While her wife was pregnant with their son, Aimee MacDonald took an unusual step of preparing her own body for the baby’s arrival. First she began taking hormones, and then for six weeks straight, she pumped her breasts day and night every two to three hours. This process tricked her body into a pregnant and then postpartum state so she could make breast milk. By the time the couple’s son arrived, she was pumping 27 ounces a day—enough to feed a baby—all without actually getting pregnant or giving birth.
And so, after a 38-hour labor and emergency C-section, MacDonald’s wife could do what many mothers who just gave birth might desperately want to but cannot: rest, sleep, and recover from surgery. Meanwhile, MacDonald tried nursing their baby. She held him to her breast, and he latched right away. Over the next 15 months, the two mothers co-nursed their son, switching back and forth, trading feedings in the middle of the night. MacDonald had breastfed her older daughter the usual way—as in, by herself—a decade earlier, and she remembered the bone-deep exhaustion. She did not want that for her wife. Inducing lactation meant they could share in the ups and the downs of breastfeeding together.
MacDonald, who lives in a small town in Nova Scotia, had never met anyone who had tried this before. People she told were routinely shocked to learn that induced lactation—making milk without pregnancy—is biologically possible. They had so many questions: Was it safe? Did she have side effects? How did it even work? But when she described how she and her wife shared nursing duties, many women told her, “I wish I had had that.”
Induced lactation wasn’t initially developed for co-nursing. Mothers who wanted to breastfeed their adoptive babies were the first to experiment with hormones and pumping. But over time, the few experts who specialize in induced lactation told me, that has given way to more queer couples who want to share or swap nursing duties. Early in her career, Alyssa Schnell, a lactation consultant in St. Louis who herself breastfed her adopted daughter 17 years ago, found that when she suggested to same-sex couples that the non-birthing partner might try nursing, “they would be horrified.” The idea that a woman would nurse a baby she did not give birth to—common in the era of wet nurses—had become strange in our era of off-the-shelf formula. Now parents are coming to her asking to induce lactation, and more of them are interested in co-nursing.
About a quarter of all babies in the U.S. are breastfed exclusively for six months; more than half are breastfed at least some of the time. The statistics don’t say by whom, but that’s because they don’t need to. We can assume it’s virtually always their birthing mother. Even with the help of formula, the pressure around or preference for breastfeeding means that, in many families, the work of feeding falls disproportionately on one parent. But induced lactation decouples breastfeeding from birth. By manipulating biology, parents who co-nurse are testing the limits of just how equal a relationship can truly be.
Breastfeeding is hard work, even when it’s “natural.” Adding induced lactation is harder work still. MacDonald was putting herself on a newborn schedule weeks before her baby was even born. She pumped at home. She pumped at work. She even pumped while her wife was in labor, because skipping sessions can cause milk supply to drop. As Diane Spatz, a lactation expert at the University of Pennsylvania and Children’s Hospital of Philadelphia, puts it, “You have to start pumping like a wild person.”
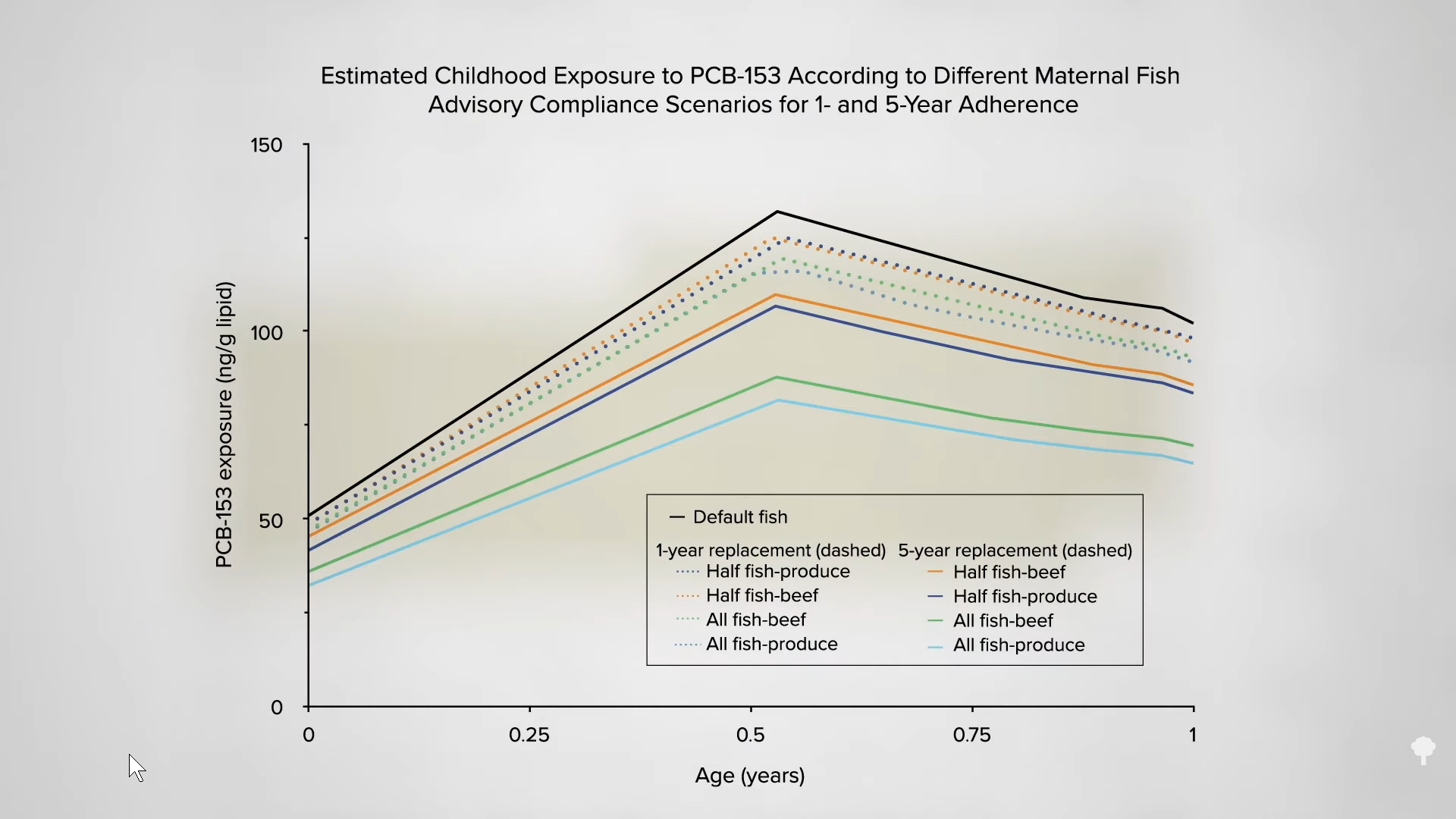
