[ad_1]
KCCI EIGHT NEWS AT TEN. THIS IS AN EXAMPLE OF IOWA. AWESOME. A BONDURANT NEIGHBORHOOD CAME TOGETHER TO HELP A THREE YEAR OLD WITH CANCER CELEBRATE HALLOWEEN. A BIT EARLY. YOU’RE GOING TO SEE THE LITTLE MAN RIGHT THERE. AND LOOK AT THAT SMILE ON HIS FACE. KCCI ABIGAIL CURTIN SPOKE WITH HIS PARENTS TO LEARN HOW ALL THE SUPPORT IS HELPING HIM THROUGH TREATMENT. GRIFFIN CELLARS IS KNOWN AS A GIGGLE MONSTER. AT LEAST THAT’S WHAT HIS PARENTS, ASHLEY AND KENNY CELLARS, CALL HIM. BUT SINCE BEING DIAGNOSED WITH STAGE FOUR, PINEOBLASTOMA, A RARE FORM OF BRAIN CANCER EARLIER THIS YEAR, IT’S BEEN HARD TO KEEP A SMILE ON HIS FACE. THE HIGH DOSE CHEMO IS HARD. VERY HARD ON THE BODY. YOU KNOW, YOU THEIR KIDS GET CHEMICAL BURNS INSIDE OR OUTSIDE THEIR BODY. HE’S GOT BURNS IN HIS THROAT. HE DOESN’T EAT. HE’S LOST A LOT OF WEIGHT. PUKING ALL THE TIME. NORMALLY, THEY SAY THEY TAKE HIM TRICK OR TREATING FOR HIS FAVORITE HOLIDAY TO BOOST HIS SPIRITS. BUT BEING SO SICK MEANS PARTICIPATING ON HALLOWEEN WASN’T REALLY A POSSIBILITY FOR GRIFFIN. SO HIS PARENTS TOOK TO SOCIAL MEDIA WITH A PLAN IN THEIR NEIGHBORHOOD FACEBOOK PAGE. THEY ASKED SOME OF THEIR NEIGHBORS TO GATHER AND HAND OUT CANDY, ALLOWING GRIFFIN TO GET A TASTE OF HALLOWEEN MAGIC HE NEEDED, AND THEY DELIVERED. DRESSING IN COSTUMES AND HANDING OUT CANDY. WEEKS OUT FROM THE ACTUAL HOLIDAY, ALL THE NEIGHBORS WE SPOKE WITH SAID HELPING OUT WAS AN EASY CHOICE. IT’S GOOD TO BE PART OF THE COMMUNITY AND TAKE CARE OF EACH OTHER, AND THEY ARE ALWAYS THERE FOR US, EVEN ONES FROM THE NEXT NEIGHBORHOOD OVER. NONE OF US KNOW WHEN OUR LAST DAY IS, BUT YOU JUST WANT TO MAKE EVERY DAY FOR HIM A LITTLE BIT MORE SPECIAL. BUT AS YOU CAN SEE FROM THIS PICTURE, GRIFFIN MADE OUT LIKE A BANDIT. BUT HIS PARENTS SAY WHILE THE CANDY IS GREAT, THE BEST PART IS SEEING HIS SPARKLE COME BACK IN. BONDURANT ABIGAIL CURTIN, KCCI EIGHT NEWS. IOWA’S NEWS LEADER. NOW WE’RE THINKING ABOUT YOU AND SENDING HEALING WISHES YOUR WAY. GRIFFIN. A PART OF THE FAMILY’S STRUGGLE IS THE FACT THAT BECAUSE GRIFFIN’S CANCER IS SO RARE, THE TREATMENTS FOR IT ARE INCREDIBLY LIMITED. BUT THAT’S WHY THEY’RE HOPING TO RAISE AWARENESS. TO LEARN MORE ABOUT HOW YOU CAN HELP, CHECK O
Iowa community rallies to bring Halloween early for boy with rare cancer
Updated: 10:22 AM PDT Oct 19, 2025
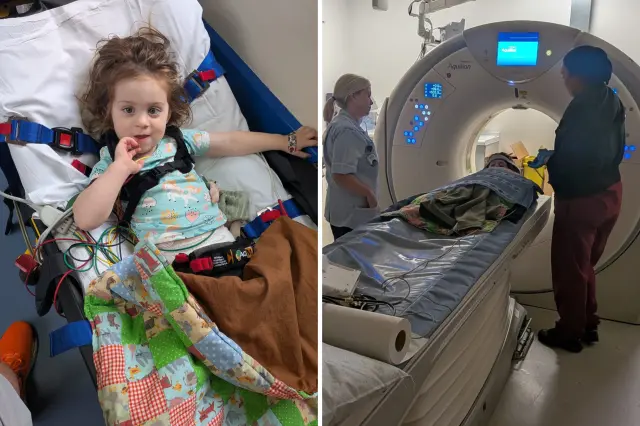
Gryffin Sellers is known as a giggle monster. At least, that’s what his parents, Ashley and Kenny Sellers, call him. But since being diagnosed with stage 4 pineoblastoma, a rare form of brain cancer, in April, they say it’s been hard to keep a smile on his face.”High-dose chemo is hard. Very hard on the body,” Ashley said. “The kids get chemical burns inside, outside their body. He’s got burns in his throat, he doesn’t eat, he’s lost a lot of weight puking all the time.”Normally, she says, they’d take him trick-or-treating to help raise his spirits on his favorite holiday. But because he’s so sick and his treatment has taken such a toll on the 3-year-old’s body, his parents put out a plea on social media, asking their Bondurant neighbors to come together and pass out candy weeks before the actual holiday.Dozens of families delivered.”It’s just good to be part of the community and take care of each other,” Jeffery Conroy, the Sellers’ neighbor, said. “They’re always there for us.” Even neighbors several streets over, like Beth Rodas, took part.”None of us know when our last day is, but you just want to make every day for him a little bit more special,” she said.Gryffin’s parents say he made out like a bandit, collecting so much candy that they plan to give some of it to his nurses. But the best part is easily seeing his sparkle