[ad_1]
What happened when topical olive oil was pitted against an ibuprofen-type drug for osteoarthritis and rheumatoid arthritis?
Fifty million Americans suffer from arthritis, and osteoarthritis of the knee is the most common form, making it a leading cause of disability. There are several inflammatory pathways that underlie the disease’s onset and progression, so various anti-inflammatory foods have been put to the test. Strawberries can decrease circulating blood levels of an inflammatory mediator known as tumor necrosis factor, but that doesn’t necessarily translate into clinical improvement. For example, drinking cherry juice may lower a marker of inflammation known as C-reactive protein, but it failed to help treat pain and other symptoms of knee osteoarthritis. However, researchers claimed it “provided symptom relief.” Yes, it did when comparing symptoms before and after six weeks of drinking cherry juice, but not any better than a placebo, meaning drinking it was essentially no better than doing nothing. Cherries may help with another kind of arthritis called gout, but they failed when it came to osteoarthritis.
However, strawberries did decrease inflammation. In fact, in a randomized, double-blind, crossover trial, dietary strawberries were indeed found to have a significant analgesic effect, causing a significant decrease in pain. There are tumor necrosis factor inhibitor drugs on the market now available for the low, low cost of only about $40,000 a year. For that kind of money, you’d want some really juicy side effects, and they do not disappoint—like an especially fatal lymphoma. I think I’ll stick with the strawberries.
One reason we suspected berries might be helpful is that when people consumed the equivalent of a cup of blueberries or two cups of strawberries daily, and their blood was then applied to cells in a petri dish, it significantly reduced inflammation compared to blood from those who consumed placebo berries, as you can see below and at 2:02 in my video Extra Virgin Olive Oil for Arthritis.
Interestingly, the anti-inflammatory effect increased over time, suggesting that the longer you eat berries, the better. Are there any other foods that have been tested in this way?
