The change in Zack Rogers was sudden. In the middle of his 12th birthday party, his stomach started hurting. He went to bed early that night, missing much of his own slumber party, and then stayed home from school the whole next week. The stomach pain was excruciating, and he couldn’t keep any food down. He lost 40 pounds in just a few weeks.
Zack spent the next three years in and out of hospitals and trying medicines that didn’t seem to work. His doctors eventually told the family that they had only one option: surgery to remove large parts of his damaged colon. But Zack’s mom, Angela Rogers, wasn’t on board. She had lost faith in his medical team and feared such an invasive step, so she asked another gastroenterologist for a second opinion. The new doctor suggested that Zack try one last treatment before surgery: hypnotherapy, in which a clinical professional helps a patient become deeply focused and relaxed in order to change their patterns of thinking.
This time, the change was gradual, but no less dramatic. In the evening after his first hypnotherapy session, Zack felt nauseated but kept his dinner down. Over the next few weeks, he stopped throwing up in school and regained the stamina to play basketball and go for bike rides. Today, Zack is a freshman in college, living away from home—something he wouldn’t have thought was possible before he was hypnotized. “If I never did hypnosis,” he told me, “I would be a complete mess. I genuinely don’t know where I would be.”
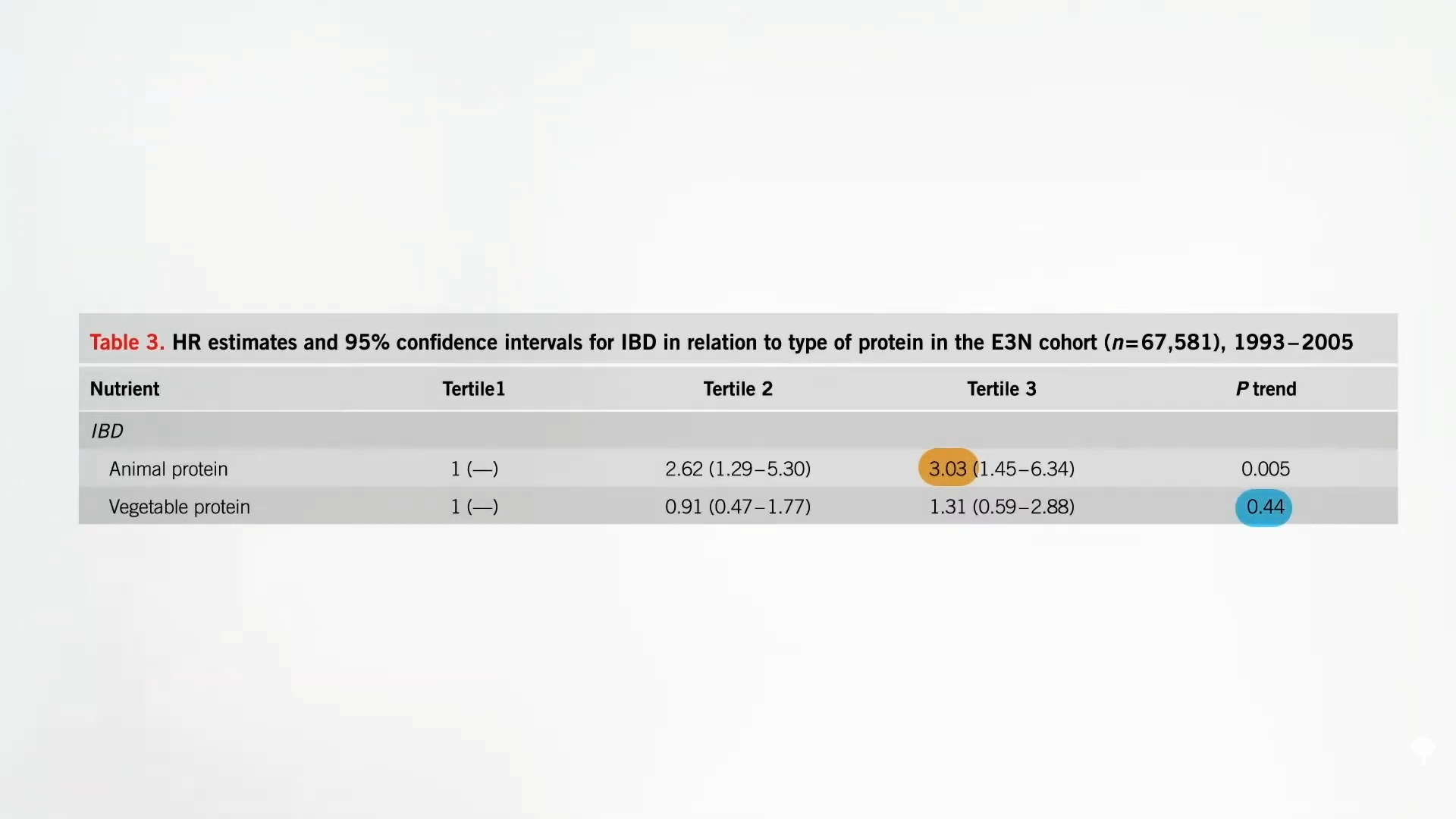
As far-fetched as it may seem, science supports the idea that digestive disorders can be treated with psychological interventions, including hypnosis. Research dating back to the 1980s suggests that, at least in the short term, hypnotherapy can be an effective treatment for irritable bowel syndrome, a gut disorder characterized by painful gastrointestinal symptoms but no visible damage to the gut. Now scientists are investigating whether it might also bring relief to patients with inflammatory bowel disease, who, like Zack, have observable damage to their digestive tract.