come back.”I feel like his spirit is kind of back because now he’s in the mindset of, I got all this candy to eat, so I need to go do treatment and get home so I can eat my candy,” Ashley said. Gryffin still has a few more rounds of high-dose chemo left, but beyond that, Ashley says there isn’t much else doctors can do. Pineoblastoma is so rare that it makes up less than 0.2% of brain tumors diagnosed in the country, according to the Cleveland Clinic. Because it’s so rare, there isn’t much research devoted to it, leaving families like Gryffin’s seeking older treatments. “His treatment plan is from 2003 for a cancer that’s not even his,” Ashley said. “That’s over 20 years old with no new research, no changes, no nothing.” Even harder, the Pediatric Brain Tumor Consortium, which leads many of the early clinical trials used to treat rarer tumors like Gryffin’s, is losing funding next year. That’s why Ashley and Kenny hope to raise awareness about the cancer in the first place: so that families in the future won’t have to rely on imperfect treatments.For more information on Gryffin’s story and to donate to help the family, click here.
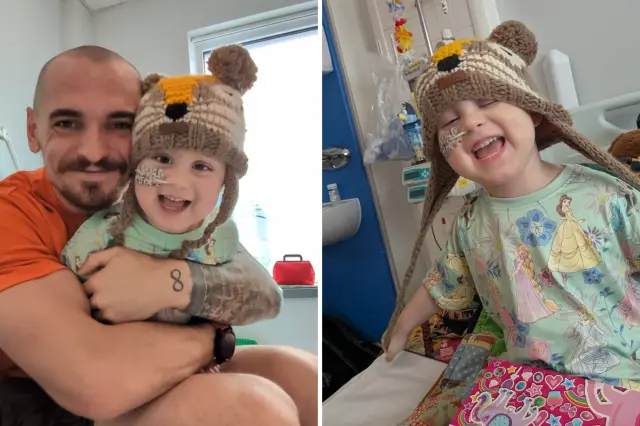
Gryffin Sellers is known as a giggle monster.
At least, that’s what his parents, Ashley and Kenny Sellers, call him.
But since being diagnosed with stage 4 pineoblastoma, a rare form of brain cancer, in April, they say it’s been hard to keep a smile on his face.
“High-dose chemo is hard. Very hard on the body,” Ashley said. “The kids get chemical burns inside, outside their body. He’s got burns in his throat, he doesn’t eat, he’s lost a lot of weight puking all the time.”
Normally, she says, they’d take him trick-or-treating to help raise his spirits on his favorite holiday. But because he’s so sick and his treatment has taken such a toll on the 3-year-old’s body, his parents put out a plea on social media, asking their Bondurant neighbors to come together and pass out candy weeks before the actual holiday.
Dozens of families delivered.
“It’s just good to be part of the community and take care of each other,” Jeffery Conroy, the Sellers’ neighbor, said. “They’re always there for us.”
Even neighbors several streets over, like Beth Rodas, took part.
“None of us know when our last day is, but you just want to make every day for him a little bit more special,” she said.
Gryffin’s parents say he made out like a bandit, collecting so much candy that they plan to give some of it to his nurses.
But the best part is easily seeing his sparkle come back.
“I feel like his spirit is kind of back because now he’s in the mindset of, I got all this candy to eat, so I need to go do treatment and get home so I can eat my candy,” Ashley said.
Gryffin still has a few more rounds of high-dose chemo left, but beyond that, Ashley says there isn’t much else doctors can do.
Pineoblastoma is so rare that it makes up less than 0.2% of brain tumors diagnosed in the country, according to the Cleveland Clinic. Because it’s so rare, there isn’t much research devoted to it, leaving families like Gryffin’s seeking older treatments.
“His treatment plan is from 2003 for a cancer that’s not even his,” Ashley said. “That’s over 20 years old with no new research, no changes, no nothing.”
Even harder, the Pediatric Brain Tumor Consortium, which leads many of the early clinical trials used to treat rarer tumors like Gryffin’s, is losing funding next year.
That’s why Ashley and Kenny hope to raise awareness about the cancer in the first place: so that families in the future won’t have to rely on imperfect treatments.
For more information on Gryffin’s story and to donate to help the family, click here.
[ad_2]