Researchers in France collected cartilage from knee replacement surgeries and then exposed it to blood samples from volunteers who had taken a whopping dose of a grapeseed and olive extract. They saw a significant drop in inflammation, as shown below and at 2:30 in my video.
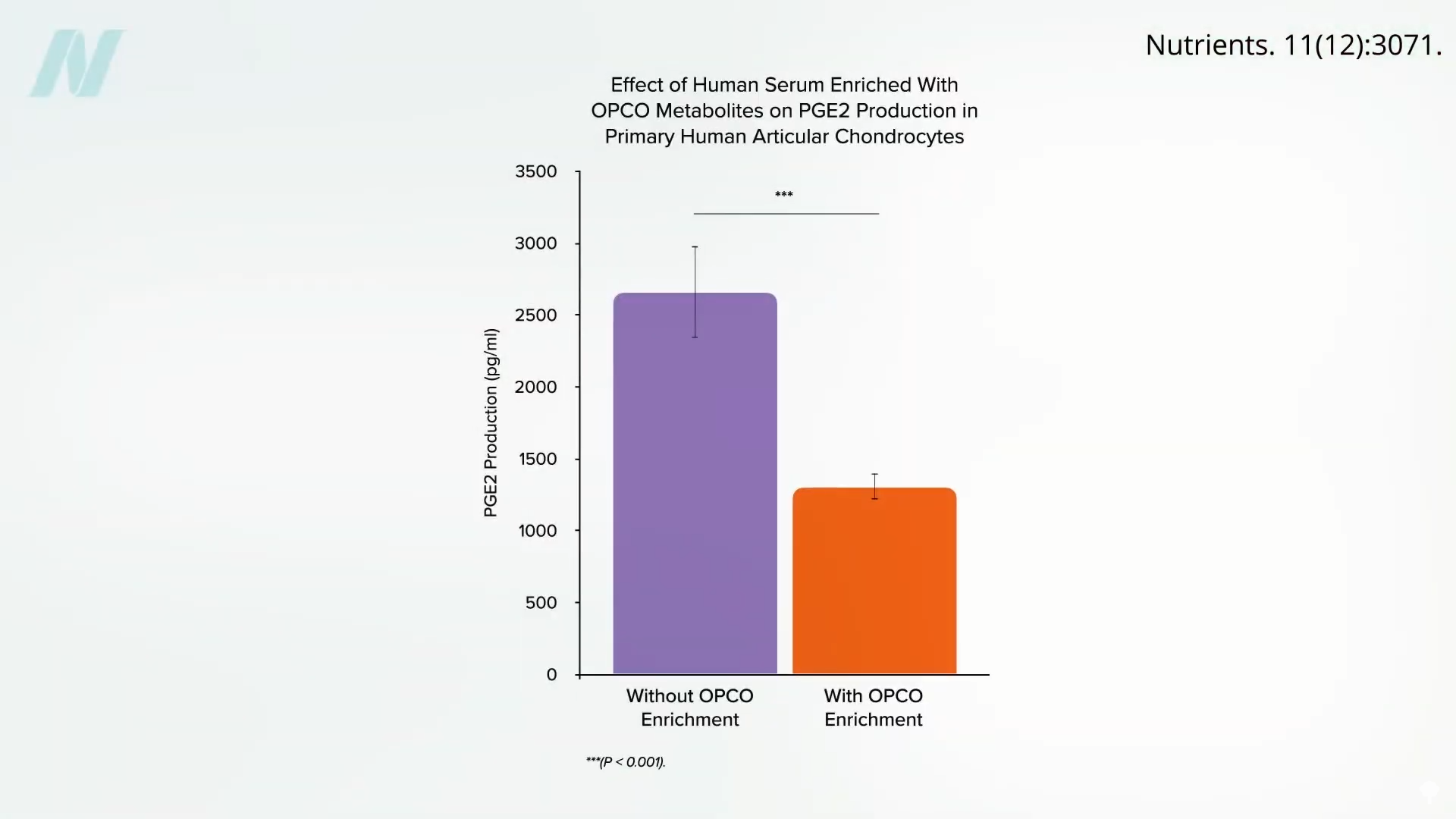
There haven’t been any human studies putting grapeseeds to the test for arthritis, but an olive extract was shown to decrease pain and improve daily activities in osteoarthritis sufferers. So, does this mean adding olive oil to one’s diet may help? No, because the researchers used freeze-dried olive vegetation water. That’s basically what’s left over after you extract the oil from olives; it’s all the water-soluble components. In other words, it’s all the stuff that’s in an olive that‘s missing from olive oil.
If you give people actual olives, a dozen large green olives a day, you may see a drop in an inflammatory mediator. But according to a systematic review and meta-analysis, olive oil—on its own—does not appear to offer any anti-inflammatory benefits. What about papers that ascribe “remarkable anti-inflammatory activity” to extra virgin olive oil? Their evidence is from rodents. In people, extra virgin olive oil may be no better than butter when it comes to inflammation and worse than even coconut oil.
So, should we just stick to olives? Sadly, a dozen olives could take up nearly half your sodium limit for the entire day, as you can see below and at 3:47 in my video.

When put to the test, extra virgin olive oil did not appear to help with fibromyalgia symptoms either, but it did work better than canola oil in alleviating symptoms of inflammatory bowel disease. Unfortunately, I couldn’t find any studies putting olive oil intake to the test for arthritis. But why then is this blog entitled “Can Olive Oil Compete with Arthritis Drugs?” Because—are you ready for this?—it appears to work topically.
Topical virgin olive oil went up against a gel containing an ibuprofen-type drug for osteoarthritis of the knee in a double-blind, randomized, clinical trial. Just a gram of oil, which is less than a quarter teaspoon, three times a day, costing less than three cents a day, worked! Topical olive oil was significantly better than the drug in reducing pain, as you can see below and at 4:37 in my video.
