[ad_1]
In health care, the stakes are never abstract. Every decision we make echoes in the lives of patients, families, and the communities we serve. My work as a surgeon has taught me as much about leadership as any management role. In both surgery and leadership, I’ve had to make complex decisions, face unexpected challenges, and adapt in real time — the parallels are striking. As the medical director of Balgrist University Hospital, I have had the privilege, and the burden, of guiding our institution through periods of rapid growth, intense challenge, and transformative achievement.
My leadership credo is simple: Strive for excellence. It has been anchored in four principles, or “my recipe for achieving excellence”:
- Define a clear vision
- Build a nourishing environment
- Ensure you have the right people
- Open your doors to collaboration
These “ingredients” might seem simple, but their true power lies in how they are lived out daily.
Before diving into the characteristics of the four principles, we should ask ourselves why? Why should a hospital strive for excellence? Simply because we want the patients to be treated the very same way we would want to be treated ourselves. That’s the only way a hospital can resist all storms, in a sustainable way.
Ingredient 1: Define One Very Clear Goal
For me, leadership has never been about me as an individual. It’s the credo that leads — a set of values stronger and more enduring than any single person. That’s what sustains a culture over the long term.
Therefore, when aiming for excellence, everyone must also work toward the same goal. It must be clear, noble, and widely respected. Once defined, the goal, not the leader, guides decisions. Leaders ensure understanding, model behavior, and align all actions with it.
Our goal at Balgrist University Hospital is simple: Treat patients as we wish to be treated. This shapes everything from knocking respectfully before entering a room to making complex medical choices with empathy. It guides research toward patient needs rather than just academic metrics, and it drives us to take on regulatory burdens when innovations may help future patients.
This vision became our compass for all strategy, from research investments to recruitment. As a specialized university hospital, focus is vital. Our niche allows unmatched depth but demands discipline, resisting distractions that dilute our mission.
Ingredient 2: Build a Nourishing Environment
Vision inspires, but without the right environment, progress stalls. Leadership means ensuring that both culture and structure support the mission.
Culturally, we value mutual respect and a shared patient-first commitment. Organizational clarity is equally important. Everyone knows their role, responsibilities and how their work connects to our mission. Clear reporting lines and streamlined communication enable swift and accurate decisions. Departments operate with transparent goals and accountability, empowering decisive action and efficient collaboration.
Our clinical structure centers on specialized units such as the Spinal Cord Injury Center, the University Spine Center, the University Foot Center, and the University Center for Prevention and Sports in Medicine, which unite multidisciplinary teams and give clinicians more time for patients. In research, the new Clinical Trial Unit Balgrist accelerates clinical experiments by supporting physician scientists.

We invested in modern tools, digital records, integrated patient pathways and well-designed team workspaces.
Our mission includes shaping the future of musculoskeletal care, so robust infrastructure is essential.
Balgrist University Hospital hosts more than 20 research groups, from biomechanics to bone sarcoma research. Before 2015, these groups worked independently, limiting collaboration. That is why we built Balgrist Campus, a 7,000-square-meter hub with offices and shared musculoskeletal centers for imaging, biobanking and movement analysis. This boosted our output to more than 400 publications annually and enabled even faster innovation cycles.
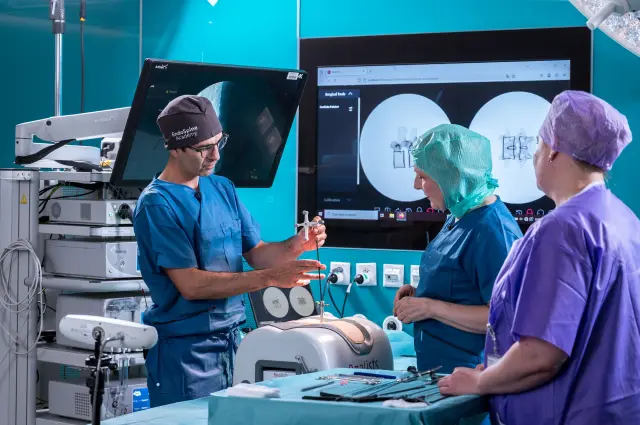
To further support innovation without disrupting clinical operations, we launched the Operating Room X (OR-X) in 2023: a dedicated surgical research, education and training space with advanced technology and artificial intelligence tools. Together, Balgrist Campus and OR-X integrate basic, translational and clinical science in one location.
The lesson is to invest in spaces and tools that bring the right people together. Such initiatives need not be as large as a new campus or OR-X; even small measures, like shared coffee areas, can strengthen collaboration. When tailored to a hospital’s resources and executed well, these investments deliver exponential returns.
Ingredient 3: Have the Right People (and Get Out of Their Way)
The right people genuinely believe in the mission. They are not always easy to find, so we grow them ourselves.
For physicians, our pipeline starts with medical students, continues through residency and fellowship, and culminates in selecting top candidates as attending surgeons. This path instills our culture, standards and patient-first philosophy from the start. We especially nurture physician-scientists who are fluent in both patient care and research, who can ask the right clinical questions and bring evidence-based answers back to the bedside.
This dual expertise keeps us at the forefront of innovation that directly benefits patients. By the time someone becomes an attending surgeon here, they are technically excellent, mission-aligned and ready to advance medicine through research, teaching and care. This investment creates a self-renewing source of excellence for generations.
Our senior staff is the perfect example to illustrate our approach: Most have been here more than 10, 15, some even 20 years – and this is how we make sure the culture remains stable.
Ingredient 4: Open Your Doors
Specialized hospitals cannot thrive in isolation. Expertise grows when shared, and impact multiplies when connected. We built partnerships with universities, research institutions, industry and hospitals worldwide.
About 20 percent of our employees are affiliated with the University of Zurich or ETH Zurich, ensuring world-class academic integration. Partnerships give us access to pioneering research, emerging technologies and global talent.
We also created the Balgrist Beteiligungs AG, which supports young researchers and clinicians in bringing ideas to life. This has led to spinoffs such as Zurimed in soft tissue repair, Moving Spine in dynamic spinal stabilization, X23D in artificial intelligence surgical navigation, and AUGMEDI in three-dimensional medical education. Such ventures speed the path from concept to real-world patient impact.
Opening our doors also means engaging with the public through patient education, community health forums, and transparency about successes and setbacks. Trust comes not from claiming perfection but from demonstrating integrity.
Conclusion
Our journey to becoming a world leader in musculoskeletal medicine shows that leadership is about stewardship, protecting the vision, nurturing the environment, choosing the right people and staying open to the world. These principles are not sequential steps but a reinforcing cycle.
Excellence in health care is never final. Medical knowledge evolves, patient needs change and new challenges arise. With a vision rooted in empathy, treating patients as we wish to be treated, we are ready not just to adapt but to lead.
Recognition as a top CEO is an honor, but the real credit belongs to those who live this vision daily. Together, we will continue to set the standard in specialized care, not for accolades, but for the lives entrusted to us.
Prof. Dr. med. Mazda Farshad is a member of the Newsweek CEO Circle, an invite-only executive community of subscribers.
[ad_2]



