[ad_1]
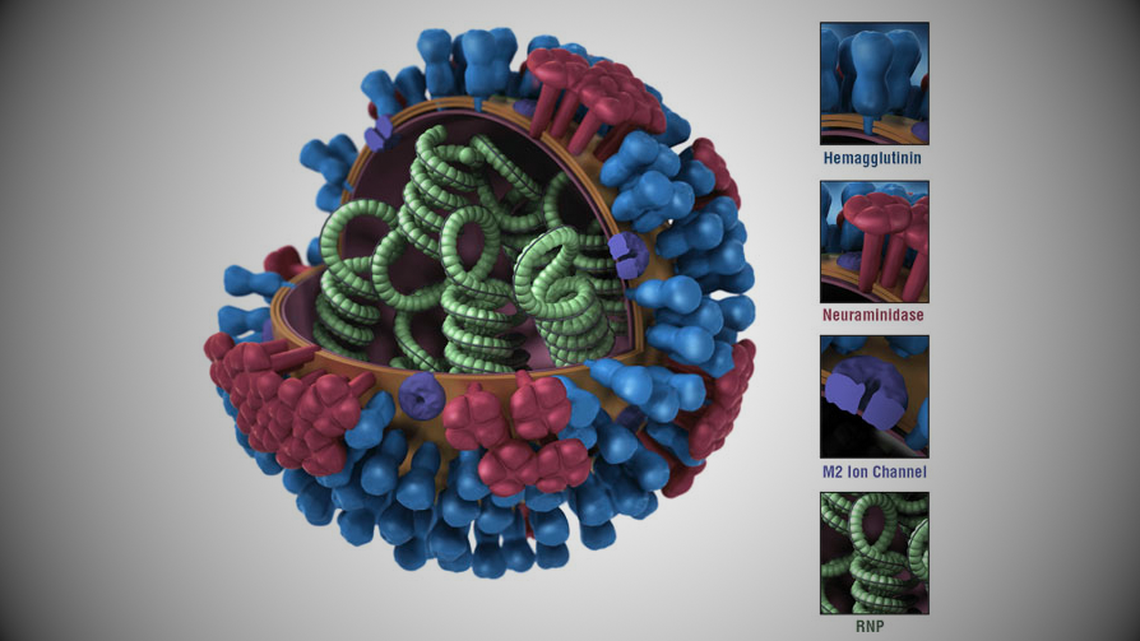
Influenza A virus.
CDC
If it feels like everyone around you is getting sick right now, you’re not imagining it.
Texans are dealing with an early wave of fevers, body aches, and that wiped-out feeling that makes you want to stay in bed for days.
The tricky part is that symptoms look a lot like COVID, allergies, or even just a bad cold, so people aren’t sure what they’ve actually caught.
Doctors say the flu is the main illness showing up in clinics right now, and it’s spreading quicker than usual for this time of year.
Here’s what to know about the variant that’s circulating and how to protect yourself from getting sick.
Which flu variant is spreading across Texas right now?
Health officials say a new version of influenza A is driving the spike in sickness across Texas and the rest of the country right now.
Tarrant County Public Health reported a 256 percent increase in flu positivity on rapid tests between Dec. 6 and Dec. 20, according to an alert Dec. 31. Hospital admissions for the flu also increased from 0.7 percent to 5.4 percent in that same span of time, TCPH said.
Furthermore, national CDC data shows 8.1 percent of lab tests came back positive for flu in early December, and most of those samples were influenza A, specifically the H3N2 strain that doctors are seeing most this season.
A newer offshoot of that strain, called subclade K, is showing up more often and may be part of the reason so many people are getting sick so quickly.
Dr. Jeffrey Kahn, chief of infectious diseases at Children’s Health and pediatrics professor at UT Southwestern, told our news partners at WFAA that many patients go from “feeling well, and then six hours later you feel like you’ve been hit by a truck. You’ve got a high fever. You can’t get out of bed. It’s the worst feeling you’ve ever had in your life.”
Which symptoms should I watch for this season?
Experts say the most common signs include fever, chills, body aches, headaches, cough, congestion and that sudden wave of exhaustion that makes it hard to get out of bed.
Many people also report feeling too weak or fatigued to keep up with daily routines.
Some of these symptoms overlap with COVID and RSV, which is part of why people are confused about what they’ve actually caught.
The CDC says you can’t always tell the difference based on symptoms alone, especially when fever and body aches are present. Testing is the only way to know for sure, and doctors say it can help guide treatment if symptoms get worse.
How serious is the flu this season in Texas?
Flu activity is higher than usual for this point in the winter, according to the Texas Department of State Health Services.
More than 5,000 Texans visited hospitals or clinics for influenza like illness during the most recent reporting period, which is more than double what the state saw around this time last year.
Influenza A is making up the majority of lab confirmed cases.
The CDC reports that hospitalizations have also increased nationally, with adults 65 and older seeing the biggest jump in flu-related admissions.
That trend mirrors what doctors in North Texas are seeing. Older adults, young children, and people with chronic health conditions remain at the highest risk for complications like pneumonia or dehydration.
Although most people recover at home within several days, health officials urge Texans to take flu symptoms seriously.
If you have trouble breathing, persistent chest pain, prolonged fever, or signs of dehydration, the CDC recommends seeking medical care right away.
How can I protect myself from the flu?
Doctors say consistent everyday habits are some of the most effective ways to avoid getting sick.
According to the CDC, washing your hands often, using hand sanitizer when soap and water aren’t available, and cleaning high touch surfaces like phones, doorknobs, and countertops can help limit the spread of the virus.
It also helps to avoid touching your eyes, nose, and mouth since flu viruses spread when people transfer germs from surfaces to their faces.
If you’re feeling sick, the CDC recommends staying home until your fever has been gone for at least 24 hours without medication.
Should I still get a flu shot if a new variant is spreading?
Yes. The CDC says flu shots remain the best way to lower your chances of severe illness, even when a new version of the virus is circulating.
This year’s vaccine targets three strains of flu, including two influenza A viruses and one influenza B virus.
While the circulating subclade K strain has some differences from the virus used to design the shot, health officials say the vaccine can still help reduce symptoms and keep people out of the hospital.
The CDC notes that it takes about two weeks for your body to build protection after getting vaccinated, so getting the shot now can still help as flu activity continues through the winter months.
Vaccination is especially important for adults 65 and older, young children, pregnant people and anyone with underlying conditions.
Where can I get a low-cost or free flu shot in Texas?
Most major pharmacies offer flu shots at no cost with insurance, according to the CDC.
Places like CVS, Walgreens, HEB, Kroger and Walmart usually take walk-ins, and many clinics allow you to book appointments online.
If you don’t have insurance, you still have options. Local health departments often provide low-cost flu shots for adults, and some community clinics offer them for free during the winter months.
You can call your county health department or check their website to see where walk in or low cost vaccination events are happening.
This story was originally published December 31, 2025 at 11:29 AM.
[ad_2]
Tiffani Jackson
Source link