[ad_1]
Because the gut microbiome can recover (with targeted nutrition & time).
[ad_2]
[ad_1]
What does the gut have to do with developing Parkinson’s disease?
Parkinson’s disease is an ever-worsening neurodegenerative disorder that results in death and affects about 1 in 50 people as they get older. A small minority of cases are genetic, running in families, but 85% to 90% of cases are sporadic, meaning they seem to pop up out of nowhere. Parkinson’s is caused by the death of a certain kind of nerve cell in the brain. Once about 70% of them are gone, the symptoms start. What kills off those cells? It still isn’t completely clear, but the abnormal clumping of a protein called alpha-synuclein or α-synuclein is thought to be involved. Why? Researchers injected blended Parkinson’s brains into the heads of rats and monkeys, and Parkinson’s pathology and symptoms were induced. It can even happen when injecting just the pure, clumped α-synuclein strands themselves. How, though, do these clumps naturally end up in the brain?
As I discuss in my video The Role Meat May Play in Triggering Parkinson’s Disease, it all seems to start in the gut. The part of the brain where the pathology often first appears is directly connected to the gut, and we have direct evidence of the spread of Parkinson’s pathology from the gastrointestinal (GI) tract to the brain: α-synuclein from brains of Parkinson’s patients is taken up in the gut wall and creeps up the vagal nerves from the gut into the brain—at least that was the case in rats. If only we could go back and look at people’s colons before they got Parkinson’s. Indeed, we can. Old colon biopsies from people who would later develop Parkinson’s were dredged up, and, years before symptoms arose, you could see the α-synuclein in their gut.
Research supported by the Michael J. Fox Foundation has found that you can reliably distinguish the colons of patients from controls by the presence of this Parkinson’s protein lodged in the gut wall. But how did it get there in the first place? Are “vertebrate food products…a potential source of prion-like α-synuclein”? Indeed, nearly all the animals with backbones that we consume—cows, chickens, pigs, and fish—express the protein α-synuclein. So, when we eat common meat products, when we eat skeletal muscle, we’re eating nerves, blood cells, and the muscle cells themselves. Every pound of meat contains, on average, half a teaspoon of blood, and that alone could be an α-synuclein source to potentially trigger a clumping cascade of our own α-synuclein in the gut. Though “it may seem intuitive that dietary α-synuclein could seed aggregation in the gut,” this kind of buildup, what evidence do we have that it’s actually happening?
We have some pretty interesting data. There’s a surgical procedure called a vagotomy, in which the big nerve that goes from our gut to our brain—the vagus nerve—is cut as an old-timey treatment for stomach ulcers. Would cutting communication between the gut and the brain reduce Parkinson’s risk? Apparently so, suggesting that the gut to brain’s vagal nerve may be critically involved in the development of Parkinson’s disease.
Of course, “many people regularly consume meat and dairy products, but only a small fraction of the general population will develop PD,” Parkinson’s disease. So, there must be other factors at play that “may provide an opportunity for unwanted dietary α-synuclein to enter the host, and initiate disease.” For example, our gut becomes leakier as we age, so might that play a role? What else makes our gut leaky? “Dietary fiber deprivation has also been shown to degrade the intestinal barrier and enhance pathogen entry.” So, this raises “possibilities for food-based therapies.”
Parkinson’s patients have significantly less Prevotella in their gut, a friendly fiber-eating flora that bolsters our intestinal barrier function. So, low levels of Prevotella are linked to a leaky gut, which has been linked to intestinal α-synuclein deposition, but fiber-rich foods may bring Prevotella levels back up. “Therefore, it is possible that by adopting a plant-based diet, in addition to the beneficial effects of phytonutrients, increasing overall fiber intake may modify gut microbiota and gut permeability [leakiness] in beneficial ways for people with PD.”
So, does a vegan diet—one with lots of fiber and no meat—reduce risk for Parkinson’s? Parkinson’s “appears to be rare in quasi-vegan cultures,” with rates that are about five times lower in rural sub-Saharan Africa, for instance. All this time, we were thinking the benefits seen for Parkinson’s from plant-based diets were due to the antioxidants and anti-inflammatory nature of the animal-free diets, but maybe it’s also due to the increased intestinal exposure to fiber and decreased intestinal exposure to ingested nerves, muscles, and blood.
Wasn’t that fascinating? For more on Parkinson’s, see the related posts below.
[ad_2]
Michael Greger M.D. FACLM
Source link
[ad_1]
Bloating is uncomfortable and frustrating. Not to mention it can derail your confidence and plans for the day. Everyone has different triggers when it comes to bloat. For example, I feel it most when I eat too quickly. Others feel it from not having a regular No 2. schedule.
[ad_2]
[ad_1]
Just about everyone gets, ahem, backed up—aka, constipation—occasionally. For many people, however, constipation can turn into a constant nightmare. Thankfully, a handy evidence-based guide out this week highlights the foods and dietary supplements most likely to help you smooth out your bathroom trips.
Researchers in the UK compiled the guide, following an extensive review of the medical literature. Kiwis, rye bread, and fiber supplements were some of the items that had clear evidence supporting their use for chronic constipation, the researchers found. The conclusions, endorsed by the British Dietetic Association, represent the first rigorous dietary guidelines for managing this frustrating health condition, the authors say.
“Chronic constipation can have a huge impact on someone’s day-to-day life,” said lead author Eirini Dimidi, a nutrition researcher at King’s College London, in a statement from the university. “For the first time, we’ve provided direction on what dietary approaches could genuinely help, and which diet advice lacks evidence.”
Estimates vary, but around 16% of the world’s population is thought to currently have constipation, while chronic constipation may affect between 9% and 20% of adults in the U.S. Constipation is also known to become more common as we age, affecting between a quarter and a third of people over 65.
Most cases of chronic constipation aren’t linked to a single known cause, such as a disease, but there are factors that raise the risk of it happening, including lifestyle habits like our diet.
Medical guidelines in the past have emphasized generalized tips for handling constipation, such as eating a diet rich in fiber. But the study researchers say their work is intended to pinpoint the specific foods and supplements that have the most scientific backing for treating constipation.
The researchers conducted four separate systematic reviews, which collectively analyzed data from 75 randomized and controlled clinical trials. The findings from this review were then used to create guidelines through an approach called the Grading of Recommendations, Assessment, Development and Evaluation, or GRADE, system.
One important aspect of the GRADE system is that it classifies the level of evidence supporting a particular recommendation as well as the strength of a recommendation, meaning how helpful it would be to people. A strong recommendation in this case, for instance, would mean that most everyone with chronic constipation would likely benefit from following it. The proposed recommendations were also evaluated and decided on by a panel of relevant experts in the field (this is known as a Delphi consensus).
The guidelines were jointly published in two journals, the Journal of Human Nutrition & Dietetics as well as Neurogastroenterology & Motility.
All in all, the researchers came up with 59 recommendations.
The supplements most strongly recommended for constipation in the guidelines are psyllium fiber supplements, magnesium oxide supplements, and probiotics (though it’s still unclear which specific strains might be best).
As for specific foods, the list goes: kiwifruits, rye bread, and high-mineral water.