Although hypnosis is a powerful relaxation tool on its own, in clinical settings, it’s most often combined with other, better-studied psychotherapy techniques, such as cognitive behavioral therapy. Research suggests that CBT, which is commonly used to treat conditions such as depression and anxiety, can also be helpful in the treatment of gastrointestinal disorders.
Read: I got hypnotized over Skype and it actually worked
Unlike CBT, hypnosis retains a reputation for quackery, and is regularly portrayed in pop culture and stage shows as a tool for exercising control over participants—willing or otherwise. And some practitioners do use it for debunked treatments, including recovered memory therapy. But whether hypnotherapy is legitimized as a medical tool has real stakes. Hypnosis practitioners believe—and there’s some research to back this up—that the technique may amplify the effectiveness of more well-established psychological interventions and therefore has the potential to provide rare benefit to patients
Hypnosis has a long history as a pain reliever. In the first half of the 19th century, before anesthetics were widely available, some surgeons hypnotized their patients. Even today, hypnosis proponents claim that it may be an effective alternative treatment for chronic back pain and the stress of childbirth; a growing body of research suggests that hypnosis can be a cost-effective and side-effect free analgesic for some people with chronic pain, though good clinical data are hard to come by.
The first randomized controlled trial of hypnotherapy for IBS was published in 1984. Among the participants—a small group of mostly female patients with severe, treatment-resistant disease— those who received hypnotherapy showed greater improvements in abdominal pain, bloating, and bowel function than those who received psychotherapy plus a placebo medication. A 2014 meta-analysis found that about half of IBS patients who try hypnotherapy see at least short-term improvements in their symptoms.
Read: The rogue theory that gravity causes IBS
The evidence for hypnotherapy isn’t as robust in the treatment of IBD, which is really an umbrella term for ulcerative colitis (Zack’s diagnosis) and Crohn’s disease. But there’s reason to believe that hypnosis could yield similar success in addressing symptoms of those conditions. The line between IBD and IBS can be murky; more than a quarter of IBD patients in remission have IBS as well. And although the evidence is still mixed—a study published in 2021, for example, found no difference in treatment outcomes between standard medical treatments and hypnotherapy—some early evidence suggests that hypnotherapy can also reduce inflammation in patients with ulcerative colitis. One small study found that just one session of hypnotherapy reduced ulcerative-colitis patients’ blood levels of several inflammatory markers.
Perhaps most important, a large body of research shows a strong link between cognition and digestion. Millions of neurons, collectively known as the enteric nervous system, regulate our digestion and are in constant communication with the central nervous system. This connection, called the “brain-gut axis,” may be why we feel so many emotions in our gut, whether the butterflies of anxiety or the clench of anger. It might also explain why both anxiety and depression are more common among patients with IBD compared with the general population. “Unequivocally, stress plays a major role in any digestive disease,” Gary Lichtenstein, a gastroenterology professor and the director of the Inflammatory Bowel Disease Center at the Hospital of the University of Pennsylvania, told me.
