ATLANTA — ATLANTA (AP) — Former first lady Rosalynn Carter, the closest adviser to Jimmy Carter during his one term as U.S. president and their four decades thereafter as global humanitarians, has died at the age of 96.
The Carter Center said she died Sunday after living with dementia and suffering many months of declining health. The statement announcing her death said she “died peacefully, with family by her side” at 2:10 p.m. at her rural Georgia home of Plains.
“Rosalynn was my equal partner in everything I ever accomplished,” Carter said in the statement. “She gave me wise guidance and encouragement when I needed it. As long as Rosalynn was in the world, I always knew somebody loved and supported me.”
President Joe Biden called the Carters “an incredible family because they brought so much grace to the office.”
“He had this great integrity, still does. And she did too,” Biden told reporters as he was boarding Air Force One to leave Norfolk, Virginia, on Sunday night. “God bless them.” Biden said he spoke to the family and was told that Jimmy Carter was surrounded by his children and grandchildren.
Later, the White House released a joint statement from the president and first lady Jill Biden saying that Carter inspired the nation. “She was a champion for equal rights and opportunities for women and girls; an advocate for mental health and wellness for every person; and a supporter of the often unseen and uncompensated caregivers of our children, aging loved ones, and people with disabilities,” the statement said.
Reaction from world leaders poured in throughout the day.
The Carters were married for more than 77 years, forging what they both described as a “full partnership.” Unlike many previous first ladies, Rosalynn sat in on Cabinet meetings, spoke out on controversial issues and represented her husband on foreign trips. Aides to President Carter sometimes referred to her — privately — as “co-president.”
“Rosalynn is my best friend … the perfect extension of me, probably the most influential person in my life,” Jimmy Carter told aides during their White House years, which spanned from 1977-1981.
The former president, now 99, remains at the couple’s home in Plains after entering hospice care himself in February.
Fiercely loyal and compassionate as well as politically astute, Rosalynn Carter prided herself on being an activist first lady, and no one doubted her behind-the-scenes influence. When her role in a highly publicized Cabinet shakeup became known, she was forced to declare publicly, “I am not running the government.”
Many presidential aides insisted that her political instincts were better than her husband’s — they often enlisted her support for a project before they discussed it with the president. Her iron will, contrasted with her outwardly shy demeanor and a soft Southern accent, inspired Washington reporters to call her “the Steel Magnolia.”
Both Carters said in their later years that Rosalynn had always been the more political of the two. After Jimmy Carter’s landslide defeat in 1980, it was she, not the former president, who contemplated an implausible comeback, and years later she confessed to missing their life in Washington.
Jimmy Carter trusted her so much that in 1977, only months into his term, he sent her on a mission to Latin America to tell dictators he meant what he said about denying military aid and other support to violators of human rights.
She also had strong feelings about the style of the Carter White House. The Carters did not serve hard liquor at public functions, though Rosalynn did permit U.S. wine. There were fewer evenings of ballroom dancing and more square dancing and picnics.
Throughout her husband’s political career, she chose mental health and problems of the elderly as her signature policy emphasis. When the news media didn’t cover those efforts as much as she believed was warranted, she criticized reporters for writing only about “sexy subjects.”
As honorary chairwoman of the President’s Commission on Mental Health, she once testified before a Senate subcommittee, becoming the first first lady since Eleanor Roosevelt to address a congressional panel. She was back in Washington in 2007 to push Congress for improved mental health coverage, saying, “We’ve been working on this for so long, it finally seems to be in reach.”
She said she developed her interest in mental health during her husband’s campaigns for Georgia governor.
“I used to come home and say to Jimmy, ‘Why are people telling me their problems?’ And he said, ‘Because you may be the only person they’ll ever see who may be close to someone who can help them,’” she explained.
After Ronald Reagan won the 1980 election, Rosalynn Carter seemed more visibly devastated than her husband. She initially had little interest in returning to the small town of Plains, Georgia, where they both were born, married and spent most of their lives.