Interestingly, the authors failed to find sturdy enough evidence to support any whole diet approach, including high-fiber diets. While it’s still possible that eating lots of fiber could prevent or manage chronic constipation, the researchers say better-quality studies are needed to know for sure. It’s also worth noting that high-fiber diets are thought to have many health benefits, so there’s no reason to feel worried if you already include plenty of fiber in your meals.
The researchers argue more extensive research should still be done to suss out the optimal treatments or interventions for constipation, since many of the studies they reviewed were low quality. But as is, their recommendations can already help people dealing with constipation, they say.
“Being able to improve this condition through dietary changes would allow people to self-manage their symptoms more and, hopefully, improve their quality of life,” said Dimidi.
[ad_2]
Ed Cara
Source link
[ad_1]
If you type “dates” into TikTok’s search bar, you’ll find plenty of ideas for a night of romance. You might also see a variety of recipes using the sweet, wrinkly, brown dried fruit. That’s because dates, the edible ones, are having a moment.
U.S. searches for “Medjool dates,” a particularly plump variety, hit a 20-year high in March of this year, according to Google Trends. And the searches aren’t just the result of a passing curiosity: Consumers are actually spending. U.S. retail sales of dates jumped about 30 percent in the 52-week period ending on July 13 compared with the year before, according to data from Circana, a market research firm. In 2024, sales increased nearly 19 percent over the prior year, Circana found. And over the past few years, dates have popped up as the hero in wellness-focused snacks.
“The Medjool is the Cadillac of dates,” said George Jeffrey, owner of Pacific Date Corporation, a grower, packer, and shipper of dates, as well as a snack manufacturer, based in Thermal, California. “It’s a pretty nice, large piece of fruit with a nice caramel flavor. And it’s having its day in the sun.” Last year, Pacific handled 17 million pounds of dates, said Jeffrey, seven million of them Medjools. Jeffrey expects growth next year. And recently, Pacific has decided to make date snacks of its own.
“We did a lot of co-manufacturing for other big date brands that were out there,” Jeffrey said, referring to contract manufacturing. “And we said, ‘Why are we doing that for everybody else? We should have our own brand.’” Sun Lovin’ Foods, which makes date-based energy bites in flavors like chocolate cherry and banana nut, launched in 2023. “It’s working very well,” Jeffrey said, noting that about 2,000 retailers are now carrying Sun Lovin’ snacks.
Jeffery is not the only farmer making the most of the fruit’s recent spike in popularity. Others, from small consumer-facing brands to players that operate behind the scenes, are marketing their own products and coming up with ways to keep the momentum going.
Their speed is “astounding to me,” says Jonna Parker, vice president of fresh foods at Circana, especially because farmers typically don’t do much marketing of their own products.
The demand means that some farmers are expanding, a welcome reversal from the national trend. “We’re going to expand on our facility here because we’ve outgrown it,” said Jeffrey. For Pacific, that means more equipment used to freeze and grade Medjools.
Meanwhile, Double Date Packing, a Medjool date grower in Coachella, California, has “been buying up ranches wherever we can,” says Hope Barbee, vice president of sales at the company. “We’ve been selling out of our fruit for the past two years straight.”
Dates are an ancient fruit with particular significance for Middle Eastern cultures. But that’s not why they’re going viral on TikTok. Foods that gain traction on social media often have a specific nutritional edge: Cottage cheese, for example, is packed with protein. Grapes are a low-calorie way to get your (natural) sugar fix. Dates are full of fiber, which is “one of the biggest trends right now,” Parker said. On social media, attempts to increase fiber intake have been dubbed “fibermaxxing,” and fibermaxxing recipes are readily available on TikTok.
The fruit has also become more visible as an ingredient in trendy packaged snacks. RX Bars, a protein bar company started in 2013, lists just a few ingredients prominently on its label, and dates are almost always among them. Over the past few years, companies like Date Better, Gato Dates, and Realsy have emerged with a focus on date-based snacks. Others, like Spring & Mulberry, are using dates to sweeten chocolate. Online, creators showcase date-heavy recipes for home-made versions of energy bars, caramels, candy bars, and more.
Rebecca Seitz, co-owner of the food and gifts retailer Sphinx Date Co. in Scottsdale, Arizona, suspects that social media has helped drive growth at her store, which specializes in dates. “They’re really simple recipes … just taking some dates and some nuts and making little energy bars,” she says. That’s “what makes it ideal for social media.” Over the past decade, Sphinx’s total sales have grown about 6.5 percent per year on average, Seitz says.
Sphinx Date Co. sells Medjool dates on their own and in gift trays or boxes. It also stocks less traditional products, like salsa and hot sauce made with dates as a sweetener. The goal is to “give an idea of the way you can use [dates] in savory applications,” said Seitz. “Lots of people come back for it,” she added. Items like that can be a boon for farmers, as well.
“People are seeing new opportunities to use dates,” said Kristy Kneiding, manager of the state-run California Date Commission. That means “growers and packers are being able to convert [dates into] … date paste, date syrup, date-based snacks – and that actually provides a good outlet for the dates that don’t look so pretty and don’t qualify under our whole fruit standard.”
An unexpected increase in demand can be stressful. This year, Pacific Date has gotten forecasts from ingredient customers showing a 35 percent spike in orders month-over-month, according to Jeffrey. “I didn’t plan for this increase,” he said. If Pacific Date can’t source dates locally, it may have to import dates and contend with any relevant tariffs. Still, he said, “we’re all excited as date farmers, and happy that things are trending up.”
Generally, higher interest in dates and date products offers some “economic stability” in a notoriously unreliable business, Kneiding noted. “All farmers across the board are at mother nature’s mercy.” Stormy weather, for example, can destroy crops, eating into farmers’ sales. Strong demand, in these cases, may help.

For the commission, which collects fees based on sales, higher revenue means more funding for key initiatives, like government relations, research, and marketing. Last year, it partnered with the American Diabetes Association to spread awareness around how dates can fit into diabetic-friendly diets. “By being able to expand our marketing and branding, we’re able to also educate our consumers,” Kneiding said. This year it’s focusing on influencer marketing, among other initiatives.
State-operated groups can help raise awareness for agricultural products overall. But packaged goods companies – or growers themselves – have to set their own items apart.
About 10 years ago, when Joan Smith decided to start Rancho Meladuco Date Farm, she was already thinking about how to make people notice her dates. At the time, she observed that most date “packaging was unremarkable,” Smith recalled. She wanted Rancho Meladuco to stand out. To that end, her products are sold in tubs and boxes that feature bold designs, recipe recommendations, and, sometimes, maps of California, where the small farm is located.
With that ethos in place, Smith started pitching. “Right after launch, I used Instagram to start reaching out to different people in the food editorial space,” she recalled. Her efforts helped land Rancho Meladuco’s products on gift guides, including one published by The Wall Street Journal. Rancho Meladuco also joined the Specialty Food Association, a trade group that puts on regular shows where small businesses can meet retailers. And it’s taking part in the current online frenzy, posting recipes for frozen ice cream bars, Medjool date turtles, and more on its social media accounts.
