoms and be aware and educated about sexual health and wellness.”
How the HPV Test Works
There’s currently no test for men who are HPV-positive and don’t show symptoms (which is the vast majority of men).
How Long It Takes to Get Results
With no current test for men, there’s no way of knowing. However, if a female partner you’ve had unprotected sex with gets tested for HPV — a fairly good marker of whether you have it — that would take one to three weeks.
How to Find Out Your STI Status
Finding a Nearby Testing Location
Going into an urgent care without insurance can leave you with a bill of over $1,000. That’s why it’s necessary to find sexual health clinics that offer free care to individuals without insurance or accept insurance with a little to zero copay.
“The best advice I can give is to Google local free clinics in the area and always check for the closest Planned Parenthood,” says Gigi Engle, a certified sex coach and clinical sexologist.
(If you live in the United States, you can head on over to the Planned Parenthood locator to find the nearest location to you.)
“At a free clinic you can expect to be seen by a nurse practitioner. They’ll take a blood sample and test for HIV, chlamydia, gonorrhea, and sometimes Hepatitis B. They don’t test for herpes unless they expect an infection, meaning that you’re having an outbreak.”
RELATED: Conversations to Have With Your Doctor
“You can also talk to your primary care physician, and don’t be afraid to tell them what’s going on. If you feel like you can’t comfortably discuss medical issues with your doctor, find a new one. You should always feel safe,” Engle added.
The Safe app is yet another option. The app privately shows your verified STI status on your phone, and also links users to testing centers. “With the app, you can skip the doctor and book testing directly at over 30,000 labs across the U.S., usually the same day and in under 15 minutes. It’s only $99 out of pocket, or you can use your insurance to cover the cost,” says Weiniger.
Using At-Home STI Test Kits
If you’re in a situation where going to a nearby clinic isn’t a convenient, feasible or available option, you can also make use of the burgeoning at-home STI test kit industry.
As with so many industries today, STI tests are something you can have delivered to your front door — but are they as good as getting tested by a professional? At least for the time being, probably not, in part because the method at-home kits use (urine analysis) isn’t the most accurate when compared to getting your blood work done.
As well, if you’re already experiencing STI symptoms, you should speak with a doctor about them anyway, so taking an at-home test might not be the most useful approach.
That being said, if you’re symptom-free, not engaging in high-risk sexual behavior and just want a quick, relatively accurate checkup, an at-home STI test kit isn’t a terrible idea.
To find out the best at-home STI test kit for you, you can check out AskMen’s list of them below:
RELATED: The Best Proven At-Home STI Test Kits
When to Get an STI Test Done
1. If You Don’t Plan on Using Condoms With Your Partner
After a period of dating, it’s not that uncommon for those in a monogamous relationship to decide that condoms aren’t necessary anymore. Prior to having unprotected sex, it’s highly recommended to get tested to ensure that both you and your partner are negative for all STIs — even if you feel completely healthy.
“Many STIs have a latency period,” warns Weiniger. Meaning, it can take as long as six weeks following intercourse to show up positive for a sexually transmitted infection such as syphilis. “An STI test is a snapshot in time, so while someone may have tested negative a few weeks ago, there’s no guarantee they haven’t been exposed or they weren’t already exposed since that test was valid.”
That’s why it’s recommended to continue using protection for two months following the last time you had sex with another person. After eight weeks, the tests for all STIs will be the most accurate.
2. If You or Your Partner Notice Any Physical Changes
If you start to see some unsightly sores, experience pain urinating, or begin releasing discharge, it’s definitely time to get tested.
RELATED: What You Should Know About Penis Health Care
Flu-like symptoms, including a high fever and swollen lymph nodes, could also indicate that you recently contracted a virus (possibly HIV or herpes). If you’re experiencing any of these symptoms, you should stop having sex and wait until your results return before having intercourse again.
While men are significantly more likely than women to show symptoms after acquiring an STI, “STIs can be asymptotic and not just in women,” clarifies Ben Davis, MD, an attending physician at Massachusetts General Hospital’s Sexual Health Clinic.
He adds, “Men are commonly asymptotic in the throat and rectum,” which is why it’s necessary for men, especially men who have sex with other men, to have both oral and rectal swabs completed when tested.
3. If One of You Has Cheated
If either of you are having unprotected sex with someone outside of the relationship, getting tested is important — even if you didn’t go “all the way.” Gonorrhea, chlamydia, and HSV-2 (genital herpes) can still be passed if oral sex is performed.
Even if you used a condom when you cheated, it still might be a good idea to go in a get tested, just in case.
RELATED: Everything You Should Know About Cheating
“Since condoms do prevent most STIs, I’m not sure I agree that routine STI testing is indicated after sex with condoms [after cheating],” Davis says.
“On the other hand, penetrative intercourse is not the only way to get STIs. You can get it from oral, including rimming. Also, STIs can be spread by skin to skin — HPV and HSV, to name two common ones. So I’d have to say I probably agree it’s a good idea to get tested after cheating with a condom, but I want to strongly make the point that condoms do protect against most STIs.”
with additional reporting by Zachary Zane
You Might Also Dig: