[ad_1]
Newswise — Certain populations of mosquitoes are more heat tolerant and better equipped to survive heat waves than others, according to new research from Washington University in St. Louis.
This is bad news in a world where vector-borne diseases are an increasingly global health concern. Most models that scientists use to estimate vector-borne disease risk currently assume that mosquito heat tolerances do not vary. As a result, these models may underestimate mosquitoes’ ability to spread diseases in a warming world.
Researchers led by Katie M. Westby, a senior scientist at Tyson Research Center, Washington University’s environmental field station, conducted a new study that measured the critical thermal maximum (CTmax), an organism’s upper thermal tolerance limit, of eight populations of the globally invasive tiger mosquito, Aedes albopictus. The tiger mosquito is a known vector for many viruses including West Nile, chikungunya and dengue.
“We found significant differences across populations for both adults and larvae, and these differences were more pronounced for adults,” Westby said. The new study is published Jan. 8 in Frontiers in Ecology and Evolution.
Westby’s team sampled mosquitoes from eight different populations spanning four climate zones across the eastern United States, including mosquitoes from locations in New Orleans; St. Augustine, Fla.; Huntsville, Ala.; Stillwater, Okla.; St. Louis; Urbana, Ill.; College Park, Md.; and Allegheny County, Pa.
The scientists collected eggs in the wild and raised larvae from the different geographic locations to adult stages in the lab, tending the mosquito populations separately as they continued to breed and grow. The scientists then used adults and larvae from subsequent generations of these captive-raised mosquitoes in trials to determine CTmax values, ramping up air and water temperatures at a rate of 1 degree Celsius per minute using established research protocols.
The team then tested the relationship between climatic variables measured near each population source and the CTmax of adults and larvae. The scientists found significant differences among the mosquito populations.
The differences did not appear to follow a simple latitudinal or temperature-dependent pattern, but there were some important trends. Mosquito populations from locations with higher precipitation had higher CTmax values. Overall, the results reveal that mean and maximum seasonal temperatures, relative humidity and annual precipitation may all be important climatic factors in determining CTmax.
“Larvae had significantly higher thermal limits than adults, and this likely results from different selection pressures for terrestrial adults and aquatic larvae,” said Benjamin Orlinick, first author of the paper and a former undergraduate research fellow at Tyson Research Center. “It appears that adult Ae. albopictus are experiencing temperatures closer to their CTmax than larvae, possibly explaining why there are more differences among adult populations.”
“The overall trend is for increased heat tolerance with increasing precipitation,” Westby said. “It could be that wetter climates allow mosquitoes to endure hotter temperatures due to decreases in desiccation, as humidity and temperature are known to interact and influence mosquito survival.”
Little is known about how different vector populations, like those of this kind of mosquito, are adapted to their local climate, nor the potential for vectors to adapt to a rapidly changing climate. This study is one of the few to consider the upper limits of survivability in high temperatures — akin to heat waves — as opposed to the limits imposed by cold winters.
“Standing genetic variation in heat tolerance is necessary for organisms to adapt to higher temperatures,” Westby said. “That’s why it was important for us to experimentally determine if this mosquito exhibits variation before we can begin to test how, or if, it will adapt to a warmer world.”
Future research in the lab aims to determine the upper limits that mosquitoes will seek out hosts for blood meals in the field, where they spend the hottest parts of the day when temperatures get above those thresholds, and if they are already adapting to higher temperatures. “Determining this is key to understanding how climate change will impact disease transmission in the real world,” Westby said. “Mosquitoes in the wild experience fluctuating daily temperatures and humidity that we cannot fully replicate in the lab.”