Others brought fresh ideas to older businesses. Aziz Farms, which sells dates to wholesalers, began to market, ship, and brand its own products when owner Mark Tadros joined the family business about 18 years ago. Some of the changes Tadros made included “building a brand, designing packaging that popped and felt right, and then telling a story along with it,” he said. The Aziz Farms logo includes palm trees, camels, and pyramids, references to Tadros’s father’s home country of Egypt. Aziz Farms started packing Medjool dates around 11 years ago, Tadros said. At the time, it sold 42,000 pounds of Medjools per year – today, it’s up to 1.5 million pounds annually.
For Tadros and others like him, date farming is more than just a job. “I saw what my father had built,” he says, and “I felt like we had an opportunity to grow it in a way that would solidify his legacy in this industry.”
As he looks ahead, Tadros sees the importance of educating young consumers about small farms like his. “We do a lot of education activities, school field trips, programs like that,” he explains. “I’m hoping that we see a world where people are willing to pay more for produce that is closer to them,” helping to make local farming more sustainable.
“We’ve got a very optimistic outlook,” he adds. “It’s just staying the course.”
[ad_2]
Danielle Wiener-Bronner
Source link
[ad_1]
If you’re training more, whether you’re logging longer runs, lifting heavier, or simply moving more throughout the week, your calorie, fat, and fiber intake should rise accordingly. Otherwise, you could be increasing your risk of stress injuries, poor recovery, or long-term hormonal disruptions without realizing it.
[ad_2]
[ad_1]
The season of pumpkin pie this and pumpkin spice that is upon us. And as a dietitian, I’m all for adding more pumpkin to your day—it is a vegetable after all! This veggie naturally has a mildly sweet taste, but so many pumpkin recipes are geared for breakfast. While these foods may satisfy your sweet tooth, they will surely spike your blood sugar and leave you feeling hungry (yet again) within the hour.
[ad_2]
[ad_1]
Eating a fiber-rich diet is linked to numerous health benefits1
[ad_2]
[ad_1]
If you struggle with going No. 2 daily, you aren’t alone. In fact, about 16% of people (and 33% of folks over 60) have difficulty going more than once every three days! And (as I’m sure you know) that can get really uncomfortable—think bloating and a distended stomach.
[ad_2]
[ad_1]
Much like the fact that some people greet each day bright-eyed and bushy-tailed while others are confirmed night owls, we don’t all arise with the same level of hunger in our bellies. It never fails that, between spouses or roommates, one person wakes up ravenous while the other could take or leave breakfast. What’s that about?
[ad_2]
[ad_1]
As with many things nutrition-related, sometimes it seems like the guidance around meal timing ping-pongs back and forth between contradictory recommendations. “Eat three square meals a day.” “No, eat six small meals per day.” “Wait several hours between meals.” “Go ahead and graze all day!” It’s enough to make you wonder whether there are any trustworthy parameters around meal timing at all.
[ad_2]
[ad_1]
It may not be the number of bacteria growing in our small intestine, but the type of bacteria, which can be corrected with diet.
When researchers tested more than a thousand patients suffering for longer than six months from symptoms typical with irritable bowel syndrome (IBS), such as excess gas, bloating, diarrhea, and abdominal pain, but who do not appear to have anything more serious going on, like inflammatory bowel disease, a significant percentage were found to be suffering from lactose intolerance—intolerance to the milk sugar lactose. In infancy, we have an enzyme called lactase in our small intestine that digests milk sugar, but, understandably, most of us lose it after weaning. “Although genetic mutation has led to persistence of lactase in adults, about 75% of the world’s population malabsorbs lactose after age 30” and have lactose intolerance. However, a third of the patients were diagnosed with small intestinal bacterial overgrowth (SIBO).
“The evidence for SIBO and IBS is shrouded in controversy, predominantly because of the fact that the [breath] tests used in clinical practice to diagnose SIBO are not valid,” as I’ve explored before. As well, the implications of having more versus fewer bacteria growing in the small intestine are unclear since the number doesn’t seem to correlate with the symptoms. It turns out it isn’t the number of bugs growing in the small intestine, but the type of bugs. So, it’s “small intestinal microbial dysbiosis”—not overgrowth in general, but the wrong kind of growth—that appears to underlie symptoms associated with functional gastrointestinal disorders, like IBS.
How can we prevent this from happening? The symptoms appear to be correlated with a significant drop in the number of Prevotella. Remember them? Prevotella are healthy fiber feeders, “suggestive of a higher fiber intake in healthy individuals,” while the bugs found more in symptomatic patients ate sugar, which “may reflect a higher dietary intake of simple sugars.” However, correlation doesn’t mean causation. To prove cause and effect, we have to put it to the test, which is exactly what researchers did.
“Switching a group of healthy individuals who habitually ate a high-fibre diet (>11g per 1,000 calories) to a low-fibre diet (<10g per day) containing a high concentration of simple sugars for 7 days produced striking results. First, 80% developed de novo [new] gastrointestinal symptoms such as bloating and abdominal pain that resolved on resumption of their habitual high-fibre diet. Second, diet-related changes in the small intestinal microbiome were predictive of symptoms (such as bloating and abdominal discomfort) and linked to an alteration in duodenal [intestinal] permeability.” In other words, they developed a leaky gut within seven days. And, while some went from SIBO positive to SIBO negative and others from SIBO negative to SIBO positive, it didn’t matter because the number of bacteria growing didn’t correlate with symptoms. It was the type of bacteria growing, as you can see below, and at 3:12 in my video Fiber vs. Low FODMAP for SIBO Symptoms.
No wonder their guts got leaky. Levels of short-chain fatty acids plummeted. Those are the magical by-products our good gut bugs make from fiber, which “play an important role in epithelial [intestinal] barrier integrity,” meaning they keep our gut from getting leaky.
So, while we don’t have sound data to suggest that something like a low FODMAP diet has any benefit for patients with SIBO symptoms, there have been more than a dozen randomized controlled trials that have put fiber to the test. Overall, researchers found there was a significant improvement in symptoms among those randomized to increase their fiber intake. That may help explain why “high-fiber, plant-based diets can prevent many diseases common in industrialized societies.” Such diets have this effect “on the composition and metabolic activity of the colonic microbiota.” Our good gut bugs take plant residues like fiber and produce “health-promoting and cancer-suppressing metabolites” like short-chain fatty acids, which have profound anti-inflammatory properties. “All the evidence points to a physiological need for ~50 g fiber per day, which is the amount contained in the traditional African diet and associated with the prevention of westernized diseases.” That is approximately twice the typical recommendation and three times more than what most people get on a daily basis. Perhaps it should be no surprise that we need so much. Even though we split from chimpanzees millions of years ago, “there is still broad congruency” in the composition of our respective microbiomes to this day. While they’re still eating their 98 to 99 percent plant-based diets to feed their friendly flora with fiber, we’ve largely removed fiber-rich foods from our food supply.
[ad_2]
Michael Greger M.D. FACLM
Source link
[ad_1]
I debunk the myth of protein as the most satiating macronutrient.