MacDonald followed a version of the Newman-Goldfarb protocol, named after a pediatrician and an adoptive mother who documented and shared the process in 2000. In addition to pumping, the protocol includes birth control, which causes a surge of progesterone and estrogen akin to pregnancy hormones, and a drug called domperidone, which boosts the milk hormone prolactin. Together they biochemically prime the body for milk production. It’s unusual, Schnell told me, for a woman inducing lactation to make enough milk to feed a baby all on her own—unless she’s breastfed before, like MacDonald had—but it’s also unusual to make no milk at all.
Read: The problems with breastfeeding go way beyond pumps
In the U.S., getting domperidone can be a challenge. Though the drug is widely available in Canada, Australia, and Europe, the FDA has banned it in the United States, citing the risk of abnormal heart rhythms and even death. But these heart problems have shown up only in the elderly, foreign experts have noted, and Australian scientists concluded in a 2019 review that domperidone is safe for lactation, as long as women are screened for heart conditions. But in the U.S., parents usually aren’t taking it under the supervision of a doctor. They might buy pills with a prescription at a Canadian pharmacy or surreptitiously order the drug online through overseas pharmacies. “There was a brief moment when you could only buy it in Bitcoin,” says Lauren Vallone, whose partner, Robin Berryman, induced lactation so that they could co-nurse their daughter, who was born in 2020.
Inducing lactation felt like a DIY project to Vallone and Berryman. As a queer couple trying to start a family, though, they were also used to doing things a different way. They eventually reached out to Schnell for guidance, but they also swapped tips in a Facebook support group that had a wealth of anecdotal advice. Not that most doctors would have been helpful. Even the idea that one can breastfeed without having been pregnant isn’t widely known, Spatz told me. “Nurses are surprised about that,” she said. “Physicians don’t know that.”
Vallone and Berryman planned to divide nursing duties 50/50, but they didn’t know exactly what that would look like. Would they trade off every other feeding? Would one nurse while the other pumped? What about when one parent went back to work? “There’s stories of people who have induced lactation, but then there’s no, like, ‘Well, what does your day look like?’” Vallone told me. They had no script to follow, so they could write their own. They envisioned giving themselves equal roles from the start, much like how many same-sex couples share a more equal division of labor, because they do not come in with the gender baggage of a heterosexual relationship.
Read: The gay guide to wedded bliss
What Vallone and Berryman did not want was to lapse into the roles that they watched their friends fall into, where the birthing parent becomes the breastfeeding parent becomes the default parent. The arrival of a new baby is a delicate time in any relationship—for many reasons, but in no small part because it disrupts whatever division of labor was previously agreed upon. Here is a tiny helpless human, along with a mountain of new tasks necessary to keep them alive. If the baby is breastfed, now a large share of that labor can be done by only one parent. In her case against breastfeeding in The Atlantic in 2009, Hanna Rosin described how that initial inequality persists and festers over the years: “She alone fed the child, so she naturally knows better how to comfort the child, so she is the better judge to pick a school for the child and the better nurse when the child is sick, and so on.” But what if—under very specific circumstances at least—breastfeeding did not fall solely on one parent? What if instead of parenthood starting off on unequal footing, it could be perfectly equal from the very beginning?