When this brain-gut axis gets out of whack, it’s known to worsen some digestive disorders. In patients with gastrointestinal issues, the tissues in the gut can become hypersensitive over time. The brain learns to interpret signals from the gut, including normal functioning, as discomfort. This faulty communication results in what experts now call disorders of gut-brain interaction (DGBIs), which include IBS, functional dyspepsia, and other digestive disorders (but not IBD). Hypnosis, proponents say, can help patients rewire the cognitive-digestive connection. In many IBS and IBD cases, “we know there’s a mind-gut connection that can only be helped by a mental-health expert,” says Mark Mattar, a gastroenterologist and director of the IBD center at MedStar Georgetown University Hospital.
Read: When gut bacteria change brain function
Mattar works closely with Ali Navidi, the clinical psychologist to whom Zack was referred in 2020. Navidi told me that at his practice, GI Psychology, 83 percent of patients with DGBIs who complete at least 10 hypnotherapy sessions achieve their treatment goals, which usually amount to reducing pain, bloating, and other uncomfortable symptoms enough to go about their day-to-day life. His data are unpublished but in line with other studies on IBS showing that more than 80 percent of patients who get gut-directed hypnotherapy as part of their treatment plan experience improvements in pain and other GI symptoms. Those numbers are even higher among children and adolescents.
Such findings persuaded the American College of Gastroenterology to recommend gut-directed psychotherapies—including hypnosis and CBT—for the treatment of IBS symptoms in its 2021 guidelines. Still, even among IBS patients, they’re not commonly used. No one appears to have studied the popularity of hypnosis specifically among IBS patients, but a 2017 study found that only 15 percent of people diagnosed with IBS had ever pursued “psychological therapies” of any kind.
For many patients who follow through with hypnotherapy, the experience is not what they expect. Patients may conflate clinical hypnosis with entertainment hypnosis, where subjects quack like a duck or forget their own name. But at practices like Navidi’s, the therapist instead focuses on helping the patient enter a trance state—the same type of consciousness we all experience when we lose track of time working, scrolling Instagram, or driving and suddenly arriving at our destination. “When we’re in a trance, we have this intense, focused concentration, and that can be used in powerful ways,” Navidi said.
Once the patient is in a trance state, therapists use guided imagery and suggestion to target specific gastrointestinal symptoms. “People get into a very relaxed state, and in that state I start to make suggestions about how the brain and the gut can work together better,” Jessica Gerson, a psychologist at NYU Langone’s Inflammatory Bowel Disease Center, told me. Gerson instructs her IBD patients to imagine the lining of their intestines healing. During his trance states, Zack was able to envision a control room for his pain in which he could dial knobs up and down. “I could turn the stomach pain down to a one or a zero, and it would go away,” Zack recalled recently, a note of surprise still in his voice.
Read: Can you quit smoking through hypnosis?
Many patients initially fear that during hypnosis they are ceding control of their mind and body to the hypnotherapist, Gerson told me. But patients are always “totally conscious, totally in control.” Indeed, Navidi and Gerson use this trance state to show patients exactly how much control they have over their own body. “Having a sense of agency is therapeutic,” Gerson said.
These days, many gastroenterologists see psychotherapies like hypnosis as an important part of a holistic treatment plan—even for IBD. (IBD patients who do respond to hypnotherapy are likely to continue to need medical monitoring and interventions, Lichtenstein said.) While gut-directed hypnotherapy still hasn’t been proved to help IBD patients without co-occurring IBS symptoms, there’s not much of a downside to trying. The experts I spoke with agreed that hypnosis is relatively risk-free as long as it is administered by a clinician, patients continue to be monitored by their medical doctors, and therapists screen potential patients for severe mental illness and untreated trauma. Patients, too, need to consider whether they can afford hypnotherapy. Like many mental-health services, it’s not always covered by insurance. Zack’s sessions were $265 each out of pocket, but according to Angela, “it was worth every cent and then some.”
Zack remembers getting stressed out a lot as a kid—over grades, making friends, basketball games, or nothing in particular. He credits Navidi with alleviating not only his stomach pain but also the relentless anxiety; he still uses the relaxation techniques he learned from Navidi when he gets worried about school or a basketball game.
Read: Reiki can’t possibly work. So why does it?
Zack is still on medication for his ulcerative colitis; every eight weeks he has an injection of Stelara, a medication that works by blocking inflammatory proteins. But after two years of appointments with Navidi, for the first time since his 12th birthday, his symptoms are reliably under control—and stress doesn’t make them come roaring back. He hasn’t had a flare up in about a year and a half. Most days, he doesn’t think about his diagnosis at all.