The importance of satiety is underscored by a rare genetic condition known as Prader-Willi syndrome. Children with the disorder are born with impaired signaling between their digestive system and their brain, so they don’t know when they’re full. “Because no sensation of satiety tells them to stop eating or alerts their body to throw up, they can accidentally consume enough in a single binge to fatally rupture their stomach.” Without satiety, food can be “a death sentence.”
Protein is often described as the most satiating macronutrient. People tend to report feeling fuller after eating a protein-rich meal, compared to a carbohydrate- or fat-rich one. The question is: Does that feeling of fullness last? From a weight-loss standpoint, satiety ratings only matter if they end up cutting down on subsequent calorie intake, and even a review funded by the meat, dairy, and egg industries acknowledges that this does not seem to be the case for protein. Hours later, protein consumed earlier doesn’t tend to end up cutting calories later on.
Fiber-rich foods, on the other hand, can suppress appetite and reduce subsequent meal intake more than ten hours after consumption—even the next day—because their site of action is 20 feet down in the lower intestine. Remember the ileal brake from my Evidence-Based Weight Loss lecture? When researchers secretly infused nutrients into the end of the small intestine, study participants spontaneously ate as many as hundreds fewer calories at a meal. Our brain gets the signal that we are full, from head to tail.
We were built for gluttony. “It is a wonderful instinct, developed over millions of years, for times of scarcity.” Stumbling across a rare bounty, those who could fill themselves the most to build up the greatest reserves would be more likely to pass along their genes. So, we are hard-wired not just to eat until our stomach is full, but until our entire digestive tract is occupied. Only when our brain senses food all the way down at the end does our appetite fully dial down.
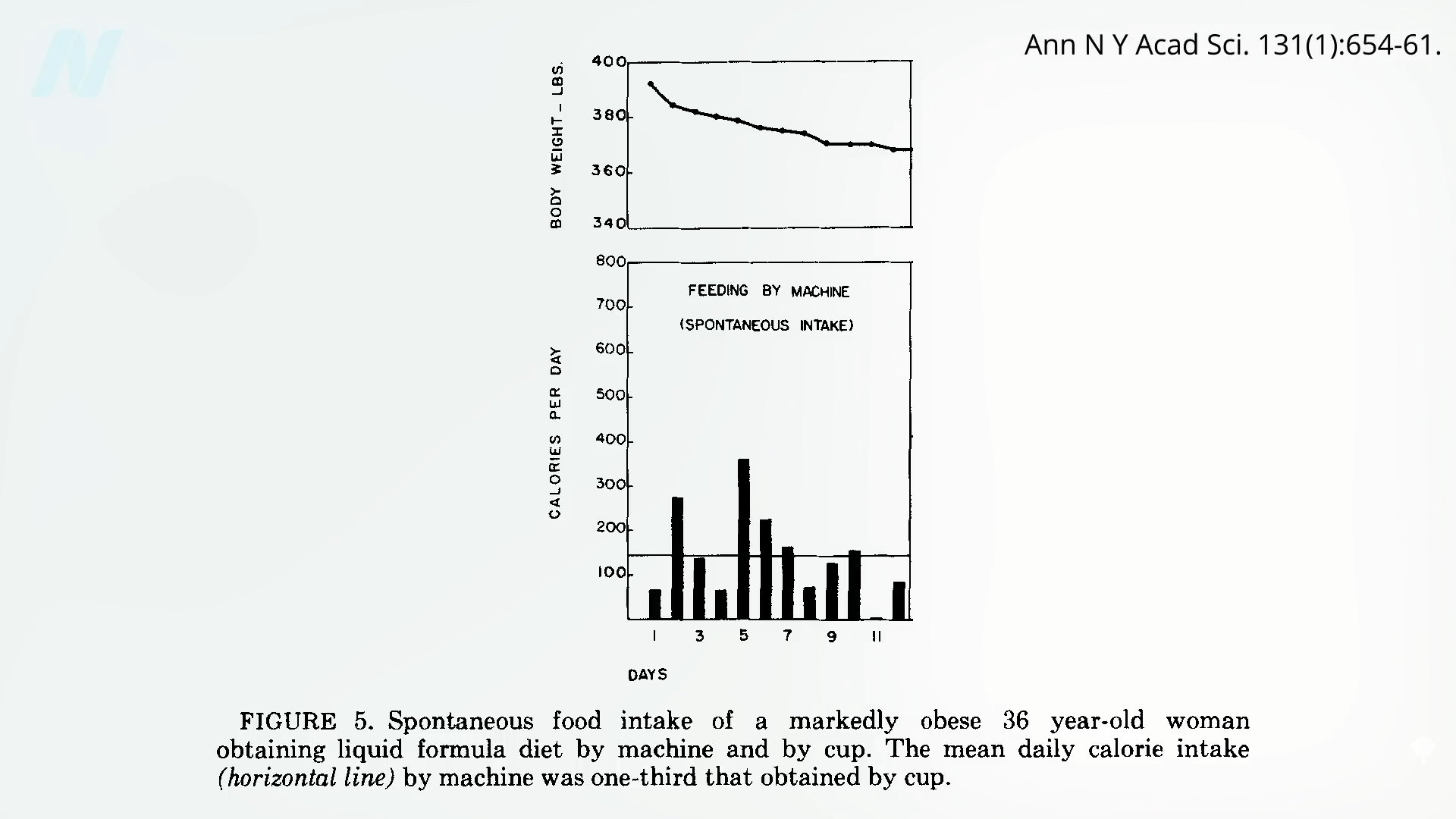
Fiber-depleted foods get rapidly absorbed early on, though, so much of it never makes it down to the lower gut. As such, if our diet is low in fiber, no wonder we’re constantly hungry and overeating; our brain keeps waiting for the food that never arrives. That’s why people who even undergo stomach-stapling surgeries that leave them with a tiny two-tablespoon-sized stomach pouch can still eat enough to regain most of the weight they initially lost. Without sufficient fiber, transporting nutrients down our digestive tract, we may never be fully satiated. But, as I described in my last video, one of the most successful experimental weight-loss interventions ever reported in the medical literature involved no fiber at all, as you can see here and at 2:47 in my video Foods Designed to Hijack Our Appetites.
At first glance, it might seem obvious that removing the pleasurable aspects of eating would cause people to eat less, but remember, that’s not what happened. The lean participants continued to eat the same amount, taking in thousands of calories a day of the bland goop. Only those who were obese went from eating thousands of calories a day down to hundreds, as shown below and at 3:22 in my video. And, again, this happened inadvertently without them apparently even feeling a difference. Only after eating was disconnected from the reward was the body able to start rapidly reining in the weight.
 We appear to have two separate appetite control systems: “the homeostatic and hedonic pathways.” The homeostatic pathway maintains our calorie balance by making us hungry when energy reserves are low and abolishes our appetite when energy reserves are high. “In contrast, hedonic or reward-based regulation can override the homeostatic pathway” in the face of highly palatable foods. This makes total sense from an evolutionary standpoint. In the rare situations in our ancestral history when we’d stumble across some calorie-dense food, like a cache of unguarded honey, it would make sense for our hedonic drive to jump into the driver’s seat to consume the scarce commodity. Even if we didn’t need the extra calories at the time, our body wouldn’t want us to pass up that rare opportunity. Such opportunities aren’t so rare anymore, though. With sugary, fatty foods around every corner, our hedonic drive may end up in perpetual control, overwhelming the intuitive wisdom of our bodies.
