[ad_1]
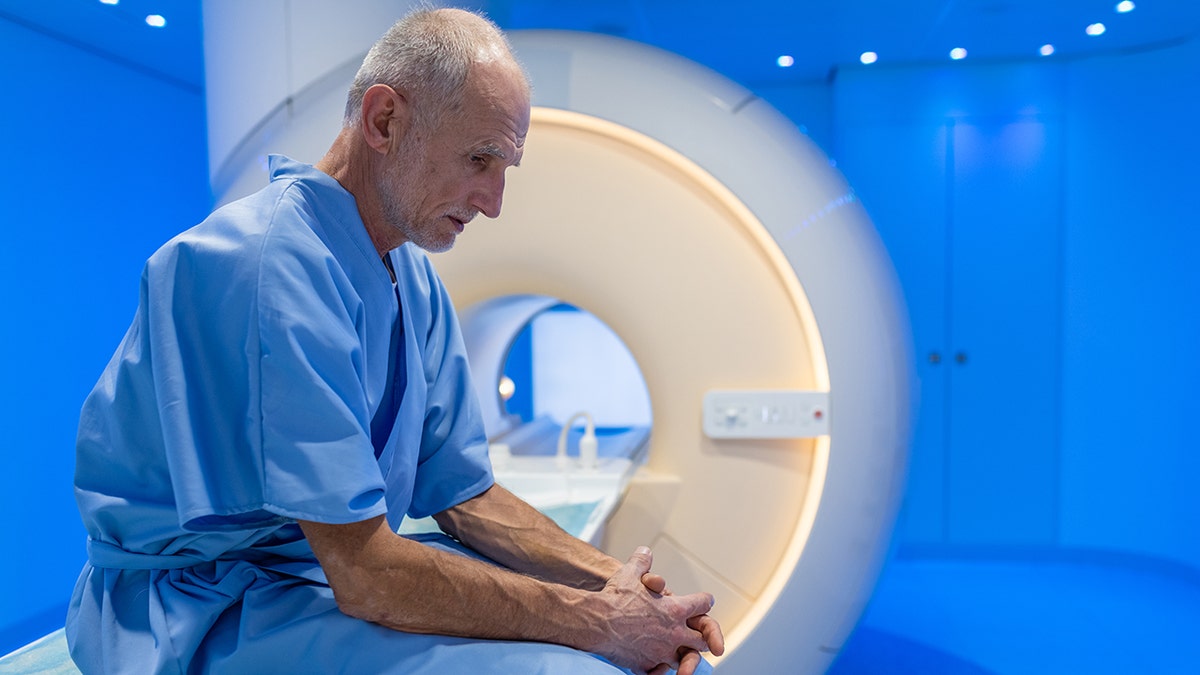
For more than a year, Diane Hunter, now 72, had been experiencing vague symptoms — pain in her spine and hips, nausea, exhaustion, thirst, and frequent urination. Her primary care physician had ruled out diabetes before finally chalking up her ailments to getting older.
But months of intense back pain eventually landed her in the emergency room, where a doctor suggested that Hunter might have multiple myeloma. Hunter’s first question was, “What is that?”
Multiple myeloma is a cancer that develops in bone marrow plasma cells, crowding out healthy blood cells and damaging the bones. It is one of the most common blood cancers — and the most diagnosed among African Americans. The mortality rate from multiple myeloma also is higher among African American patients than white people, with a number of studies showing that, in addition to disease biology, societal factors such as socioeconomic status and lack of access to health insurance or medical services delay timely diagnoses.
A belated diagnosis is what happened to Hunter, a Black woman in Montgomery, Alabama. She said her primary care doctor dismissed a recommendation from her endocrinologist to refer her to a hematologist after finding high protein counts in her blood. Then, she said, he also refused to order a bone marrow biopsy after the ER doctor suggested she might have multiple myeloma. Fed up, she said, she found a new doctor, got tested, and learned she indeed had the disease.
Monique Hartley-Brown, a multiple myeloma researcher at the Dana-Farber Cancer Institute in Boston, said Hunter’s experience is fairly common, particularly among Black patients who live in underserved communities.
“On average, patients see their primary doctor three times before being accurately diagnosed,” Hartley-Brown said. “The delay from symptom onset to diagnosis is even longer for Black Americans. Meanwhile, the disease is wreaking havoc — causing fractures, severe anemia, fatigue, weight loss, kidney problems.”
Black and Hispanic patients are also less likely to receive the newest therapies, according to the Multiple Myeloma Research Foundation, and, when they do, they are more likely to do so later in the course of their disease than white patients. An analysis published in 2022 of racial and ethnic disparities in multiple myeloma drug approval trials submitted to the Food and Drug Administration concluded that Black patients made up only 4% of participants despite being roughly 20% of those living with the disease.
