[ad_1]
Ketogenic diets have been found to undermine exercise efforts and lead to muscle shrinkage and bone loss.
An official International Society of Sports Nutrition position paper covering keto diets notes the “ergolytic effect” of keto diets on both high- and low-intensity workouts. Ergolytic is the opposite of ergogenic. Ergogenic means performance-boosting, whereas ergolytic means performance-impairing.
For nonathletes, ketosis may also undermine exercise efforts. Ketosis was correlated with increased feelings of “perceived exercise effort” and “also significantly correlated to feelings of ‘fatigue’ and to ‘total mood disturbance,’” during physical activity. “Together, these data suggest that the ability and desire to maintain sustained exercise might be adversely impacted in individuals adhering to ketogenic diets for weight loss.”
You may recall that I’ve previously discussed that shrinkage of measured muscle mass among CrossFit trainees has been reported. So, a ketogenic diet may not just blunt the performance of endurance athletes, but their strength training as well. As I discuss in my video Keto Diets: Muscle Growth and Bone Density, study participants performed eight weeks of the battery of standard upper and lower body training protocols, like bench presses, pull-ups, squats, and deadlifts, and there was no surprise. You boost muscle mass—unless you’re on a keto diet, in which case there was no significant change in muscle mass after all that effort. Those randomized to a non-ketogenic diet added about three pounds of muscle mass, whereas the same amount of weight lifting on the keto diet tended to subtract muscle mass by about 3.5 ounces on average. How else could you do eight weeks of weight training and not gain a single ounce of muscle on a ketogenic diet? Even keto diet advocates call bodybuilding on a ketogenic diet an “oxymoron.”
What about bone loss? Sadly, bone fractures are one of the side effects that disproportionately plague children placed on ketogenic diets, along with slowed growth and kidney stones. Ketogenic diets may cause a steady rate of bone loss as measured in the spine, presumed to be because ketones are acidic, so keto diets can put people in what’s called a “chronic acidotic state.”
Some of the case reports of children on keto diets are truly heart-wrenching. One nine-year-old girl seemed to get it all, including osteoporosis, bone fractures, and kidney stones, then she got pancreatitis and died. Pancreatitis can be triggered by having too much fat in your blood. As you can see in the graph below and at 2:48 in my video, a single high-fat meal can cause a quintupling of the spike in triglycerides in your bloodstream within hours of consumption, which can put you at risk for inflammation of the pancreas.
The young girl had a rare genetic disorder called glucose transporter deficiency syndrome. She was born with a defect in ferrying blood sugar into her brain. That can result in daily seizures starting in infancy, but a ketogenic diet can be used as a way to sneak fuel into the brain, which makes a keto diet a godsend for the 1 in 90,000 families stricken with this disorder.
As with anything in medicine, it’s all about risks versus benefits. As many as 30 percent of patients with epilepsy don’t respond to anti-seizure drugs. Unfortunately, the alternatives aren’t pretty and can include brain surgery that implants deep electrodes through the skull or even removes a lobe of your brain. This can obviously lead to serious side effects, but so can having seizures every day. If a ketogenic diet can help with seizures, the pros can far outweigh the cons. For those just choosing a diet to lose weight, though, the cost-benefit analysis would really seem to go the other way. Thankfully, you don’t need to mortgage your long-term health for short-term weight loss. We can get the best of both worlds by choosing a healthy diet, as I discussed in my video Flashback Friday: The Weight Loss Program That Got Better with Time.