We appear to have two separate appetite control systems: “the homeostatic and hedonic pathways.” The homeostatic pathway maintains our calorie balance by making us hungry when energy reserves are low and abolishes our appetite when energy reserves are high. “In contrast, hedonic or reward-based regulation can override the homeostatic pathway” in the face of highly palatable foods. This makes total sense from an evolutionary standpoint. In the rare situations in our ancestral history when we’d stumble across some calorie-dense food, like a cache of unguarded honey, it would make sense for our hedonic drive to jump into the driver’s seat to consume the scarce commodity. Even if we didn’t need the extra calories at the time, our body wouldn’t want us to pass up that rare opportunity. Such opportunities aren’t so rare anymore, though. With sugary, fatty foods around every corner, our hedonic drive may end up in perpetual control, overwhelming the intuitive wisdom of our bodies.
So, what’s the answer? Never eat really tasty food? No, but it may help to recognize the effects hyperpalatable foods can have on hijacking our appetites and undermining our body’s better judgment.
Ironically, some researchers have suggested a counterbalancing evolutionary strategy for combating the lure of artificially concentrated calories. Just as pleasure can overrule our appetite regulation, so can pain. “Conditioned food aversions” are when we avoid foods that made us sick in the past. That may just seem like common sense, but it is actually a deep-seated evolutionary drive that can defy rationality. Even if we know for a fact a particular food was not the cause of an episode of nausea and vomiting, our body can inextricably tie the two together. This happens, for example, with cancer patients undergoing chemotherapy. Consoling themselves with a favorite treat before treatment can lead to an aversion to their favorite food if their body tries to connect the dots. That’s why oncologists may advise the “scapegoat strategy” of only eating foods before treatment that you are okay with, never wanting to eat again.
Researchers have experimented with inducing food aversions by having people taste something before spinning them in a rotating chair to cause motion sickness. Eureka! A group of psychologists suggested: “A possible strategy for encouraging people to eat less unhealthy food is to make them sick of the food, by making them sick from the food.” What about using disgust to promote eating more healthfully? Children as young as two-and-a-half years old will throw out a piece of previously preferred candy scooped out of the bottom of a clean toilet.
Thankfully, there’s a way to exploit our instinctual drives without resorting to revulsion, aversion, or bland food, which we’ll explore next.
[ad_2]
Michael Greger M.D. FACLM
Source link
[ad_1]
Emulsifiers are the most widely used food additives. What are they doing to our gut microbiome?
When grocery shopping these days, unless you’re sticking to the produce aisle, “it is nearly impossible to avoid processed foods, particularly in the consumption of a typical Western diet,” which is characterized by insufficient plant foods, too much meat, dairy, and eggs, and a lot of processed junk, “along with increased exposure to additives due to their use in processed foods.”
The artificial sweetener sucralose, for example, which is sold as Splenda, “irrefutably disrupts the gut microbiome at doses relevant to human use” and “induces glucose intolerance.” In other words, it can make our blood sugars worse instead of better. It’s relatively easy to avoid artificial sweeteners, but “it may be much more difficult to avoid ingestion of emulsifiers…because they are commonly added to a wide variety of foods within the modern Western diet.” In fact, “emulsifiers are the most widely used additives,” and “most processed foods contain one or more emulsifiers that allow such foods to maintain desired textures and avoid separation into distinct parts (e.g, oil and water layers).” We now consume emulsifiers by the megaton every year, thanks to a multibillion-dollar industry, as you can see below and at 1:03 in my video Are Emulsifiers Like Carboxymethylcellulose and Polysorbate 80 Safe?.
Emulsifiers are commonly found in fatty dressings, breads and other baked goods, mayonnaise and other fatty spreads, candy, and beverages. “Like all authorized food additives, emulsifiers have been evaluated by risk assessors, who consider them safe. However, there are growing concerns among scientists about their possible harmful effects on our intestinal barriers and microbiota,” in terms of causing a leaky gut. As well, they could possibly “increase the absorption of several environmental toxins, including endocrine disruptors and carcinogens” present in the food.
We know that the consumption of ultra-processed foods may contribute to weight gain. Healthier, longer-lived populations not only have low meat intake and high plant intake, but they also eat minimally processed foods and “have far less chronic diseases, obesity rates, and live longer disease-free.” Based on a number of preclinical studies, it may be that the emulsifiers found in processed foods are playing a role, but who cares if “emulsifiers make rats gain weight”? When we read that “emulsifiers can cause striking changes in the microbiota,” they aren’t talking about the microbiota of humans.
Often, mice are used to study the impact on the microbiome, but “only a few percent of the bacterial genes are shared between mice and humans.” Even the gut flora of different strains of mice can be considerably different from each other, so if we can’t even extrapolate from one type of mouse to another, how are we supposed to translate results from mice to humans? “Remarkably, there has been little study of the potential harmful effects of ingested…emulsifiers in humans.”
Take lecithin, for example, which is “perhaps best known as a key component of egg yolks.” Lecithin was found to be worse than polysorbate 80 in terms of allowing bacteria to leak through the gut wall into the bloodstream. However, it’s yet to be determined whether lecithin consumption in humans causes the same problem. “There is certainly a paucity in the data of human trials with the effects of emulsifiers in processed foods,” but we at least have data on human tissue, cells, and gut flora.
A study was titled: “Dietary emulsifiers directly alter the human microbiota composition and gene expression ex vivo potentiating intestinal inflammation.” Ex vivo means outside the body. Researchers inoculated an artificial gut with fresh human feces until a stable culture was established, then added carboxymethylcellulose (CMC) or polysorbate 80 (P80), resulting in boosts in proinflammatory potential starting within one day with the carboxymethylcellulose and within the first week with polysorbate 80, as you can see below and at 3:39 in my video.