[ad_2]
Washington University in St. Louis
Source link


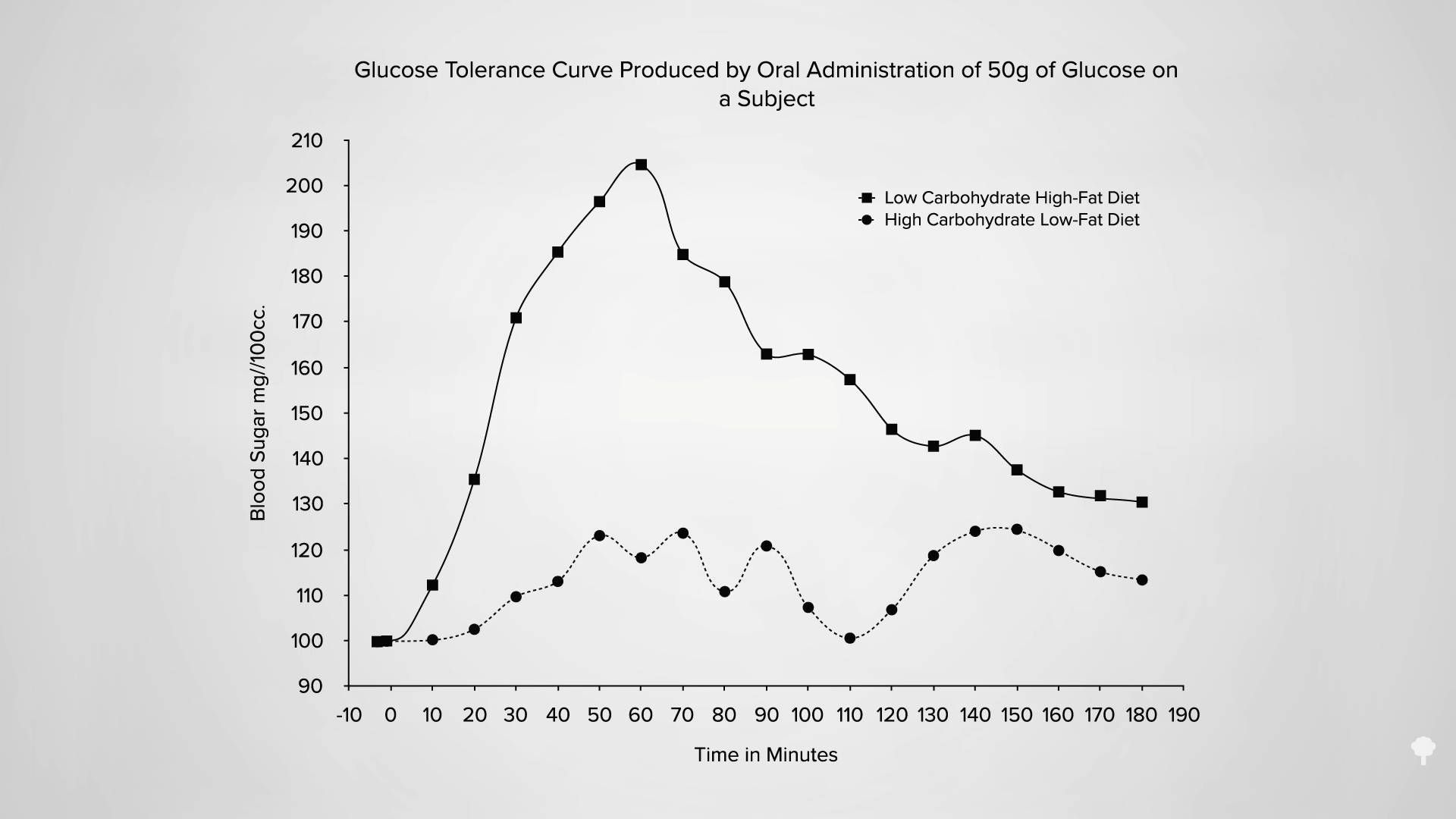
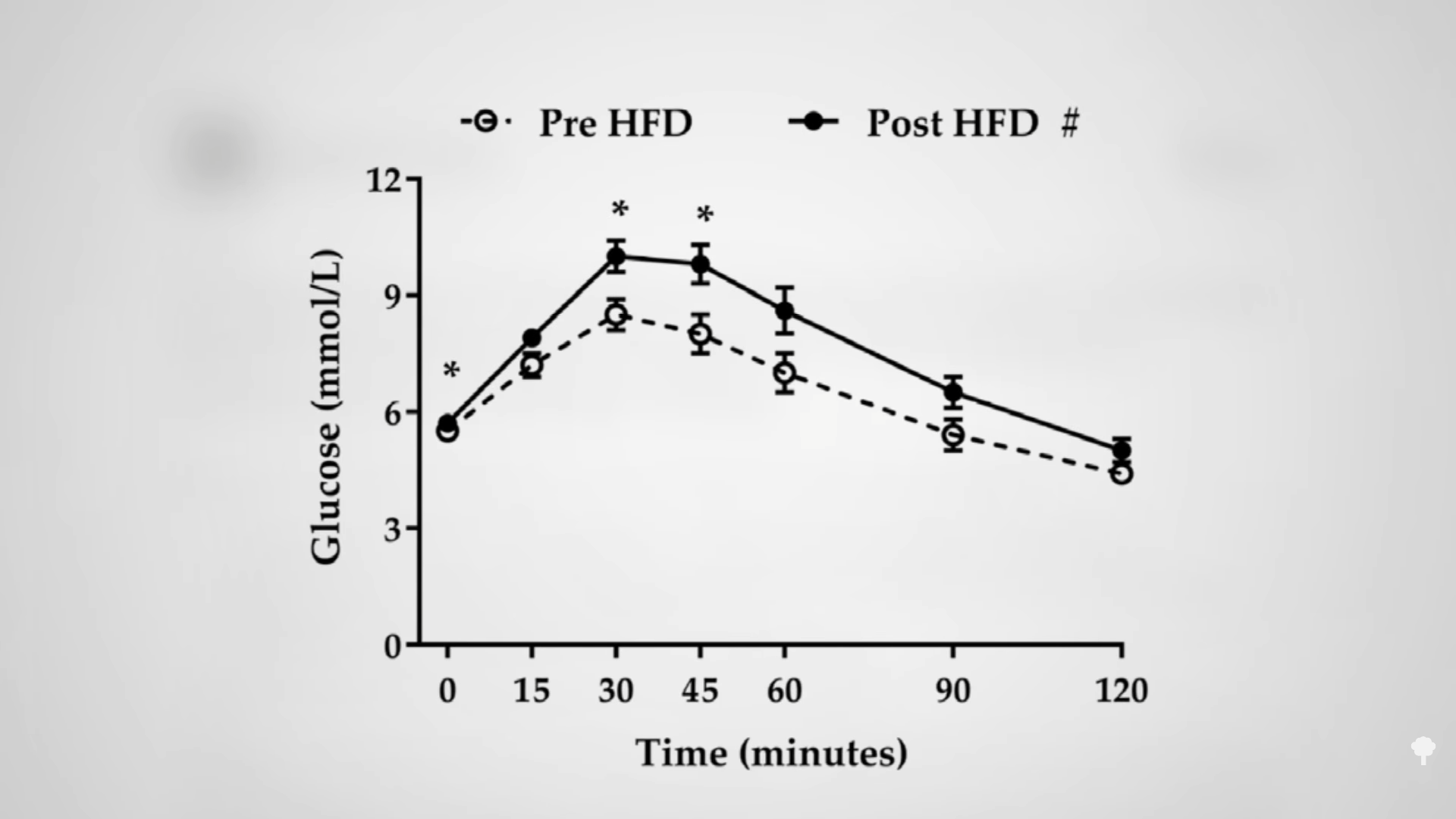