“I was hesitant, not at all sure that I could be happy here after the dazzle of the White House and the years of stimulating political battles,” she wrote in her 1984 autobiography, “First Lady from Plains.” But “we slowly rediscovered the satisfaction of a life we had left long before.”
After leaving Washington, Jimmy and Rosalynn co-founded The Carter Center in Atlanta to continue their work. She chaired the center’s annual symposium on mental health issues and raised funds for efforts to aid the mentally ill and homeless. She also wrote “Helping Yourself Help Others,” about the challenges of caring for elderly or ailing relatives, and a sequel, “Helping Someone With Mental Illness.”
Frequently, the Carters left home on humanitarian missions, building houses with Habitat for Humanity and promoting public health and democracy across the developing world.
“I get tired,” she said of her travels. “But something so wonderful always happens. To go to a village where they have Guinea worm and go back a year or two later and there’s no Guinea worm, I mean the people dance and sing — it’s so wonderful.”
In 2015, Jimmy Carter’s doctors discovered four small tumors on his brain. The Carters feared he had weeks to live. He was treated with a drug to boost his immune system, and later announced that doctors found no remaining signs of cancer. But when they first received the news, she said she didn’t know what she was going to do.
“I depend on him when I have questions, when I’m writing speeches, anything, I consult with him,” she said.
She helped Carter recover several years later when he had hip replacement surgery at age 94 and had to learn to walk again. And she was with him earlier this year when he decided after a series of hospital stays that he would forgo further medical interventions and begin end-of-life care.
Jimmy Carter is the longest-lived U.S. president. Rosalynn Carter was the second longest-lived of the nation’s first ladies, trailing only Bess Truman, who died at age 97.
Eleanor Rosalynn Smith was born in Plains on Aug. 18, 1927, the eldest of four children. Her father died when she was young, so she took on much of the responsibility of caring for her siblings when her mother went to work part time.
She also contributed to the family income by working after school in a beauty parlor. “We were very poor and worked hard,” she once said, but she kept up her studies, graduating from high school as class valedictorian.
She soon fell in love with the brother of one of her best friends. Jimmy and Rosalynn had known each other all their lives — it was Jimmy’s mother, nurse Lillian Carter, who delivered baby Rosalynn — but he left for the Naval Academy in Annapolis, Maryland, when she was still in high school.
After a blind date, Jimmy told his mother: “That’s the girl I want to marry.” They wed in 1946, shortly after his graduation from Annapolis and Rosalynn’s graduation from Georgia Southwestern College.
Their sons were born where Jimmy Carter was stationed: John William (Jack) in Portsmouth, Virginia, in 1947; James Earl III (Chip) in Honolulu in 1950; and Donnel Jeffery (Jeff) in New London, Connecticut, in 1952. Amy was born in Plains in 1967. By then, Carter was a state senator.
Navy life had provided Rosalynn her first chance to see the world. When Carter’s father, James Earl Sr., died in 1953, Jimmy Carter decided, without consulting his wife, to move the family back to Plains, where he took over the family farm. She joined him there in the day-to-day operations, keeping the books and weighing fertilizer trucks.
“We developed a partnership when we were working in the farm supply business,” Rosalynn Carter recalled with pride in a 2021 interview with The Associated Press. “I knew more on paper about the business than he did. He would take my advice about things.”
At the height of the Carters’ political power, Lillian Carter said of her daughter-in-law: “She can do anything in the world with Jimmy, and she’s the only one. He listens to her.”