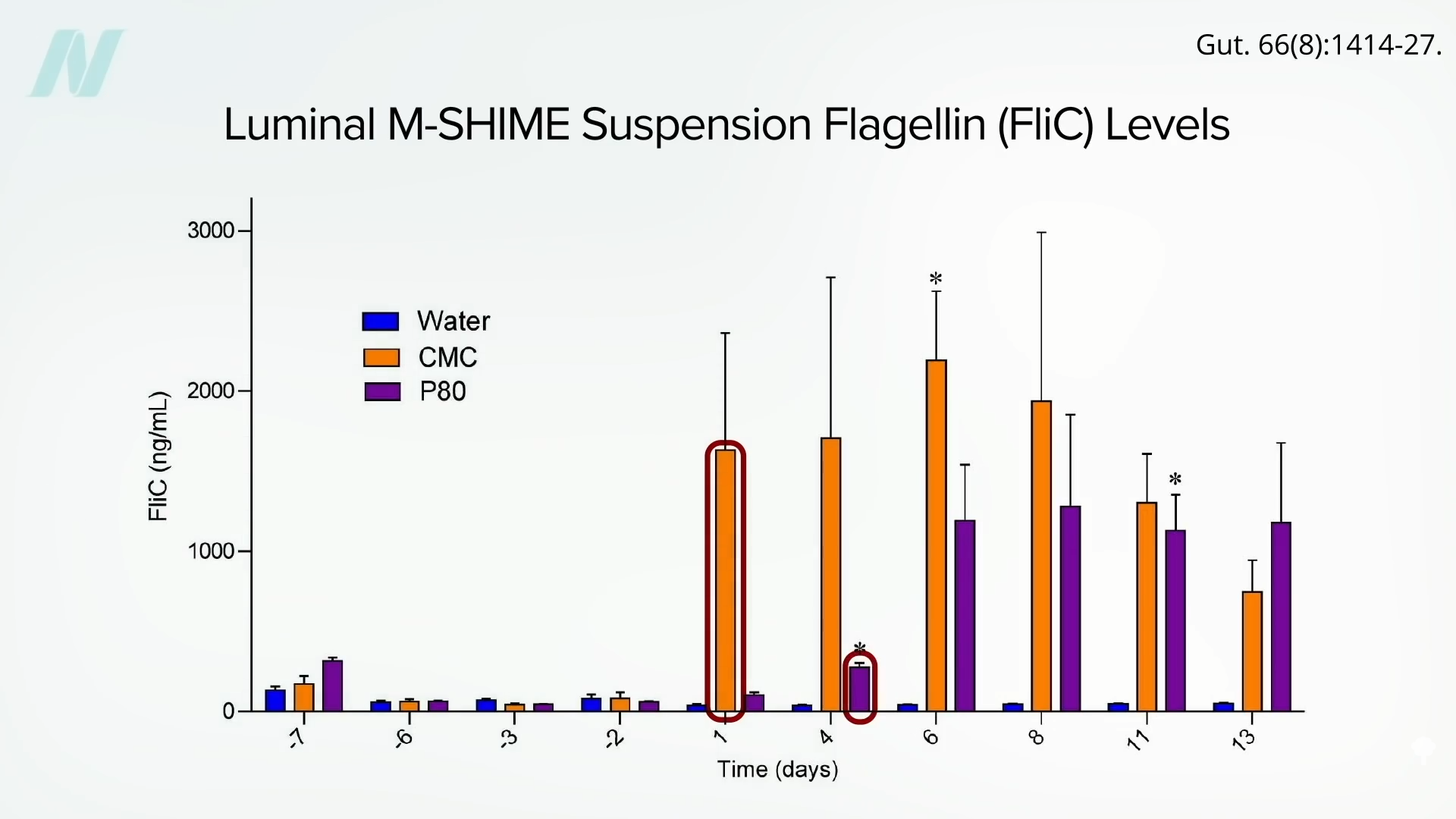
“This approach revealed that both P80 and CMC acted directly upon human microbiota to increase its proinflammatory potential…” When researchers then tested the effect of these emulsifiers on the protective mucus layer in petri dish cultures of human gut lining cells, they found that they can partially disrupt the protective layer. As you can see below and at 4:00 in my video, the green staining is the mucus. Both emulsifiers cut down the levels.
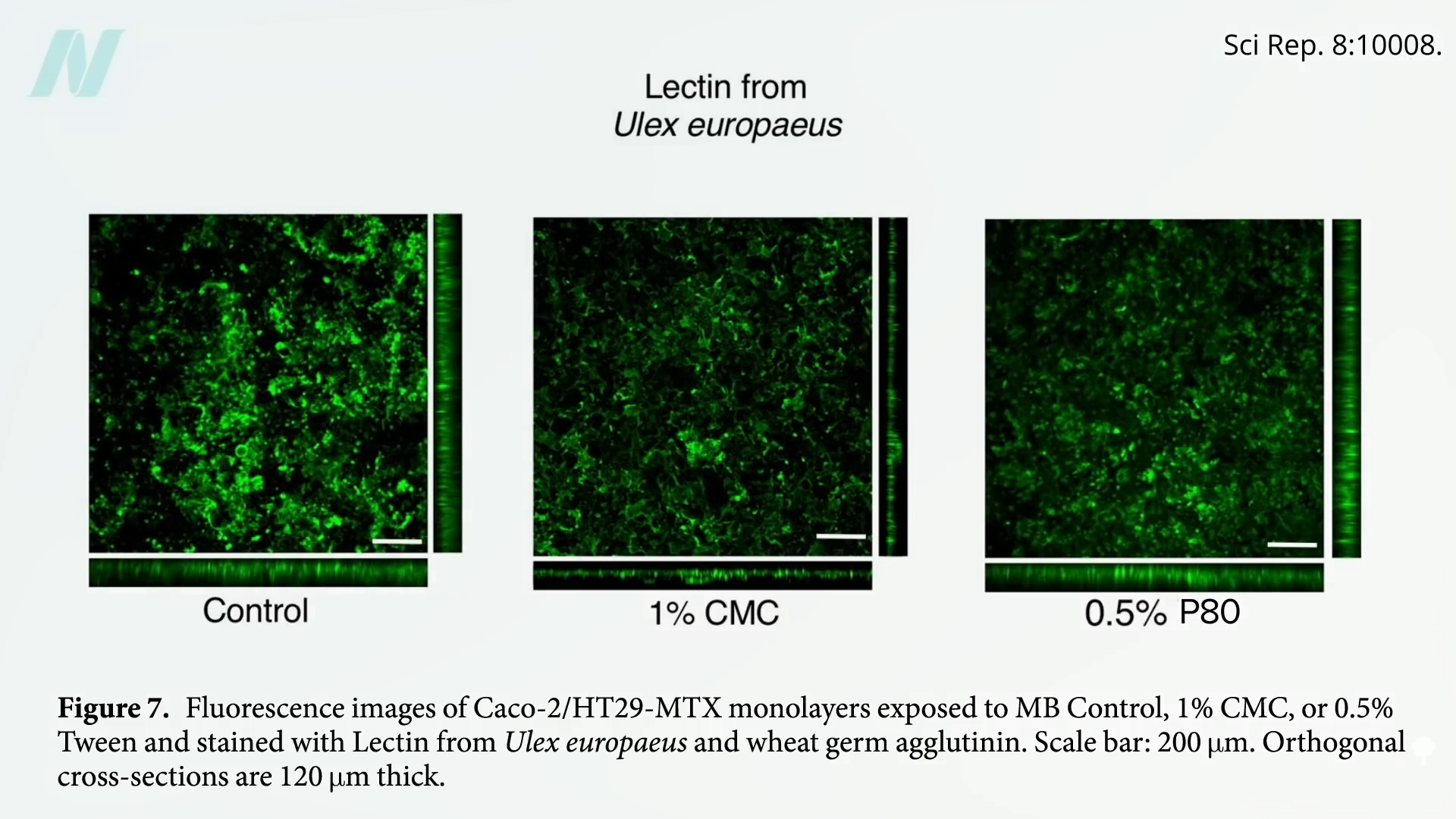
However, this study and the last both used emulsifier concentrations that were far in excess of what people might typically get day-to-day.
