[ad_1]
Trump administration health officials plan to remove a vaccine ingredient that’s been safely in use for decades, aluminum.
The Trump administration’s Department of Health and Human Services has reduced some vaccine access. The agency scaled back COVID-19 vaccine recommendations, approved COVID-19 vaccines for fewer people and aimed to remove the preservative thimerosal from U.S. vaccines. Experts told PolitiFact scientific research did not support its removal.
During a Sept. 22 press conference in which President Donald Trump told people not to take Tylenol during pregnancy, he also mentioned another objective: “We want no aluminum in the vaccine,” he said. The administration was already in the process of removing aluminum from vaccines, he added.
About two weeks later on Oct. 8, the U.S. Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices, or ACIP, announced a new working group focused on the childhood vaccine schedule. Its discussion topics include vaccine ingredient safety and “aluminum adjuvants.”
Robert Malone, an ACIP member who has opposed COVID-19 vaccines, told Axios he expected the committee would determine there was “a lot of evidence” of “issues” with aluminum in vaccines. The committee likely would vote to recategorize vaccines containing aluminum adjuvants so that people would have to discuss with their doctor before getting them, Malone told Axios.
That could have far-reaching ramifications. Here’s what to know about aluminum in vaccines.
Q: Why is a metal such as aluminum in some vaccines?
A: Small amounts of aluminum are sometimes included in vaccines as adjuvants, or substances that boost the body’s immune response to the vaccine to ensure protection from infection.
That boost means people can get fewer vaccine doses in smaller quantities.
Q: When used, how much aluminum is in a vaccine?
A: Vaccines with aluminum adjuvants usually contain less than a milligram of aluminum per dose, according to the Children’s Hospital of Philadelphia.
That’s a pretty abstract number. To help make it more concrete: A milligram is one-thousandth of a gram. One gram is about the weight of a raisin or a stick of gum. Imagine cutting one of those items into 1,000 equal pieces. One of the pieces would be about 1 milligram.
Here’s another way to think about it.
People come in contact with and consume aluminum all of the time. It is one of the most abundant metal elements in the earth’s crust, according to the U.S. Geological Survey. It’s naturally occurring in soil, air and water. Food is the main way people are exposed to aluminum. The average adult eats about 7 to 9 milligrams of aluminum per day, according to the Centers for Disease Control and Prevention.
A baby in its first six months might receive a total of about 4.4 milligrams of aluminum from recommended vaccines. In the same period of time, a breastfed infant would ingest about 7 milligrams of aluminum from breastmilk and a formula-fed baby would ingest about 38 milligrams from formula.
Q: How long have vaccines contained aluminum?
A: Aluminum adjuvants have been used in vaccines for more than 70 years, the CDC said.
“Aluminum is one of our oldest adjuvants, it’s been used in vaccines since the 1920s,” said Dr. Peter Hotez, a Baylor College of Medicine professor and codirector of Texas Children’s Hospital Center for Vaccine Development.
Q: How do we know it’s safe to include small amounts of aluminum in vaccines?
A: Every vaccine’s safety and efficacy is tested in animal studies and human clinical trials before the U.S. Food and Drug Administration licenses it for public use. Every vaccine containing adjuvants has been tested and health agencies continuously monitor their safety, the CDC said.
Over several decades of use, vaccines with aluminum adjuvants have been proven safe, the FDA said.
Vaccines containing aluminum have been “given to billions of people worldwide now,” said Dr. Kawsar Talaat, a professor at Johns Hopkins’ Bloomberg School of Public Health.
A growing body of research has also found aluminum adjuvants don’t cause aluminum toxicity or other adverse outcomes.
Q: Do aluminum adjuvants have any risks?
A: Rarely, some people have allergic reactions to aluminum in the same way they might have allergic reactions to other substances, Talaat said.