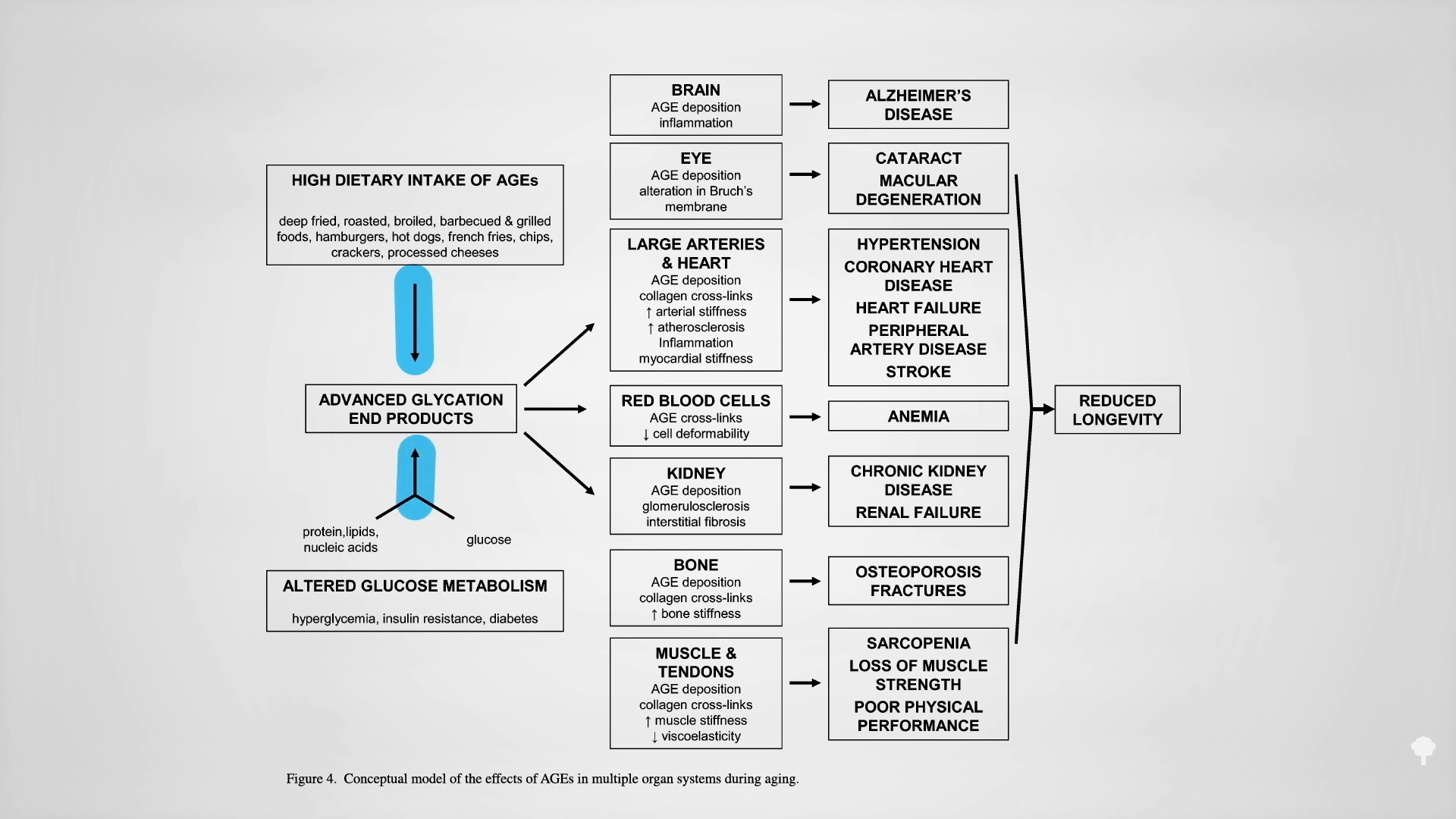
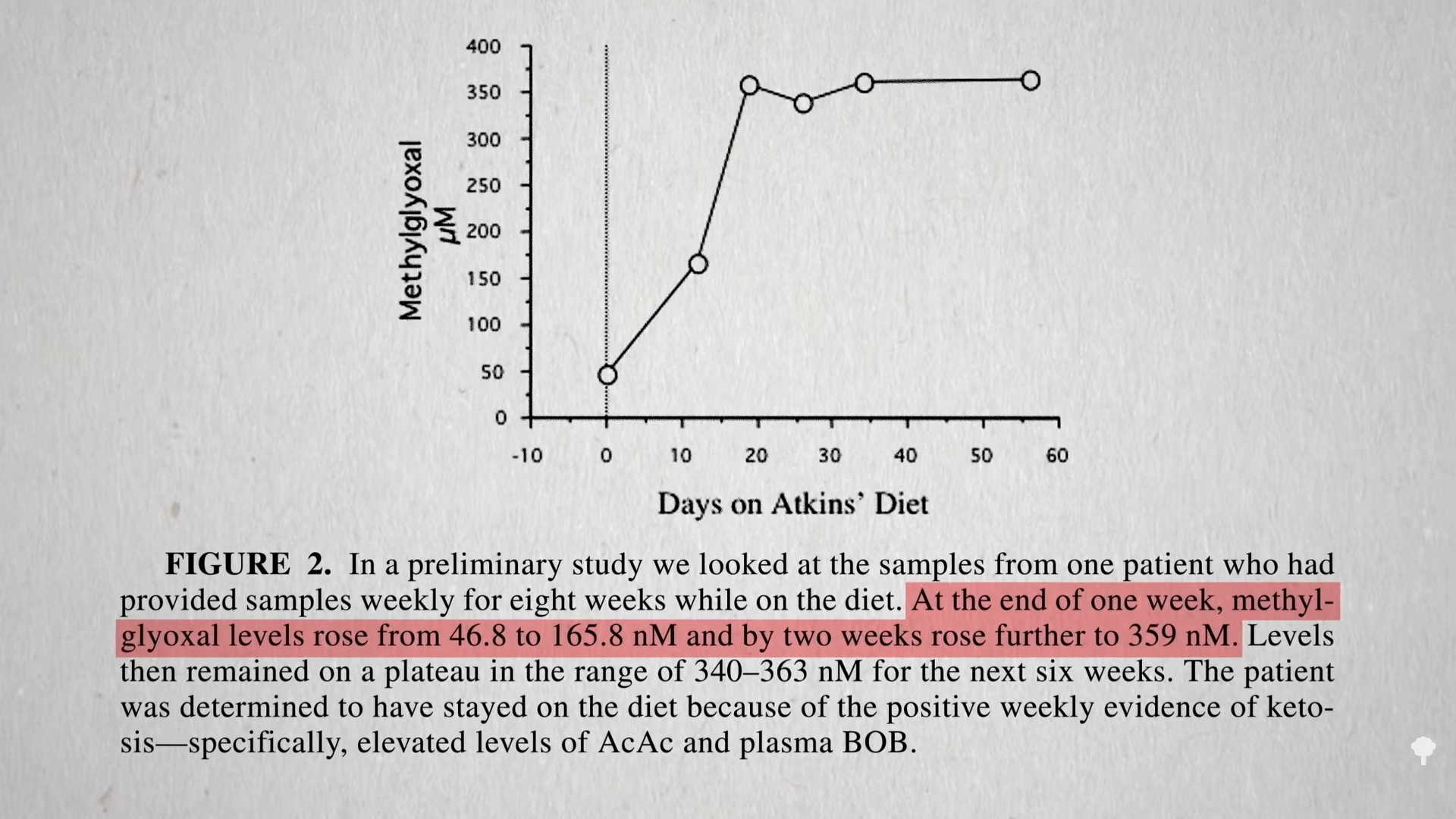
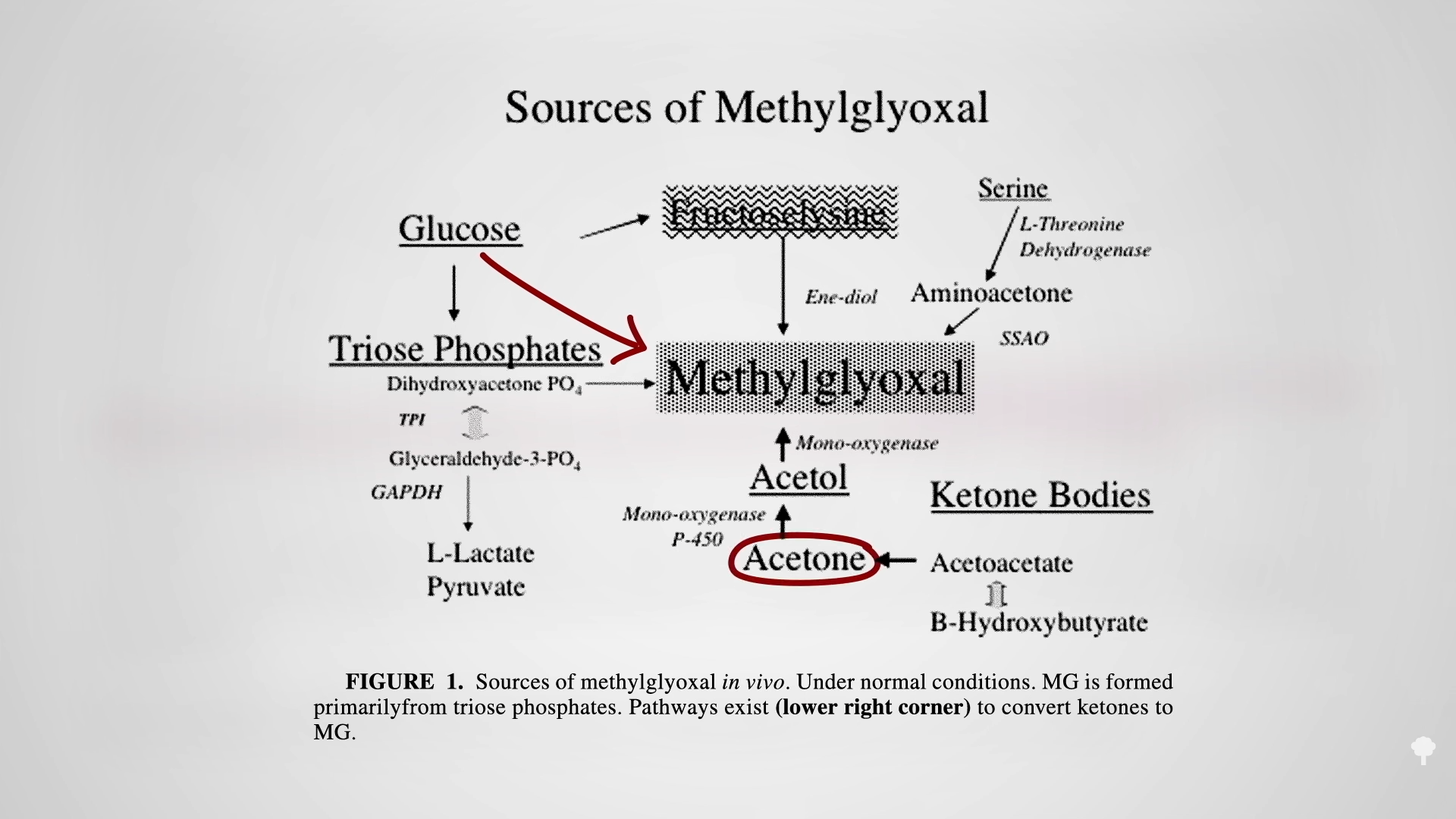