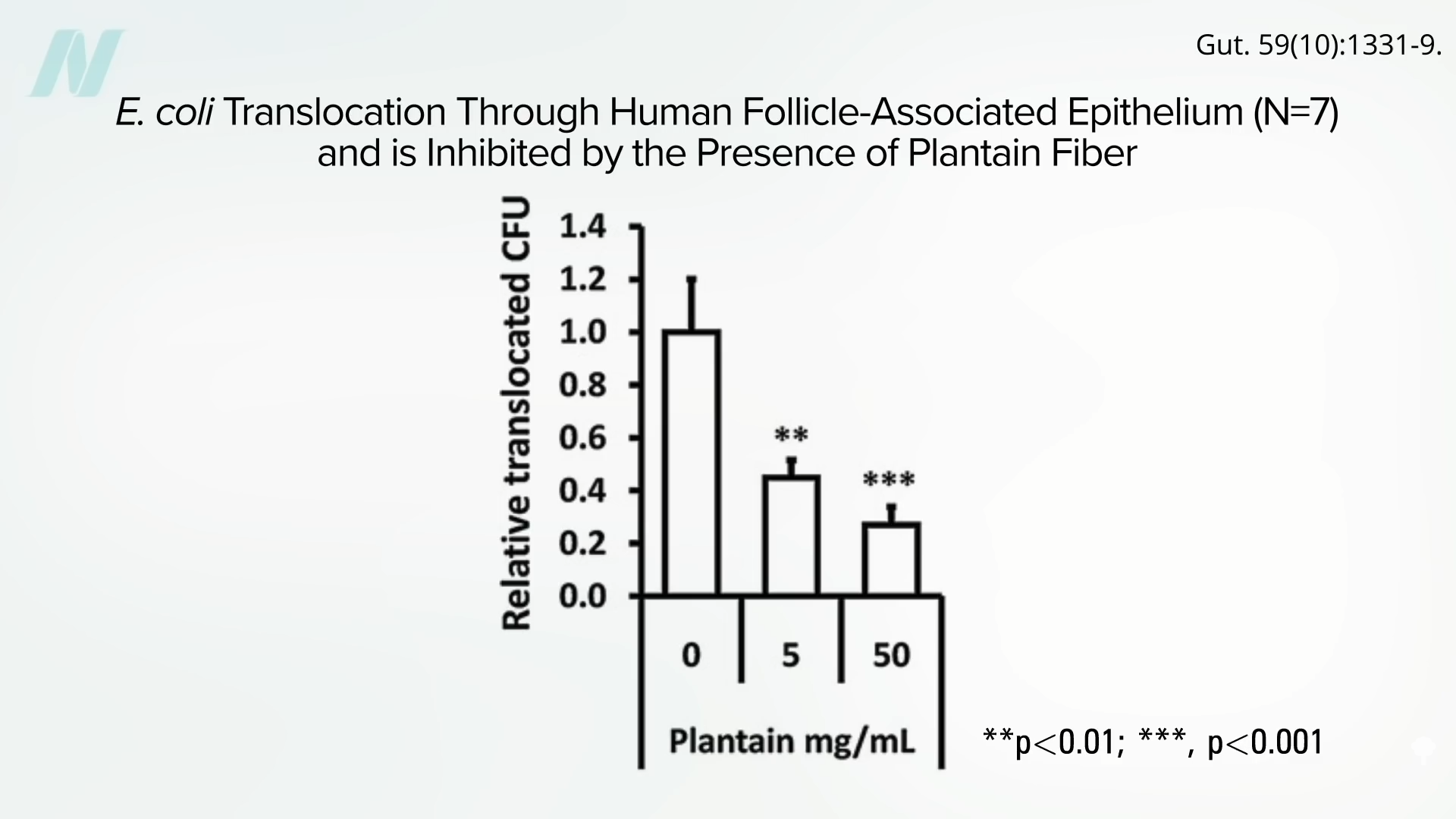
“Translocation of Crohn’s disease Escherichia coli across M-cells: contrasting effects of soluble plant fibres and emulsifiers” is probably the study that raised the greatest potential concern. The researchers surgically obtained cells, as well as actual intestinal wall tissue, and found that polysorbate 80 could double the invasion of E. coli through the intestinal lining tissue, as shown here and at 4:27 in my video.
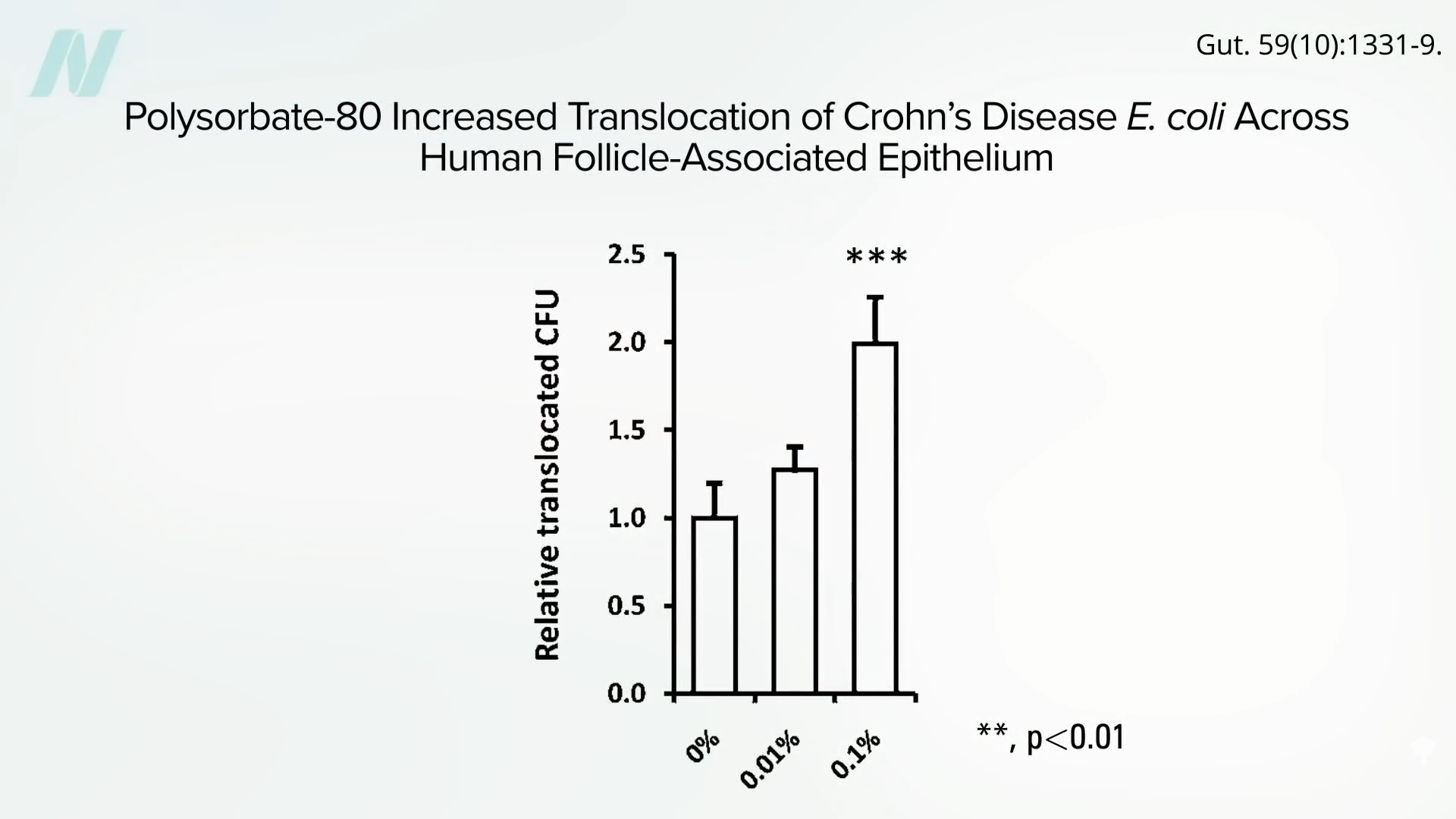 In contrast, adding fiber—in this case, fiber from plantains—could seal up the gut wall tissue twice as tightly, as seen below and at 4:33.