For a while, Vallone and Berryman did trade off feedings, and both continued to pump, because they worried that their milk supplies would drop. They tracked every ounce in a shared spreadsheet. (This careful data logging actually allowed Schnell to write a case study about the couple.) The pumping eventually became too much—they couldn’t sleep if they were pumping!—but they have kept co-nursing for two years now.
From the early days, they saw that nursing not only nourished their baby but also soothed her when she cried, made her sleepy when she was tired but fussy. So the work of not just feeding but all-round caregiving fell on them more equally. In the morning, they could alternate one person waking up early with the baby, the other sleeping in. At night, one parent could go out with friends without racing home for bedtime or pumping a bottle of breast milk for the other to feed. Because they could each provide everything their baby wanted, they were also each freer. Breastfeeding simultaneously deepened their relationships with their baby and allowed them a life outside of that. “You really get a sense of how radical it is to have caretaking split so evenly,” Vallone said. The couple is now trying for their second child, which Berryman plans to carry. They plan to co-nurse again.
Vallone and Berryman did, however, run into an unexpected obstacle to their co-nursing: their baby. She at one point refused to nurse on Vallone, the birthing parent, and wanted to nurse only on Berryman. Any parent is probably familiar with how babies can develop seemingly arbitrary preferences: breast over bottle, left breast over right breast, even. As they get older, toddlers, too, go through periods of wanting only one parent or another to feed, clothe, bathe, or comfort them. In this case—as in many cases—Vallone and Berryman had to be deliberate about returning to a more even state. At its most intense, Berryman would sleep away from the baby in another room; it got better over time, but it also sometimes got worse. Equality did not come easily even with two nursing parents, which perhaps isn’t surprising. The advent of formula did not magically render all marriages equal. Vallone and Berryman still had to work toward keeping their co-nursing relationship as balanced as possible. Dividing work is also, well, work.
Read: Lessons from 40 men in egalitarian relationships
Not all couples who induce lactation end up splitting breastfeeding evenly. Some are not able to, and some don’t even want to. For example, one parent might choose to carry the baby while the other takes on breastfeeding. Some of the women I spoke with were primarily motivated to induce lactation to pass along their antibodies in breast milk, or to physically bond with a baby they did not carry. Even for those who never made more than a few of the roughly 25 ounces a baby typically needs every day, being able to comfort nurse—when a baby sucks more for soothing than for nourishment—was meaningful. They could nurse their baby to sleep or calm them when upset. It brought the parents closer together too: Although inducing lactation is not equivalent to pregnancy, both parents felt like their bodies were preparing for a baby together. And later, they could troubleshoot a bad latch or clogged duct together. Breastfeeding can be an isolating experience when one parent is attached to a baby eight times a day and the other looks on a bit helplessly; co-nursing made it less so.
Because induced lactation has flown under the radar of mainstream science for so long, a lot remains unknown. A couple of small studies suggest that the protein and sugar content of induced breast milk is in the normal range, but detailed experiments into, for example, the mix of antibodies have never been done. And why are some women inducing lactation able to produce more than others? Schnell has noticed that those who have struggled with infertility or hormonal balances usually make less milk. She has worked with trans women, too, who are able to make milk, though usually not in large amounts. Men, theoretically, could lactate as well; early studies into domperidone actually noted this as a side effect. There are anecdotal reports of men breastfeeding infants, but there’s virtually no research into the phenomenon.
One mother I interviewed, Morgan Lage, told me that her experience inducing lactation to breastfeed her daughter inspired her to train as a lactation consultant, and she hopes now to fill in some of the many unknowns. The Newman-Goldfarb protocol is widely used as the template for anyone attempting induced lactation, but no one has rigorously studied the optimal time to initiate pumping or birth control. Lage started pumping earlier than the protocol suggested, and she wonders if that’s why she was able to have a full milk supply despite never having breastfed before. She loved nursing her daughter. She loved feeling “just as important and needed” in the fleeting, precious period of infancy.
Read: Breastfeeding at any cost
I know what Lage means about feeling needed, though perhaps because I breastfed solo—as most mothers do—I did not always love it. Still, I remember staring at my baby’s eyelashes and toes, marveling at how nearly every molecule in her body came from mine. We did supplement with formula, too, in part because we wanted my husband to be involved in her feeding. Although the bottle satisfied her hunger, it did not always satisfy some primal need for comfort. During her most inconsolable nights, my husband would spend hours trying to soothe her with every trick in the book, only for her to fall quiet and asleep the minute I nursed her. This frustrated us both. To be needed this way was a burden and a joy. I was sorry, for both of us, that we could not share it.