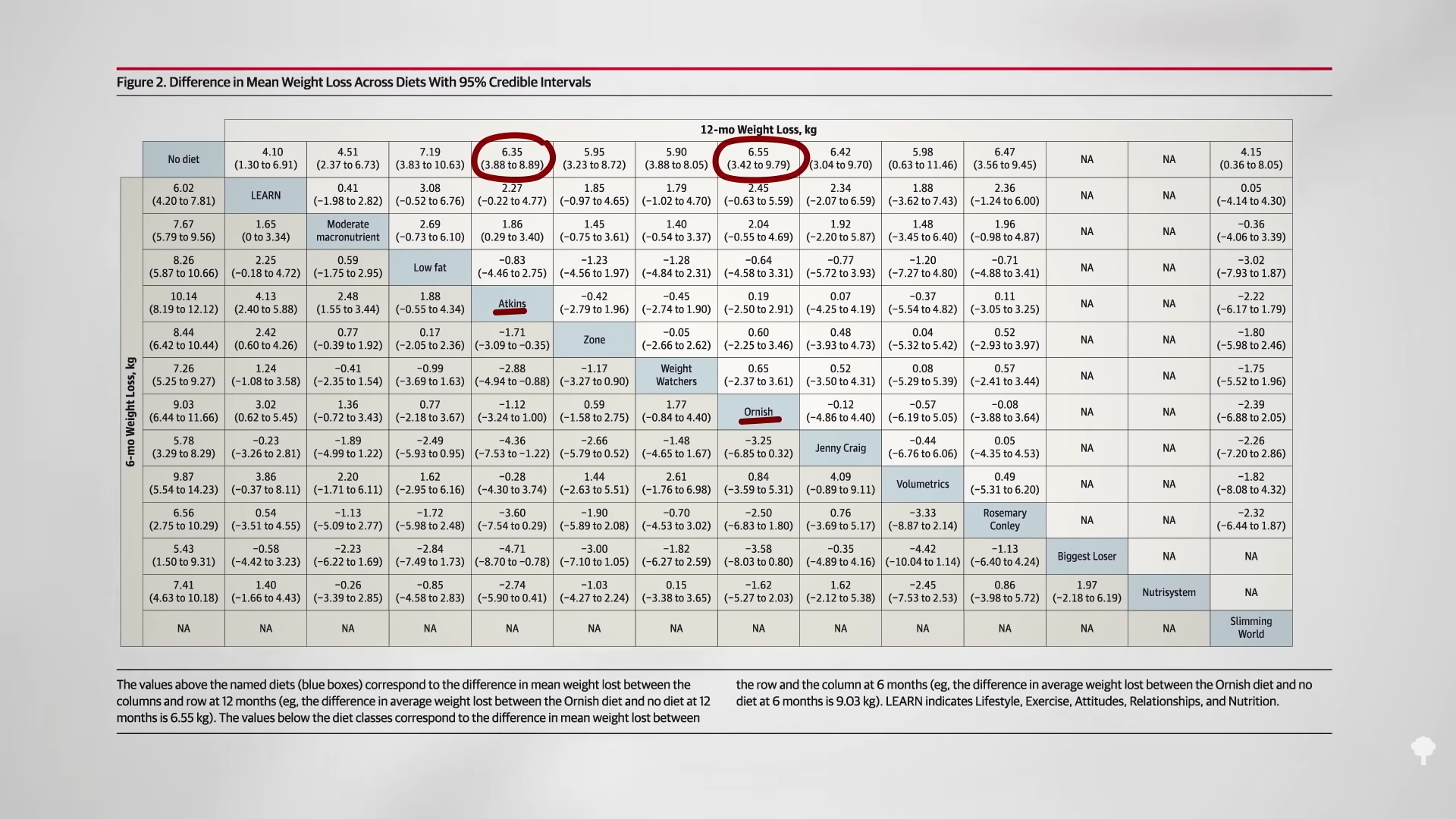
Remember the study that showed the weight loss was nearly identical in those who had been told to eat the low-carb Atkins diet for a year and those told to eat the low-fat Ornish diet, as seen below and at 4:18 in my video? The authors concluded, “This supports the practice of recommending any diet that a patient will adhere to in order to lose weight.” That seems like terrible advice.
There are regimens out there like “The Last Chance Diet which consisted of a low-calorie liquid formula made from leftover byproducts from a slaughterhouse [that] was linked to approximately 60 deaths from cardiovascular-related events.” An ensuing failed lawsuit from one widower laid the precedent for the First Amendment protection for those who produce deadly diet books.