In contrast, adding fiber—in this case, fiber from plantains—could seal up the gut wall tissue twice as tightly, as seen below and at 4:33.
[ad_2]
Michael Greger M.D. FACLM
Source link
[ad_1]
Plant-based diets can be 98 percent effective in keeping ulcerative colitis patients in remission, far exceeding the efficacy of other treatments.
“One of the most common questions physicians treating patients with IBD [inflammatory bowel disease] are asked is whether changing diet could positively affect the course of their disease.” Traditionally, we had to respond that we didn’t know. That may now be changing, given the “evidence in the literature that hydrogen sulfide may play a role in UC,” ulcerative colitis. And, since the sulfur-containing amino acids concentrated in meat cause an increase in colonic levels of this rotten egg gas, perhaps we should “take off the meat.” Indeed, animal protein isn’t associated only with an increased risk of getting inflammatory bowel disease in the first place, but also IBD relapses once you have the disease.
This is a recent development. “Because the concept of IBD as a lifestyle disease mediated mainly by a westernized diet is not widely appreciated, an analysis of diet in the follow-up period [after diagnosis] in relation to a relapse of IBD has been ignored”—but no longer. Ulcerative colitis patients in remission and their diets were followed for a year to see which foods were linked to the return of their bloody diarrhea. Researchers found that the “strongest relationship between a dietary factor and an increased risk of relapse observed in this study was for a high intake of meat,” as I discuss in my video The Best Diet for Ulcerative Colitis Treatment.
What if people lower their intake of sulfur-containing amino acids by decreasing their consumption of animal products? Researchers tried this on four ulcerative colitis patients, and without any change in their medications, the patients experienced about a fourfold improvement in their loose stools. In fact, they felt so much better that the researchers didn’t think it was ethical to try switching the patients back to their typical diets. “Sulfur-containing amino acids are the primary source of dietary sulfur,” so a “low-sulfur” diet essentially means “a shift from a more traditional western diet (high in animal protein and fat, and low in fiber) to more of a plant-based diet (high in fiber, lower in animal protein and fat).” “Altogether, westernized diets are pro-inflammatory, and PBD [plant-based diets] are anti-inflammatory.”
What can treatment with a plant-based diet do after the onset of ulcerative colitis during a low-carbohydrate weight-loss diet? A 36-year-old man lost 13 pounds on a low-carb diet, but he also lost his health; he was diagnosed with ulcerative colitis. When he was put on a diet centered around whole plant foods, his symptoms resolved without medication. He achieved remission. That was just one case, though. Case reports are akin to glorified anecdotes. The value of case reports lies in their ability to inspire researchers to put them to the test, and that’s exactly what they did.
Until then, there had never been a study published that focused on using plant-based diets for treating ulcerative colitis. Wrote the researchers, a group of Japanese gastroenterologists, “We consider that the lack of a suitable diet is the biggest issue faced in the current treatment of IBD. We regard IBD as a lifestyle disease caused mainly by our omnivorous (Western) diet. We have been providing a plant-based diet (PBD) to all patients with IBD” for more than a decade and have published extraordinary results, far better than have been reported elsewhere in the medical literature to date. (I profiled some of their early work in one of the first videos that went up on NutritionFacts.org.) The researchers found a plant-based diet to be “effective in the maintenance of remission” in Crohn’s disease by 100 percent at one year and 90 percent at two years. What about a plant-based diet for relapse prevention in ulcerative colitis?
“Educational hospitalization” involved bringing patients into the hospital to control their diet and educate them about the benefits of plant-based eating (so they’d be more motivated to continue it at home). “Most patients (77%) experienced some improvement, such as disappearance or decrease of bloody stool during hospitalization.” Fantastic!
Here’s the really exciting part. The researchers then followed the patients for five years, and 81 percent of them remained in remission for the entire five years, and 98 percent kept the disease at bay for at least one year. That blows away other treatments. Those relapse rates are far lower than those reported with medication. Under conventional treatment, other studies found that about half of the individuals relapse, compared to only 2 percent of those taught to eat healthier.
“A PBD was previously shown to be effective in both the active and quiescent stages of Crohn’s disease. The current study showed that a PBD is effective in both the active and quiescent stages of UC as well.” So, the researchers did another study on even more severely affected cases with active disease and found the same results, with plant-based eating beating conventional drug therapy by far. People felt so much better that they were still eating more plant-based food even six years later. The researchers conclude that a plant-based diet is effective for treating ulcerative colitis to prevent a relapse.
Why? Well, plant-based diets are rich in fiber, which feeds our good gut bugs. “This observation might partly explain why a PBD prevents a variety of chronic diseases. Indeed, the same explanation applies to IBD, indicating that replacing an omnivorous diet with a PBD in IBD is the right approach.”
It’s like using plant-based diets to treat the cause of heart disease, our number one killer. Plant-based eating isn’t only safer and cheaper, but it also works better with no noted adverse side effects. Let’s compare that to the laundry list of side effects of immunosuppressants used for ulcerative colitis, like cyclosporine, which you can see below and at 5:40 in my video.
We now have even fancier drugs costing about $60,000 a year, about $5,000 a month, and they don’t even work very well; clinical remission at one year is only about 17 to 34 percent. And, instead of no adverse side effects, the drugs can give us a stroke, give us heart failure, and can even give us cancer, including a rare type of cancer that often results in death. Also, a serious brain disease known as progressive multifocal leukoencephalopathy, which can kill us, and for which there is no known treatment or cure. One drug lists an “increased risk of death” but touts that it’s just “a small pill” in an “easy-to-open bottle.” I’d skip the pills (and their potential side effects) and stick with plant-based eating.
Doctor’s Note:
If you missed the previous video, see Preventing Inflammatory Bowel Disease with Diet and stay tuned for The Best Diet for Crohn’s Disease Treatment, coming up next.
Check the related posts below for some older videos on IBD that may be of interest to you.
[ad_2]
Michael Greger M.D. FACLM
Source link