[ad_1]
For Lacy Cornelius Boyd, March 19, 2024, was an exciting day. She and her husband had taken their 6-year-old daughter to the Grand Canyon as part of a family road trip. Boyd, her husband and their daughter were planning to stop at McDonald’s before heading home to Oklahoma.
Everything was well — until their car hit a patch of black ice.
“We were spinning. My husband obviously lost control, and he hit another car head-on,” Boyd recalled. Everything else was a blur.
Boyd’s daughter had a broken arm. Her husband and the other driver were fine. Boyd had broken bones in her neck and ribs, a collapsed lung, and severe injuries to her intestines. She had six surgeries in five days.
But the damage to her intestines — caused by a too-tight seatbelt — kept getting worse, Boyd said.
“They were trying to save my intestines, and every time they would go back in, they were just dying from no blood flow,” Boyd said. “I was told that most people have 35 feet of small intestine. I was left with about 35 inches.”
Lacy Cornelius Boyd
“Just going through the motions”
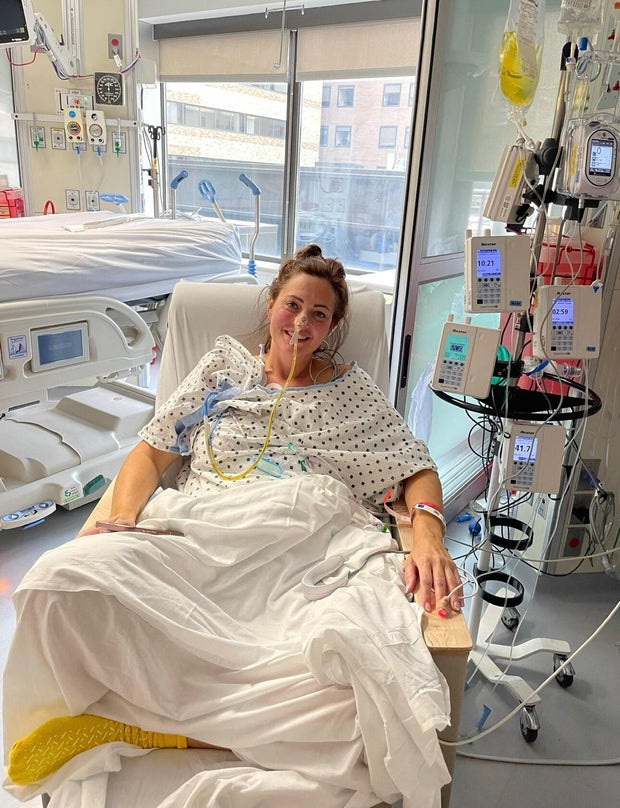
Boyd was discharged from the hospital after a month. She was diagnosed with short bowel syndrome and had an ileostomy bag attached to her side to collect waste. Her remaining intestines couldn’t process the nutrients from food, so she needed 12 hours of IV nutrition a day. She said her daughter was afraid of the tubes, wires and medical machines that now filled their home. Boyd was always weak and dehydrated, and never wanted to leave the house.
“If I went out to eat somewhere, I’d be in the bathroom immediately, or I’d have to go to the bathroom five times at a restaurant, so it was just embarrassing,” Boyd said. “I felt like everyone was enjoying their life and I was just going through the motions.”
Lacy Cornelius Boyd
Boyd, who had previously worked in healthcare, regularly met with doctors to see if her quality of life could be improved. No one had answers. Finally, she followed up on an unlikely lead. During her hospitalization, a surgeon had told Boyd’s sister she should contact the Cleveland Clinic.
Boyd self-referred herself to the hospital system in November 2024. She met with general surgeon Dr. Masato Fujiki and after an evaluation, he suggested something she’d never heard of before: An intestinal transplant.
“I started crying. I think he thought I was sad, but I was really happy,” Boyd said. “Everyone had told me that was going to be my life.”
A rare, risky transplant
Intestinal transplants are a rare procedure, said Dr. Adam Griesemer, a transplant surgeon at NYU Langone. Only about 100 are done in the U.S. every year, compared to the 25,000 kidney transplants done annually, said Fujiki, the director of Cleveland Clinic’s Intestinal Transplant Program.
Intestinal transplants have the worst outcomes of any type of transplant, Griesemer said, so there is a “high threshold” for doctors to consider them. They are generally only recommended for children born with intestinal defects and people who will be dependent on IV nutrition for the rest of their lives, like Boyd, he said.
Intestinal transplant patients “really struggle with rejection and infections,” Griesemer said. Intestines harbor bacteria inside them, so during cases of organ rejection, the barrier preventing the bacteria from entering the bloodstream breaks down. Fujiki said rejection rates have been improving over the past decade, estimating that it has decreased from 40% of cases to about 8%. Medication can help reduce infections, he said.
Only about 50% of patients survive more than five years after receiving the transplant, Griesemer said. In comparison, kidney transplants have a 98% five-year survival rate.
“Prepared for the worst”
Boyd began the process of getting listed for an intestinal transplant in November. In July 2025, 16 months after the car crash, Boyd received the transplant at the Cleveland Clinic. The day of the operation was filled with emotion, she said.
“I was excited. I was nervous. I was sad about leaving my daughter, and I felt for the donor’s family,” Boyd said. “But really, I was prepared for the worst.”
Lacy Cornelius Boyd
The operation took about 12 hours, Fujiki said. Everything went smoothly. But it was just the first step in a long process: Boyd spent the next three weeks recovering in the hospital, followed by three months of outpatient recovery in Cleveland so she could stay near her care team for close monitoring.
Boyd had no complications in her recovery, Fujiki said. Her ostomy bag was removed. She no longer needed IV nutrition. The weekend before Thanksgiving, she returned to Oklahoma.
“It was amazing to be able to come home,” Boyd said.
A festive return home
Boyd arrived home just in time for beloved holiday traditions. After missing other milestones, like her daughter’s first day of school and Halloween, Boyd was relieved to be a part of the celebrations.
“My daughter is six now, but my husband carries her to the Christmas tree every morning to get her presents. I don’t know how much longer she’s going to let him do that,” Boyd said. “I was like, ‘This year might be the last time, and I’ll miss it.’ But I didn’t.”
Boyd remains on a regimen of anti-rejection medications and will continue to receive follow-up care at the Cleveland Clinic. Otherwise, normalcy reigns, and it feels like the last of the trauma from the crash has been repaired, she said.
“It’s nice to take my daughter to school, pick her up, not have to worry about anything, to take her and to be able to go out to eat. I couldn’t drink Coke before. I couldn’t do normal things for like, a year and a half,” Boyd said. “It’s so much. Everyone is just a little bit more at peace.”
Lacy Cornelius Boyd
[ad_2]