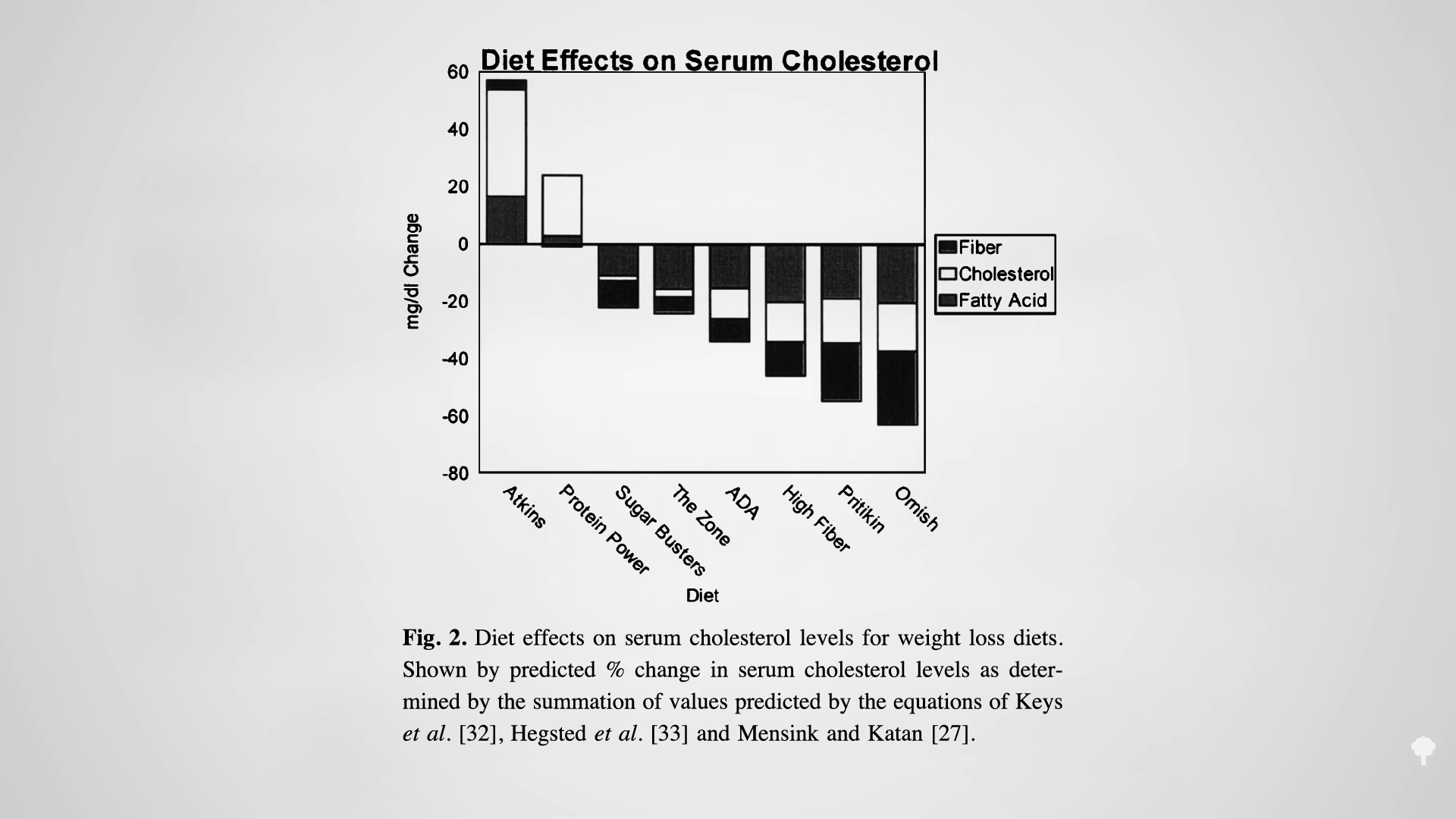
It’s possible to construct a healthy low-carb diet or an unhealthy low-fat one—a diet of cotton candy would be zero fat—but the health effects of a typical low-carb ketogenic diet like Atkins are vastly different from a low-fat plant-based diet like Ornish’s. As you can see in the graph below and at 5:26 in my video, they would have diametrically opposed effects on cardiovascular risk factors in theory, based on the fiber, saturated fat, and cholesterol contents of their representative meal plans.