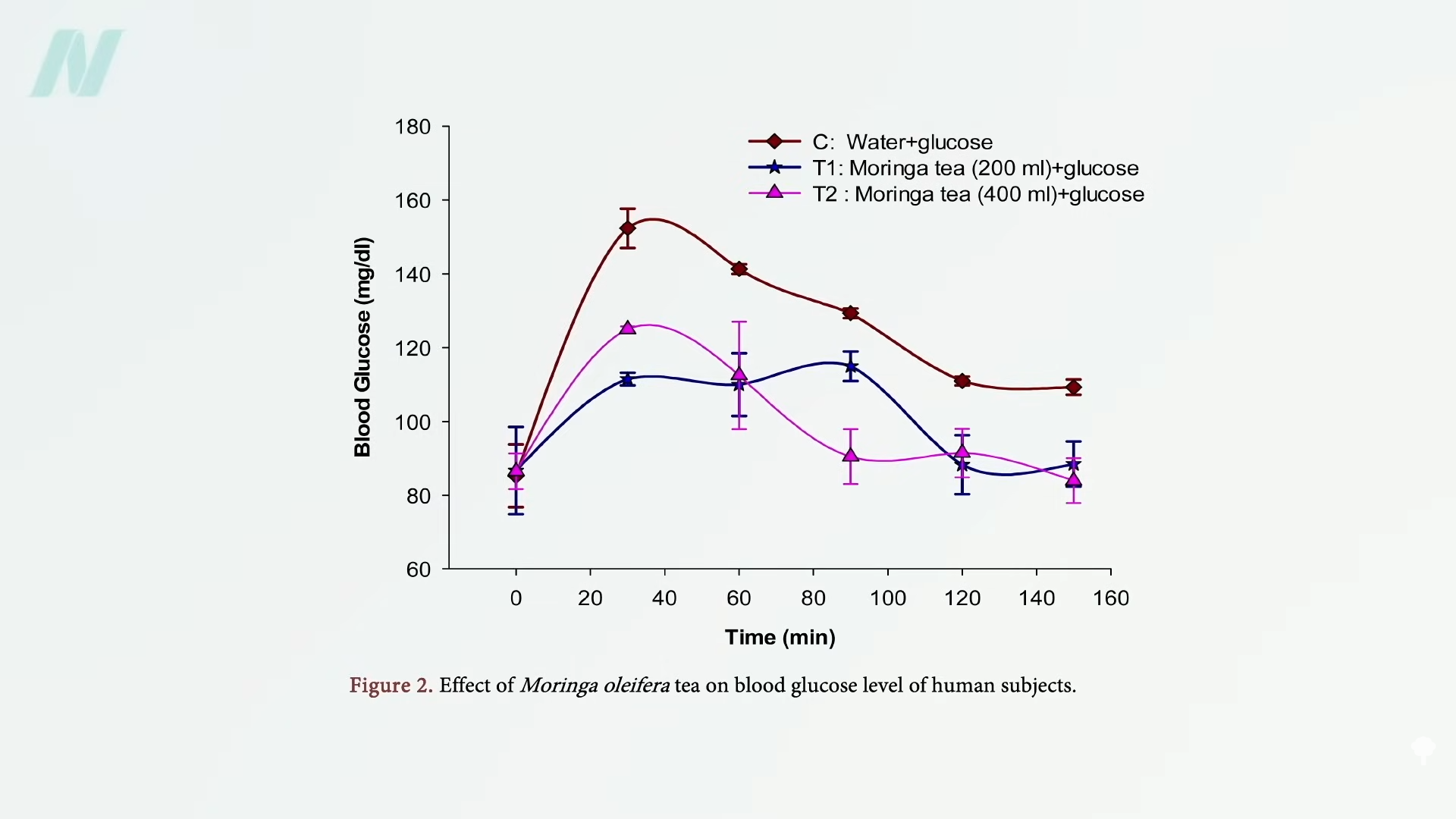 People with diabetes were
People with