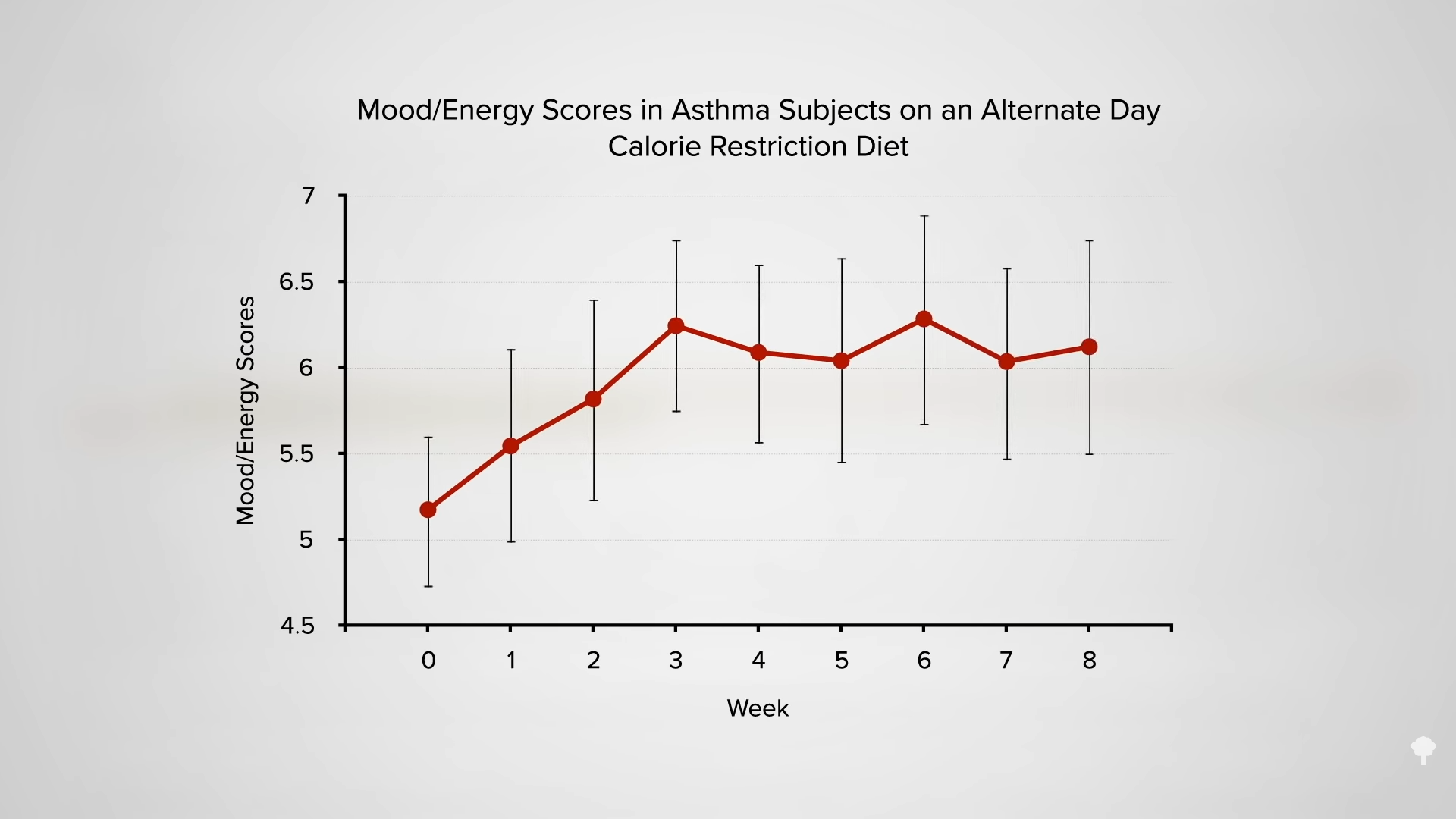
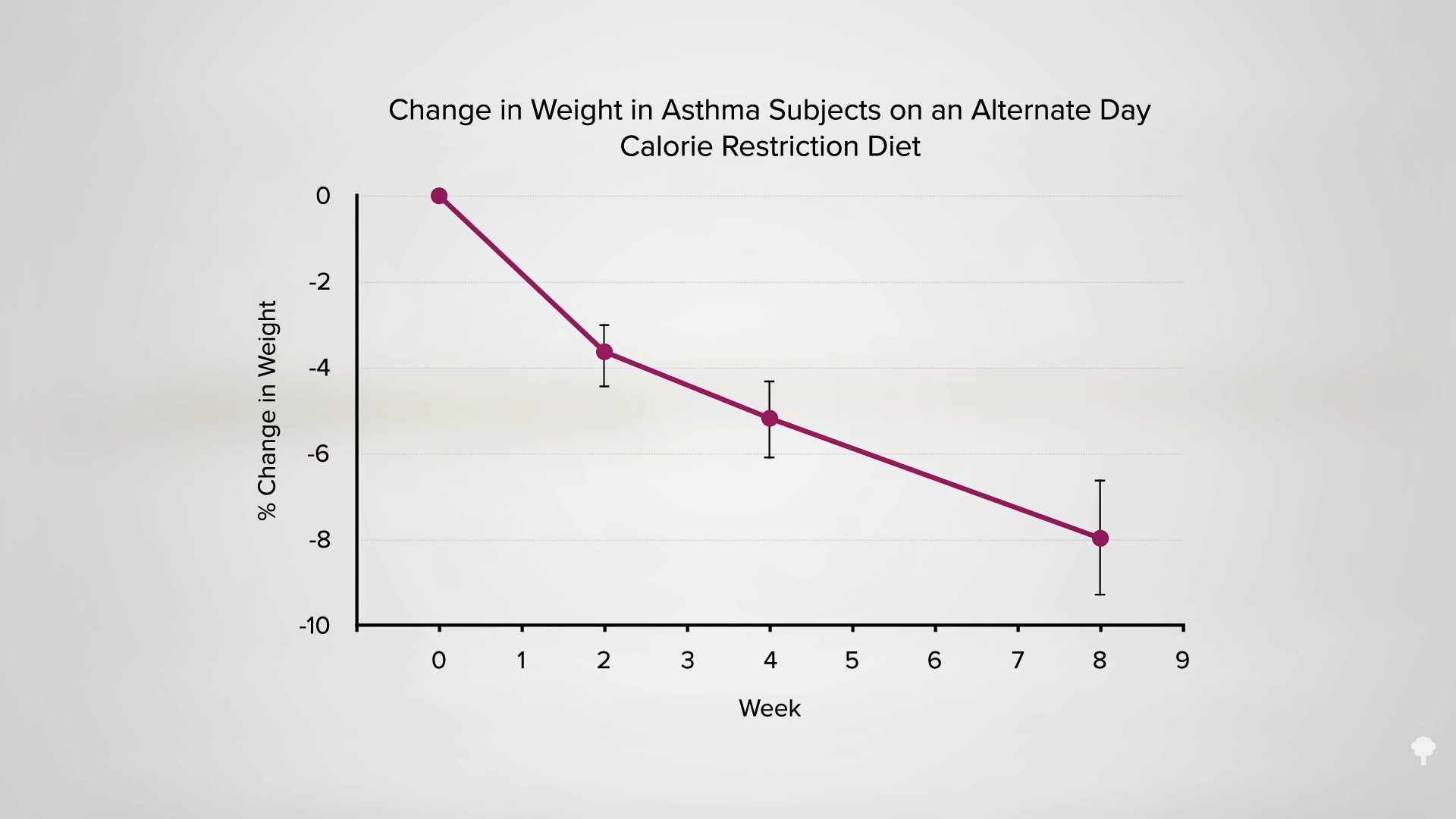
In 2022, researchers published a retrospective, observational study on more than 325,000 children that found an association between vaccine-related aluminum exposure and persistent asthma. Association is not the same as causation, meaning the study did not prove a link between aluminum in vaccines and asthma.
Experts from the CDC and American Academy of Pediatrics encouraged more research on the subject because the backward-looking observational study didn’t prove causation and also had limitations — including that it excluded many children who developed asthma before they turned 2 years old.
A 2025 study found no increased risk of asthma associated with childhood exposure to aluminum-absorbed vaccines.
Q: Which vaccines contain aluminum adjuvants?
A: At least 25 vaccines approved for use in the U.S. have aluminum adjuvants, the CDC says. That includes vaccines that protect against HPV, hepatitis A and B and diphtheria, tetanus, and acellular pertussis (whooping cough).
Q: Which vaccines do not contain aluminum adjuvants?
The CDC’s list of vaccines without adjuvants includes vaccines against COVID-19, Ebola, meningococcal, polio and rabies. Additionally, most seasonal flu shots and the vaccine against measles, mumps and rubella do not contain aluminum adjuvants.
Q: Can we remove aluminum from vaccines?
