[ad_1]
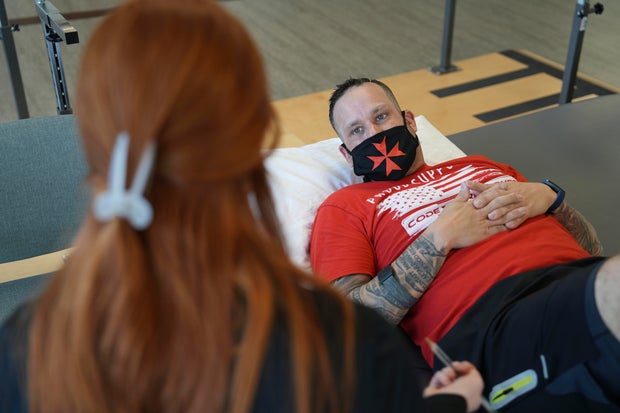
Firefighter and paramedic Mike Camilleri once had no trouble hauling heavy gear up ladders. Now battling long COVID, he gingerly steps onto a treadmill to learn how his heart handles a simple walk.
“This is, like, not a tough-guy test so don’t fake it,” warned Beth Hughes, a physical therapist at Washington University in St. Louis.
Somehow, a mild case of COVID-19 set off a chain reaction that eventually left Camilleri with dangerous blood pressure spikes, a heartbeat that raced with slight exertion, and episodes of intense chest pain.
He’s far from alone. How profound a toll COVID-19 has taken on the nation’s heart health is only starting to emerge, years into the pandemic.
“We are seeing effects on the heart and the vascular system that really outnumber, unfortunately, effects on other organ systems,” said Dr. Susan Cheng, a cardiologist at Cedars-Sinai Medical Center in Los Angeles.
It’s not only an issue for long COVID patients like Camilleri. For up to a year after a case of COVID-19, people may be at increased risk of developing a new heart-related problem, anything from blood clots and irregular heartbeats to a heart attack –- even if they initially seem to recover just fine.
Among the unknowns: Who’s most likely to experience these aftereffects? Are they reversible — or a warning sign of more heart disease later in life?
“We’re about to exit this pandemic as even a sicker nation” because of virus-related heart trouble, said Washington University’s Dr. Ziyad Al-Aly, who helped sound the alarm about lingering health problems. The consequences, he added, “will likely reverberate for generations.”
Angie Wang / AP
Heart disease has long been the top killer in the nation and the world. But in the U.S., heart-related death rates had fallen to record lows in 2019, just before the pandemic struck.
COVID-19 erased a decade of that progress, Cheng said.
Heart attack-caused deaths rose during every virus surge. Worse, young people aren’t supposed to have heart attacks but Cheng’s research documented a nearly 30% increase in heart attack deaths among 25- to 44-year-olds in the pandemic’s first two years.
An ominous sign the trouble may continue: High blood pressure is one of the biggest risks for heart disease and “people’s blood pressure has actually measurably gone up over the course of the pandemic,” she said.
Cardiovascular symptoms are part of what’s known as long COVID, the catchall term for dozens of health issues including fatigue and brain fog. The National Institutes of Health is beginning small studies of a few possible treatments for certain long COVID symptoms, including a heartbeat problem.
But Cheng said patients and doctors alike need to know that sometimes, cardiovascular trouble is the first or main symptom of damage the coronavirus left behind.
“These are individuals who wouldn’t necessarily come to their doctor and say, ‘I have long COVID,’” she said.
In St. Louis, Camilleri first developed shortness of breath and later a string of heart-related and other symptoms after a late 2020 bout of COVID-19. He tried different treatments from multiple doctors to no avail, until winding up at Washington University’s long COVID clinic.
“Finally a turn in the right direction,” said the 43-year-old Camilleri.
There, he saw Dr. Amanda Verma for worsening trouble with his blood pressure and heart rate. Verma is part of a cardiology team that studied a small group of patients with perplexing heart symptoms like Camilleri’s, and found abnormalities in blood flow may be part of the problem.
How? Blood flow jumps when people move around and subsides during rest. But some long COVID patients don’t get enough of a drop during rest because the fight-or-flight system that controls stress reactions stays activated, Verma said.
Some also have trouble with the lining of their small blood vessels not dilating and constricting properly to move blood through, she added.
Hoping that helped explain some of Camilleri’s symptoms, Verma prescribed some heart medicines that dilate blood vessels and others to dampen that fight-or-flight response.
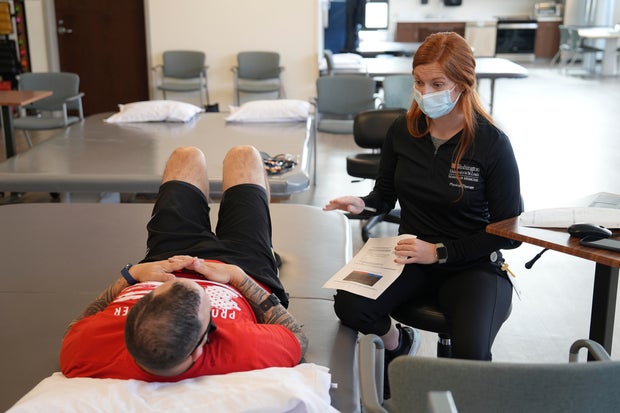
Back in the gym, Hughes, a physical therapist who works with long COVID patients, came up with a careful rehab plan after the treadmill test exposed erratic jumps in Camilleri’s heart rate.
“We’d see it worse if you were not on Dr. Verma’s meds,” Hughes said, showing Camilleri exercises to do while lying down and monitoring his heart rate. “We need to rewire your system” to normalize that fight-or-flight response.
Camilleri said he noticed some improvement as Verma mixed and matched prescriptions based on his reactions. But then a second bout with COVID-19 in the spring caused even more health problems, a disability that forced him to retire.
Angie Wang / AP
How big is the post-COVID heart risk? To find out, Al-Aly analyzed medical records from a massive Veterans Administration database. People who’d survived COVID-19 early in the pandemic were more likely to experience abnormal heartbeats, blood clots, chest pain and palpitations, even heart attacks and strokes up to a year later compared to the uninfected. That includes even middle-aged people without prior signs of heart disease
Based on those findings, Al-Aly estimated 4 of every 100 people need care for some kind of heart-related symptom in the year after recovering from COVID-19.
Per person, that’s a small risk. But he said the pandemic’s sheer enormity means it added up to millions left with at least some cardiovascular symptom. While a reinfection might still cause trouble, Al-Aly’s now studying whether that overall risk dropped thanks to vaccination and milder coronavirus strains.
More recent research confirms the need to better understand and address these cardiac aftershocks. An analysis this spring of a large U.S. insurance database found long COVID patients were about twice as likely to seek care for cardiovascular problems including blood clots, abnormal heartbeats or stroke in the year after infection, compared to similar patients who’d avoided COVID-19.
A post-infection link to heart damage isn’t that surprising, Verma noted. She pointed to rheumatic fever, an inflammatory reaction to untreated strep throat –- especially before antibiotics were common — that scars the heart’s valves.
“Is this going to become the next rheumatic heart disease? We don’t know,” she said.
But Al-Aly says there’s a simple take-home message: You can’t change your history of COVID-19 infections but if you’ve ignored other heart risks –- like high cholesterol or blood pressure, poorly controlled diabetes or smoking -– now’s the time to change that.
“These are the ones we can do something about. And I think they’re more important now than they were in 2019,” he said.
[ad_2]