diabetes were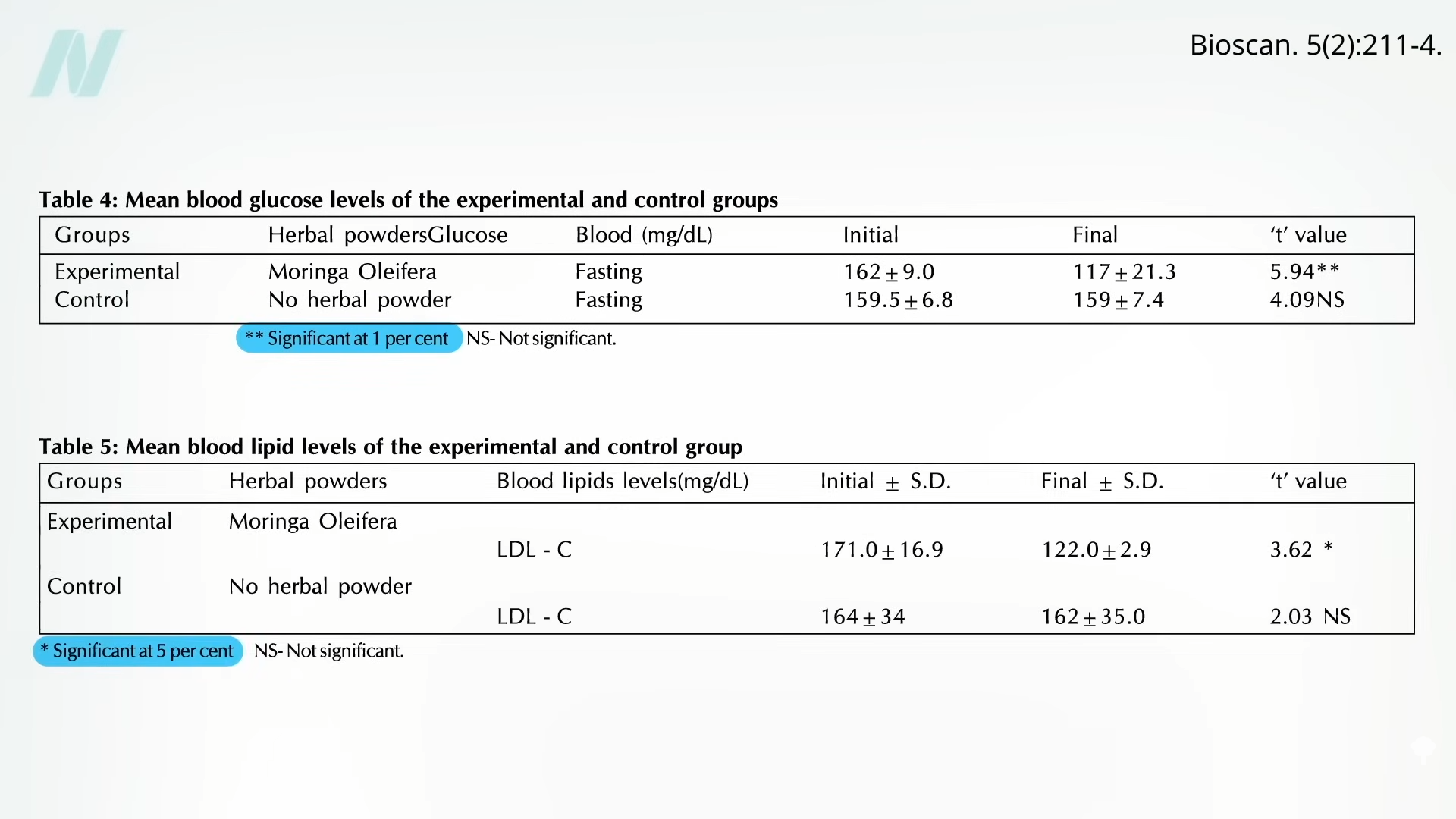


 Medically-supervised fasting has