A: Not quickly. If it could be done at all, it would take years to develop, test and license new, aluminum-free vaccines. Many of the vaccines with aluminum adjuvants don’t have aluminum-free formulas.
“A vaccine is licensed based on all of its ingredients and the exact manufacturing process,” Talaat said. “If you were to take an ingredient out of a vaccine, you would have to start all over with the clinical trials and the manufacturing, and it is highly possible that some of these vaccines wouldn’t work without the aluminum in there.”
Although other adjuvants exist, they’re newer and often more scarce than aluminum, which is abundant.
An immediate ban on aluminum in vaccines would drastically reduce people’s ability to protect themselves and others against numerous diseases.
“I think we’d see outbreaks of vaccine-preventable diseases,” Talaat said.
Q: Why do people think aluminum in vaccines is causing autism?
A: A 2011 study said vaccines with aluminum adjuvants “may be a significant” contributing factor to the rising number of autism diagnoses in kids, Nature reported.
A year later, a World Health Organization vaccine safety committee called the 2011 study “seriously flawed.” The 2011 study and another by the same authors compared vaccines’ aluminum content and autism rates in several countries, the WHO group said, but that cannot be used to establish a causal relationship.
“We studied aluminum, and have no link between aluminum and autism,” Talaat said.
RELATED: No, vaccines do not contain unsafe amounts of aluminum for infants, research shows
[ad_2]