For years, Tylenol has generally been considered safe for treating pain and fever — even during pregnancy, when doctors discourage patients from using many medications.
Doctors might even recommend taking Tylenol for pain or fever during pregnancy, because left untreated, they can pose their own health risks.
But recent news reports about the federal government connecting Tylenol to autism have drawn fresh questions about the drug, and concerns.
A few things are clear.
After years of research, no study has shown that acetaminophen, the main ingredient in Tylenol, causes autism. There’s no known single cause of autism, a neurological condition that influences how someone acts and communicates.
Sign up for PolitiFact texts
But some scientific terms, like “association,” can confuse the issue. There’s some research that says there’s an association between taking acetaminophen during pregnancy and autism. There’s also some research that says there’s not an association.
But either way, there’s an important caveat: “Association” is not the same as causation. That means that research showing an association between the medication and autism doesn’t mean the medication caused autism.
Here’s what else you should know.
#1: Doctors say it’s safe to use acetaminophen to reduce fever and pain during pregnancy.
After the Wall Street Journal reported on Health Secretary Robert F. Kenndy Jr.’s plans to link Tylenol to autism, leading maternal and prenatal care organizations reiterated their longstanding support for using acetaminophen during pregnancy.
The American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine said acetaminophen is a safe way to treat pain and fever when used in moderation.
“Pregnant patients should not be frightened away from the many benefits of acetaminophen, which is safe and one of the few options pregnant people have for pain relief,” said Dr. Christopher Zahn, ACOG’s chief of clinical practice.
In fact, Dr. Salena Zanotti, an obstetrician and gynecologist, told Cleveland Clinic earlier this year that acetaminophen is considered the safest drug to take during pregnancy for fever and pain.
“When you’re pregnant, it’s riskier to have an untreated fever than it is to take acetaminophen,” Zanotti said.
Other common pain relievers such as ibuprofen or naproxen — often sold as Advil or Aleve, respectively — aren’t recommended during pregnancy because they could harm fetal development, Zanotti said. The Food and Drug Administration said as much in 2023, advising that such nonsteroidal anti-inflammatory drugs, or NSAIDs, shouldn’t be used during pregnancy after 20 weeks of gestation.
#2: Having an untreated fever while pregnant can harm a baby.
Ignoring medical conditions such as fever that could be treated with acetaminophen during pregnancy is “far more dangerous than theoretical concerns based on inconclusive reviews of conflicting science,” Zahn said.
The Centers for Disease Control and Prevention says that fever during pregnancy has been linked to adverse outcomes including birth defects.
Untreated fever and pain during pregnancy has maternal and infant health risks, including preterm birth, according to the Society for Maternal-Fetal Medicine.
Generic acetaminophen capsules in Santa Ana, California. (AP)
#3: Research has not shown that using acetaminophen during pregnancy causes autism.
No study has shown using acetaminophen during pregnancy causes developmental disabilities — including autism.
But the language used in scientific research can be confusing. Words like “correlation,” “association,” and “increased risk,” in studies about acetaminophen use during pregnancy do not mean that the medication caused a disability like autism.
“Both ‘association’ and ‘increased risk’ are very different from ‘proven causal link,’” said Christopher J. Smith, chief science officer at Southwest Autism Research & Resource Center.
The FDA, the Society for Maternal-Fetal Medicine and ACOG have all reviewed the available research on acetaminophen use during pregnancy and subsequent neurodevelopmental issues in children and found no evidence proving the medication caused those disabilities, Zahn said.
“The vast majority of the studies done on acetaminophen use in pregnancy are inconclusive and unable to confirm a causal relationship between the prudent use of acetaminophen during pregnancy and fetal developmental issues,” he said.
#4: Some research has shown possible associations between prenatal acetaminophen exposure and childhood development — but here’s what that means.
For more than a decade, scientists have investigated potential associations between using acetaminophen during pregnancy and developmental disabilities.
Some studies have found positive associations between acetaminophen and autism, meaning children whose mothers took the drug during pregnancy were more likely to later have autism symptoms or be diagnosed with autism.
A 2025 Mount Sinai study that reviewed some existing research concluded the available evidence supported an association between prenatal acetaminophen exposure and increased incidence of neurodevelopmental disorders.
But the largest study on this topic, from 2024, found no evidence supporting an increased risk of autism, attention-deficit/hyperactivity disorder or intellectual disability associated with acetaminophen use during pregnancy.
The 2024 study is one of the two highest quality studies on the topic, Zahn said, and neither found an association between acetaminophen use and adverse neurodevelopmental outcomes.
What does this mean for confused parents? Associations between acetaminophen and autism are “based on limited, conflicting, and inconsistent science and is premature given the current science,” according to the Autism Science Foundation.
There’s yet another wrinkle: the potential for “publication bias,” a phrase that describes when scientific publications avoid publishing findings that don’t show significant associations. That means studies that don’t find an association between autism and acetaminophen are less likely to be accepted for publication, said Dr. Judette Louis, dean of Old Dominion University’s medical school and chair of the Society for Maternal-Fetal Medicine publications committee.
#5: An association between prenatal acetaminophen exposure and autism might be explained by other factors.
Research has shown that genetics plays a role in autism. Hundreds of genes have been linked to autism, as have some environmental factors such as how old parents are when a child is conceived, low birth weights, and fever or illness during pregnancy, the Autism Science Foundation said.
Brian Lee, a Drexel University epidemiology professor, coauthored the 2024 study, which evaluated data on nearly 2.5 million births in Sweden from 1995 to 2019 to assess acetaminophen use during pregnancy and the risk of autism. The study initially replicated a small statistical association between acetaminophen use and the risk of autism and ADHD, Lee said.