Medically-supervised fasting has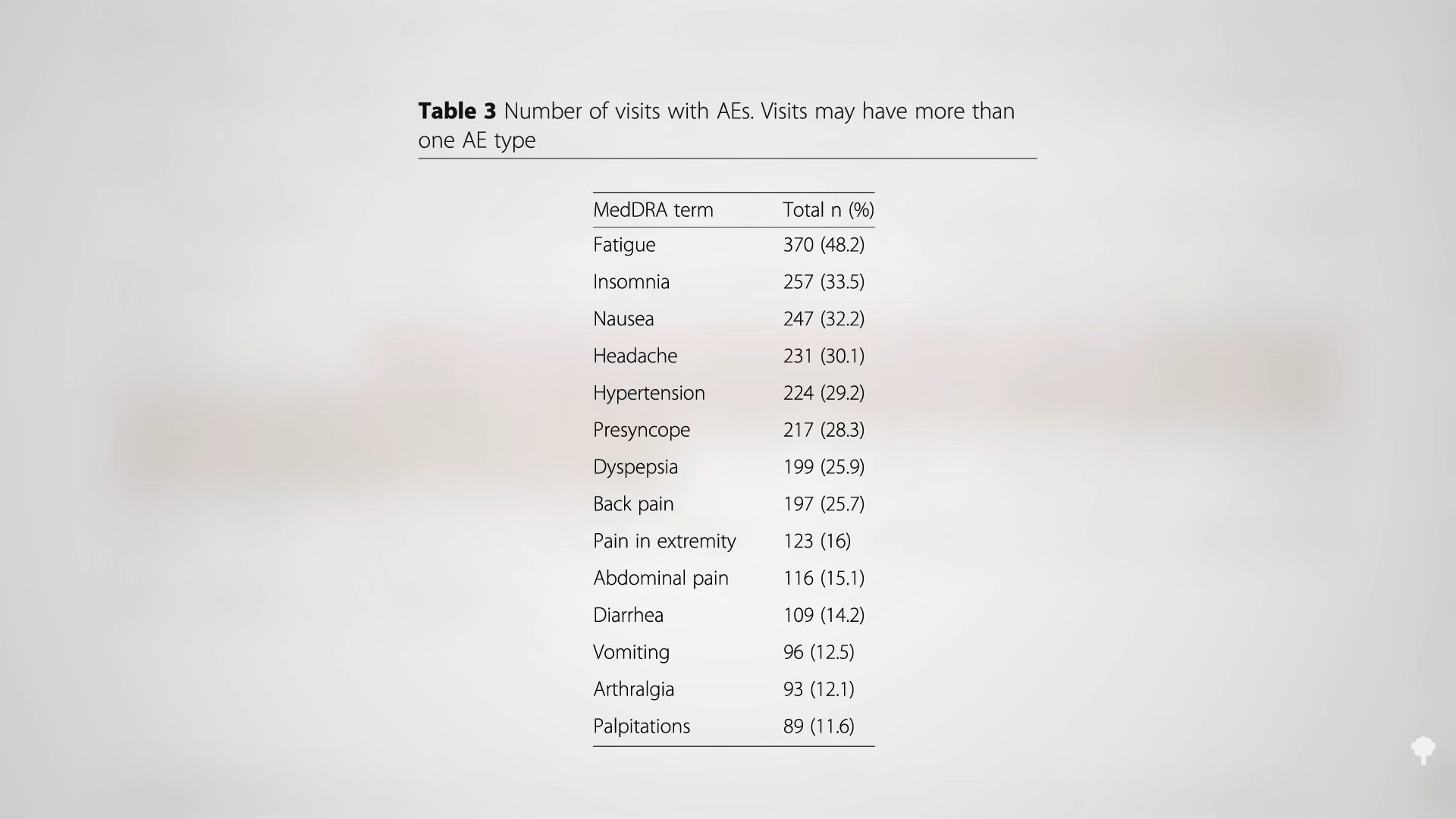 “
“