[ad_1]
Lacy was an outgoing, fun nine-year-old. Then, one night, everything changed. She became a shell of herself.
Her mother, Crystal, 30, from Illinois, told Newsweek she can only describe last year as “hell.” Doctors said her first-born had anxiety and depression — but Crystal’s instincts told her something else was happening.
Recently, Crystal shared a TikTok video on (@crysrenae) showing Lacy on her ninth birthday, sitting in front of a watermelon wedge with candles, her face blank beside her excited younger brother. The clip then cuts to this year: The same girl grinning from ear to ear in front of cake. The transformation has struck a chord online, drawing almost 40 million views.
Crystal says the change came after Lacy received the right diagnosis and treatment. Now, she’s using her platform to raise awareness about pediatric acute-onset neuropsychiatric syndrome, or PANS — a condition in which children develop sudden obsessive-compulsive symptoms or restrictive eating, alongside an abrupt and dramatic behavioral decline. The syndrome is often linked to infections, though a clear trigger isn’t always identified.
The PANDAS Physicians Network (PPN) explains a related condition, PANDAS — pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections — is considered a subtype of PANS. It follows the same sudden-onset pattern but is specifically tied to a recent strep infection and can include tics and neurological changes.
What Are the Symptoms?
Children with PANS or PANDAS don’t just develop OCD-like behaviors or eating restriction overnight. They also experience a rapid onset of at least two other serious symptoms.
These can include:
- Severe anxiety
- Mood swings or depression
- Irritability or aggression
- Regression in behavior
- Sudden academic decline
- Motor or sensory abnormalities
- Physical issues such as sleep disruption
Lacy suffered with all of the above; her mom told Newsweek that she was suddenly full of “rage.”
What May Cause It?
The PPN states researchers with believe simultaneous exposure to multiple infections can essentially “misfire” the immune system. In some cases, that may mean the body’s normal safeguards fail, allowing immune cells to attack healthy tissue. In others, the immune system may become overactivated and mistakenly target neuronal cells. Genetics may also play a role, with some children more predisposed to these abnormal immune responses than others.
How Lacy “Changed Overnight”
Crystal said the earliest signs appeared after Lacy developed food poisoning. She became intensely fearful of vomiting and started showing separation anxiety. She also stopped enjoying toys and TV shows.
“She was checked out,” Crystal told Newsweek. “Little did we know that was the beginning of PANS.”
Then, in July, her symptoms escalated dramatically.
“She had a mental break and almost had an episode of psychosis,” her mother recalled. “One night, she became out of touch with reality and started banging on my door in the middle of the night, saying she needed to go to the hospital.
“She didn’t know why, but she knew something was happening.
“After that, she had many fear episodes, it was insane. She became a fear-ridden kid.”
Lacy was seen by multiple doctors and repeatedly diagnosed with anxiety and depression. But Crystal says the behavior looked like something deeper — and far more frightening.
“It seems horrible to say, but she almost seemed possessed, like something came over her body.
“She was trying to run away. She felt trapped and was in utter terror.”
Lacy began expressing suicidal thoughts, she destroyed her bedroom multiple times and smashed a window. By August, she was begging to be admitted to a psychiatric ward.
“Everything happened so fast, she started to try and hurt herself and us,” Crystal said.
“Anxiety wasn’t even the right word; she was scared of herself and so were her siblings.”
Crystal said psychiatrists struggled to explain what was happening. Feeling out of options, the family started researching on their own — and came across PANS.
“I was trying to figure out what happened, because I didn’t know who this child was,” she said.
The Search for Help
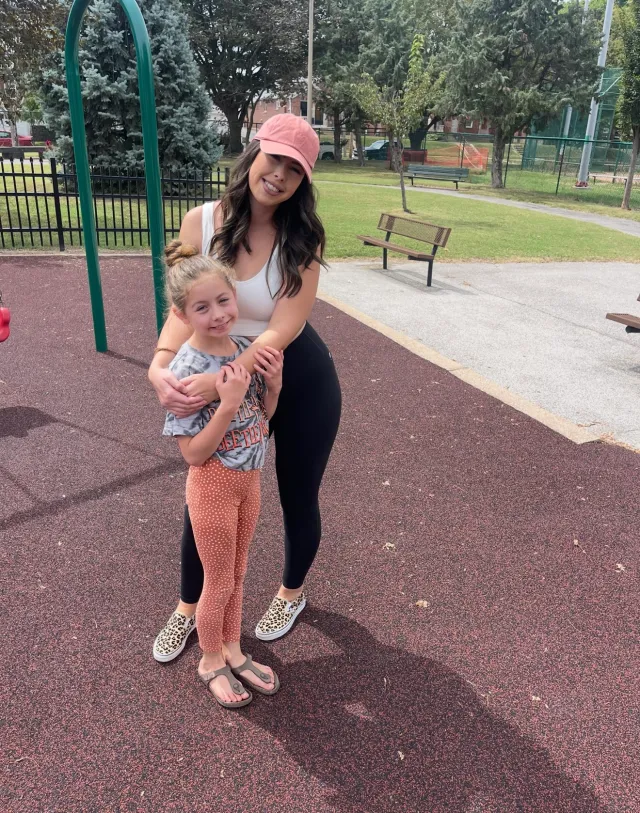
Crystal took Lacy out of the psychiatric ward in September, and her family drove to Indiana to see a PANS specialist.
“I didn’t know it was a controversial diagnosis or that it would be an issue to get the diagnosis,” Crystal said.
“It was the hardest thing I have ever dealt with, and I think I have post-traumatic stress disorder from it.”
She stressed there were no major life events that could explain the shift and that Lacy’s grandmother moved in to help manage the chaos at home.
“There were times when I thought she was going to kill one of us — not necessarily meaning to — but I thought my parents were going to have a heart attack from stress,” Crystal said.
Lacy’s symptoms were often quieter in the morning, then worsened at night. She refused to sleep. The family cycled through care options, many of which were not covered by insurance.
“A lot of insurance companies do not cover it, so we had to pay out of pocket,” Crystal said.
“If it wasn’t for my parents, we wouldn’t have been able to fund it.”
She estimates her parents spent more than $10,000 on testing and medication. Bloodwork screened for infections and abnormal antibodies.
A Turning Point

“From what I understand, her immune system attacked her brain, causing inflammation — autoimmune encephalitis — and she didn’t have control of her brain,” Crystal said.
The family tried multiple antibiotics before one began to help. In December 2024, doctors recommended adding a very low-dose antipsychotic alongside antibiotics.
“We were against it but we were so desperate,” she said.
“It was a turning point.”
On Christmas Day last year, Crystal said she saw her daughter return.
“It was a miracle — she was happy, smiling, and living life again,” she said.
Since then, Lacy has continued improving. She’s had setbacks, but her mother says she is largely back to herself. She also receives IVIG infusions, a treatment aimed at regulating immune function and preventing relapse.
“Today, she is living life again — doing extracurricular activities and hanging out with her friends,” Crystal said.
“I didn’t think this would be possible one year ago.”
“She wasn’t eating then, and now she almost doesn’t have anxiety anymore.”
“We are all doing much better as well.”
“You Aren’t Alone”
Crystal says she’s sharing Lacy’s story for the families who are still in the spiral she remembers all too clearly.
“I want people to know they aren’t alone,” she said.
“I was looking for anything I could find, desperate to find other parents going through it.”
“I felt like I was living a life that nobody knew about.”
“I felt alone and desperate to find other parents.”
[ad_2]