Now, even though significant progress has been made in understanding the biology of multiple myeloma and how to treat it, those racial gaps may grow larger amid federal cuts to cancer research and the backlash against diversity and inclusion efforts. While few multiple myeloma experts were willing to talk on the record about the impact of the funding cutbacks, Michael Andreini, president and CEO of the Multiple Myeloma Research Foundation, has written that cuts to the National Institutes of Health and its National Cancer Institute put future innovations at risk.
“Even before these potential cuts, funding for myeloma lagged behind,” he wrote before the cuts were finalized. “The myeloma specific budget has decreased significantly. Myeloma is almost 2% of all cancers, yet receives less than 1% of the NCI’s budget.”
The disease is already hard to diagnose. Because multiple myeloma is usually diagnosed when a patient is over 65 (African Americans tend to be diagnosed five years younger, on average), common symptoms such as lower back pain and fatigue are often chalked up to just getting older.
That’s what happened to Jim Washington of Charlotte, North Carolina. He was 61 when excruciating hip pain brought his regular tennis games to a sudden stop.
“I figured I’d done something to injure myself,” Washington said. “But I’d been playing tennis all my life, and this pain was different from anything I’d ever felt before.”
Washington was fortunate to have a concierge doctor and premium health insurance. In quick succession, he underwent X-rays that revealed a lesion on his spine and received a referral to an oncologist, who identified a cancerous tumor. A subsequent biopsy and blood tests confirmed he had multiple myeloma.
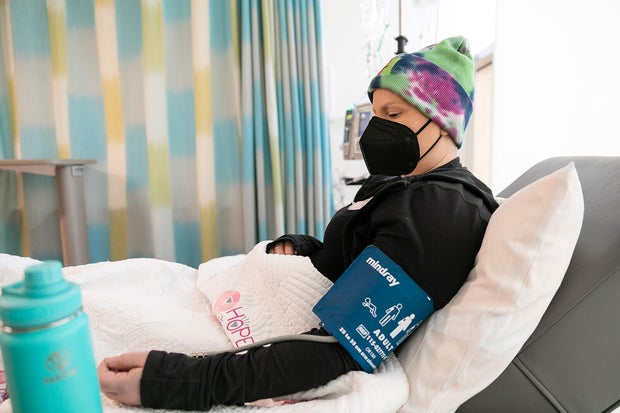
A.M. Stewart for KFF Health News
Washington had weeks of high-dose chemotherapy, followed by what is known as an autologous stem cell transplant, which used his own stem cells to regrow healthy blood cells in his body. It was a grueling process that ultimately left him with a clean bill of health. For the next several years, his doctors monitored him closely, including conducting an annual bone marrow biopsy.
Before treatment, he said, myeloma had infiltrated 60% of his blood cells. The stem cell transplant brought those levels down to zero. After about five years, however, his multiple myeloma level had crept back up to 10% and required more treatment.
But Washington had closely followed the latest research and believed he had reason to be optimistic. The FDA had approved the first CAR T-cell therapy for multiple myeloma in 2021.
Hartley-Brown said the lack of Black patients in multiple myeloma drug approval trials raises concerns about whether the trial results are equally applicable to the Black population and may help explain why treatment advances have been less effective in Black patients.
She cited multiple causes for the low trial participation rate, including historical distrust of the medical establishment and a lack of available clinical trials. “If you are living in an underserved or underrepresented area, the hospital or community doctor may not have clinical trials available, or that patient may have limitations getting to that location affiliated with the clinical trial,” she said.
Washington, a Black patient, appears to have avoided this trap, having benefited from the latest treatments both times. In January, he began six weeks of chemotherapy with a three-drug combination of Velcade, Darzalex, and dexamethasone before undergoing CAR T-cell therapy.
For that, doctors collected Washington’s T cells, a type of white blood cell, and genetically modified them to better recognize and destroy the cancer cells before reinfusing them into his body. He didn’t require hospitalization post-transplant and could do daily blood draws at home. His energy levels were much higher than during his first treatment.
“I’ve been in a very privileged position,” Washington said. “The prognosis is very positive, and I’m feeling good about where I am at this point.”
Hunter, too, considers herself lucky despite receiving a delayed diagnosis. After her diagnosis in January 2017, she underwent five months of immunotherapy with a three-drug combination (Revlimid, Velcade, and dexamethasone) followed by a successful stem cell transplant and two weeks in the hospital. She has been in remission since July 2017.
Hunter, now a support group co-leader and patient advocate, said that stories like Washington’s and her own provide hope despite the research cuts.
In the eight years since her treatment, she said, she’s seen the thinking around multiple myeloma — long described as a treatable but incurable disease — begin to shift as a growing subset of patients remain disease-free for many years. She said she has even met people living with the disease for 30 years.
“The word ‘cure’ is now being heard,” Hunter said.
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF — the independent source for health policy research, polling, and journalism.
[ad_2]