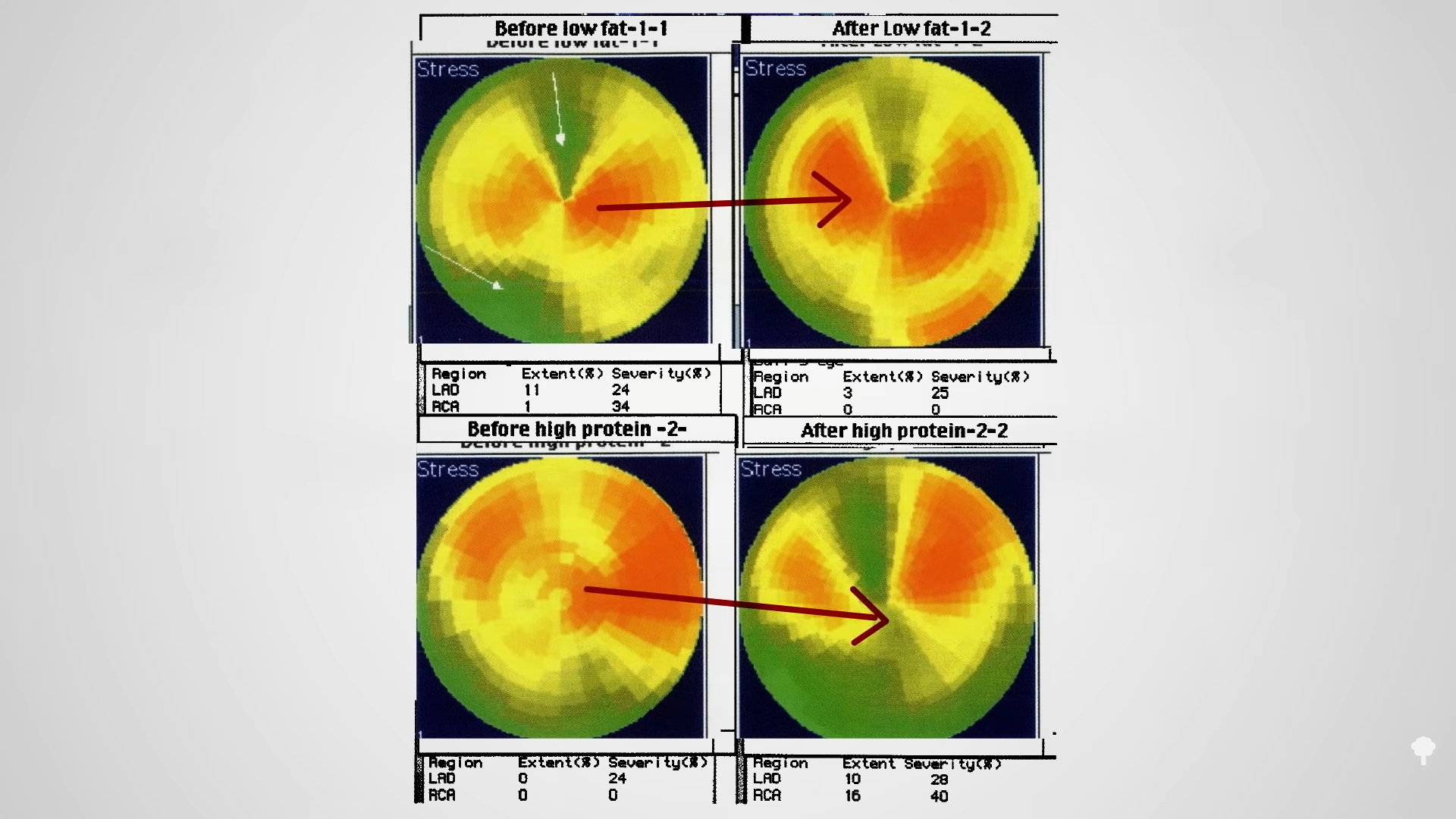
And when actually put to the test, low-carb diets were found to impair artery function. Over time, blood flow to the heart muscle itself is improved on an Ornish-style diet and diminished on a low-carb one, as shown below and at 5:44 in my video. Heart disease tends to progress on typical weight-loss diets and actively worsens on low-carb diets, but it may be reversed by an Ornish-style diet. Given that heart disease is the number one killer of men and women, “recommending any diet that a patient will adhere to in order to lose weight” seems irresponsible. Why not tell people to smoke? Cigarettes can cause weight loss, too, as can tuberculosis and a meth habit. The goal of weight loss is not to lighten the load for your pallbearers.
For more on keto diets, see my videos on the topic. Interested in enhancing athletic performance? Check out the related videos below.
[ad_2]
Michael Greger M.D. FACLM
Source link




![Snoop Dogg finally QUITS smoking marijuana [VIDEO] – Medical Marijuana Program Connection](https://reportwire.org/wp-content/uploads/2022/04/mmp-logo.jpg)