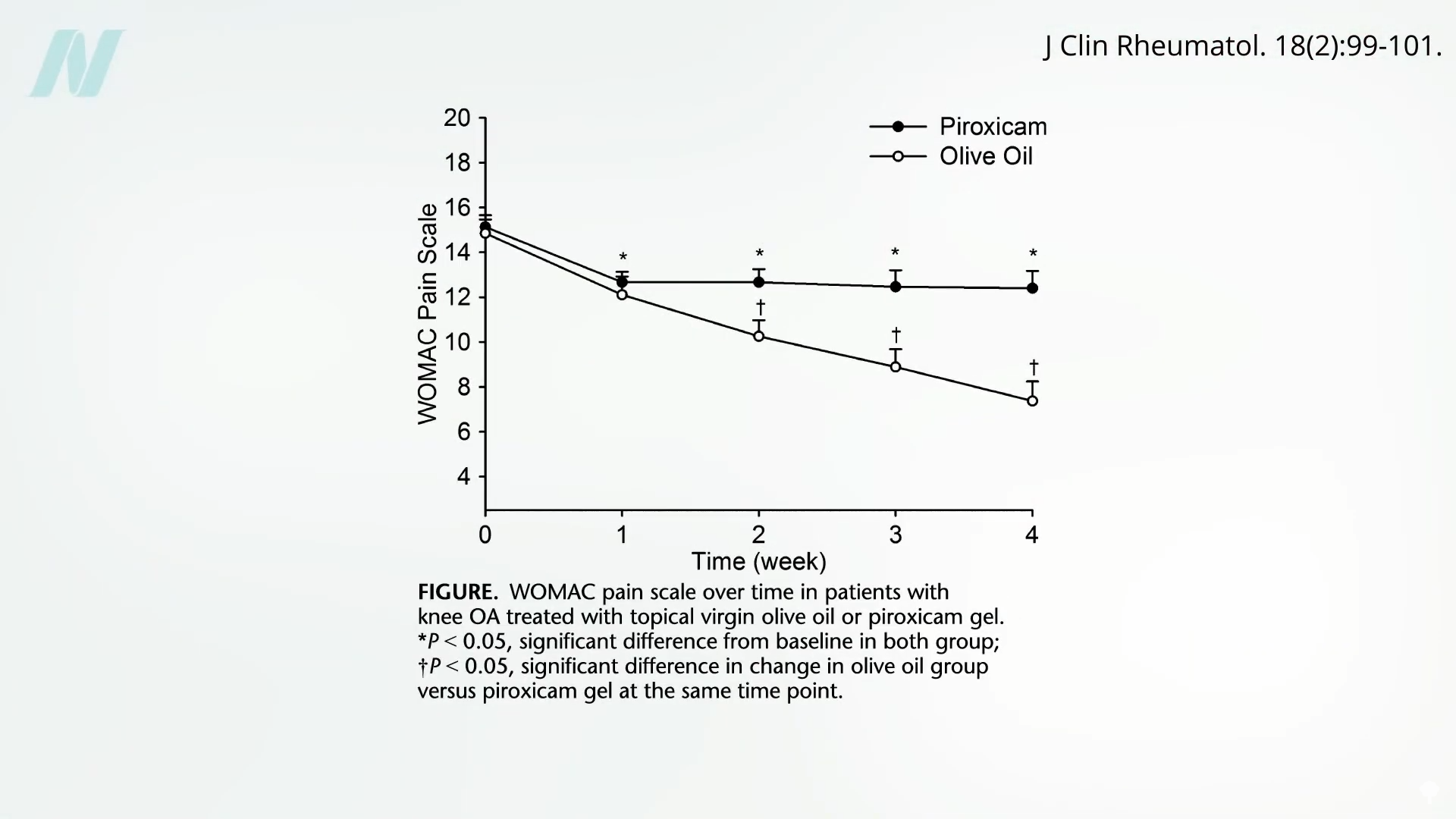
The study only lasted a month, so is it possible that the olive oil would have continued to work better and better over time?
Is olive oil effective in controlling morning inflammatory pain in the fingers and knees among women with rheumatoid arthritis? The researchers went all out, comparing the use of extra virgin olive oil to rubbing on nothing and also to rubbing on that ibuprofen-type gel, and, evidently, the decrease in the disease activity score in the olive oil group beat out the others.
Doctor’s Note
For more on joint health, see related posts below.
What about eating olive oil? See Olive Oil and Artery Function.
[ad_2]
Michael Greger M.D. FACLM
Source link