“However, when we did a sibling analysis that compared siblings (born to the same mother), the association completely went away,” he said. “We do the sibling analysis because it allows us to control for genetic and environmental factors that we do not otherwise have data on.”
The sibling analysis showed that other factors caused the initial statistical association, Lee said. The paper highlighted the possibility that genetics acted as a variable that could predict both a mother’s use of pain relief medication and a child’s risk of autism.
A mother’s genetic predisposition for autism and ADHD, which is also genetic, is associated with “greater pregnancy pain, more headache and migraine, and more use of pain-relieving medications,” Lee said. In other words, mothers who are genetically predisposed toward autism or ADHD are more likely to have conditions that cause them to use acetaminophen — and that same genetic predisposition could be what increases the likelihood of a child having those conditions.
Another consideration: Many studies rely on parents self-reporting acetaminophen use, so the data could be unreliable.
Someone might be more likely to remember taking acetaminophen during pregnancy if their child has autism or ADHD, for example — especially if they think there could be a connection between the drug and the diagnosis, according to Dr. Erin Clark, a University of Utah obstetrics and gynecology professor. A person might also be less likely to remember taking acetaminophen during pregnancy if their child hasn’t received such a diagnosis.
Zoe Gross, director of advocacy at the Autistic Self Advocacy Network, said other considerations might explain any association between acetaminophen and autism. Conditions that cause someone to take acetaminophen during pregnancy — such as fever or migraine — might increase the likelihood that a child will be autistic.
RELATED: RFK Jr.’s statements about autism and environmental toxins conflict with ample research







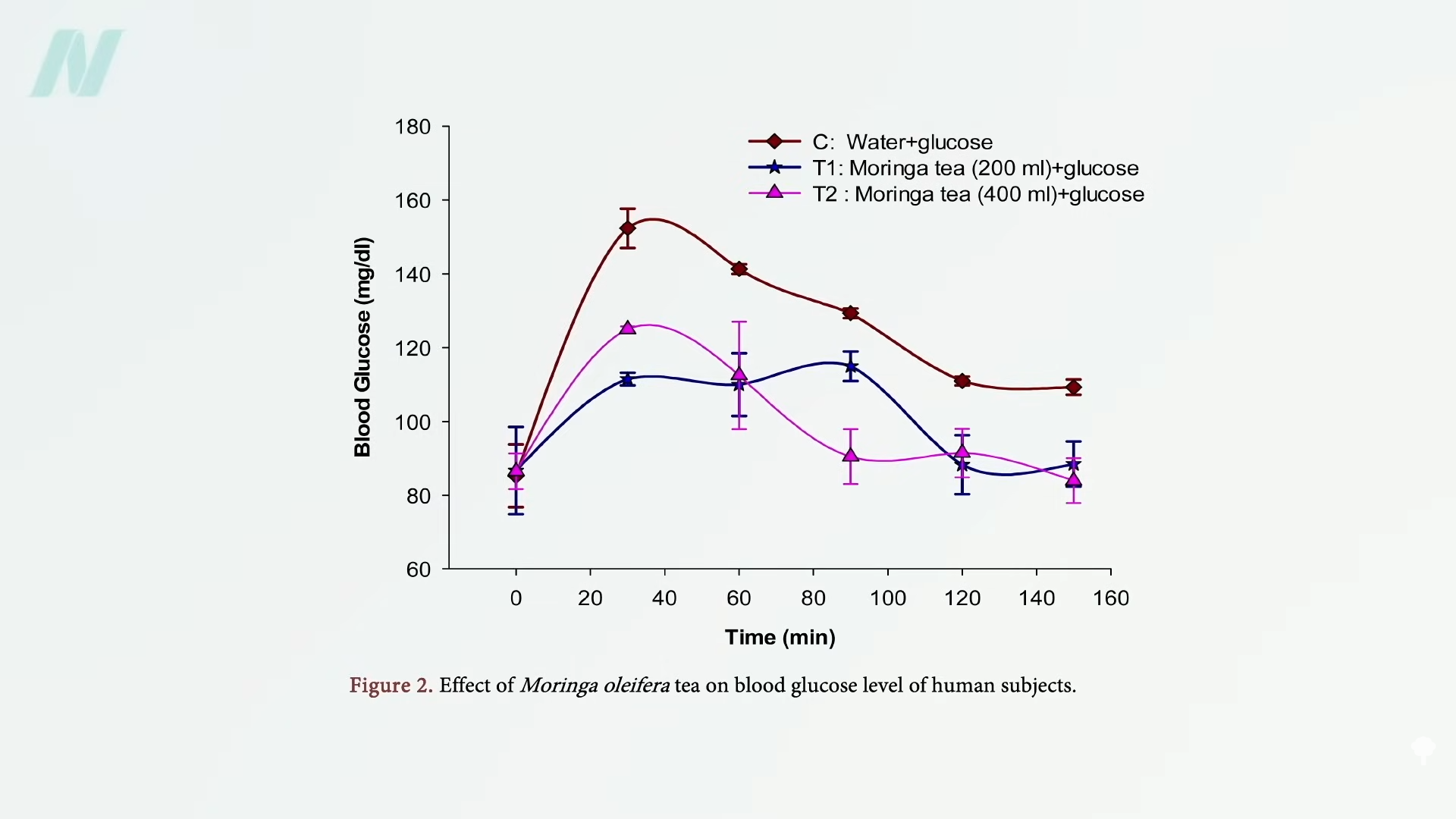 People with diabetes were
People with diabetes were