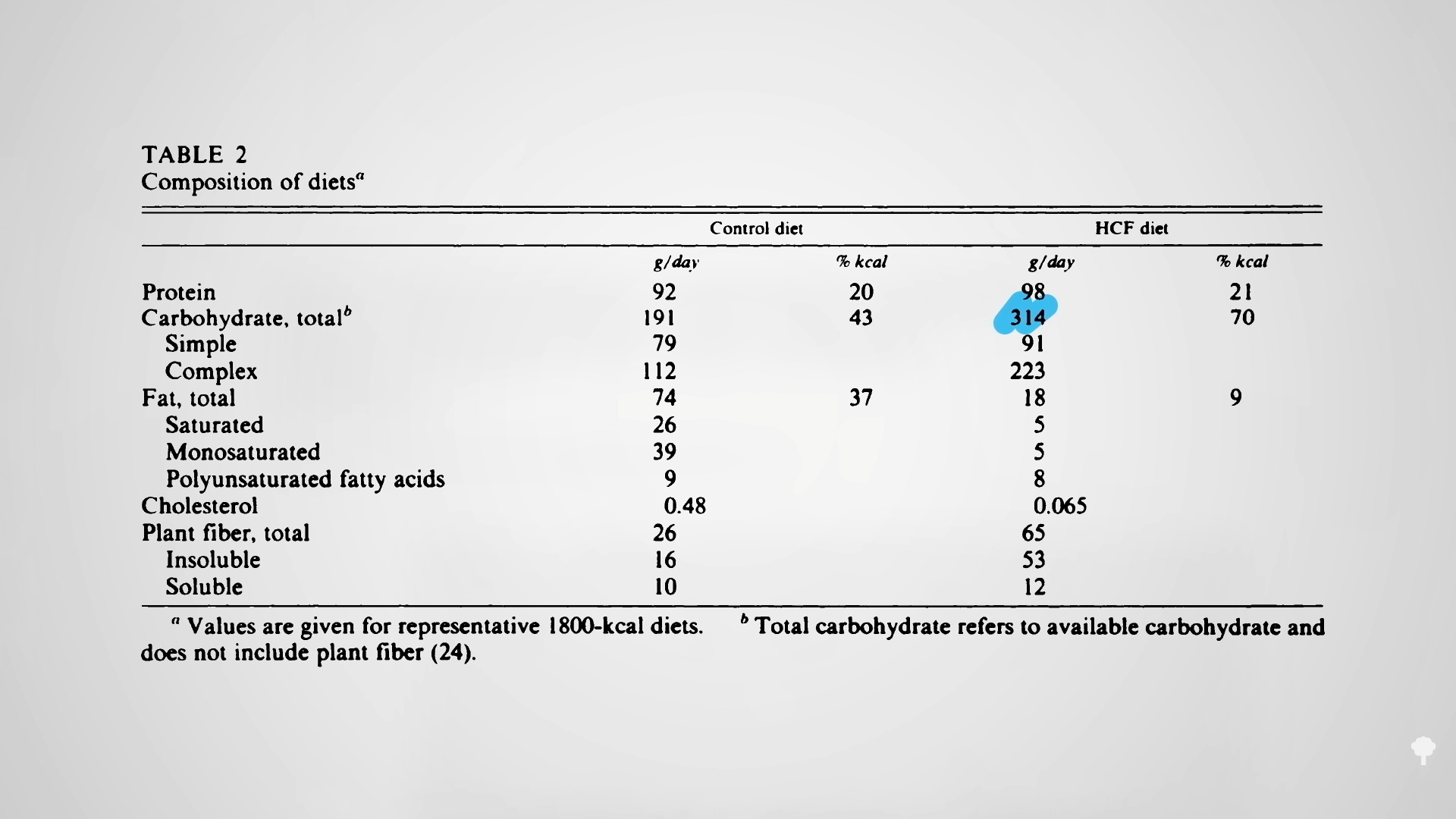 The irony doesn’t stop there. One of the reasons people with diabetes suffer such nerve and artery damage is due to an inflammatory metabolic toxin known as methylglyoxal, which forms at high blood sugar levels. Methylglyoxal
The irony doesn’t stop there. One of the reasons people with diabetes suffer such nerve and artery damage is due to an inflammatory metabolic toxin known as methylglyoxal, which forms at high blood sugar levels. Methylglyoxal