[ad_1]
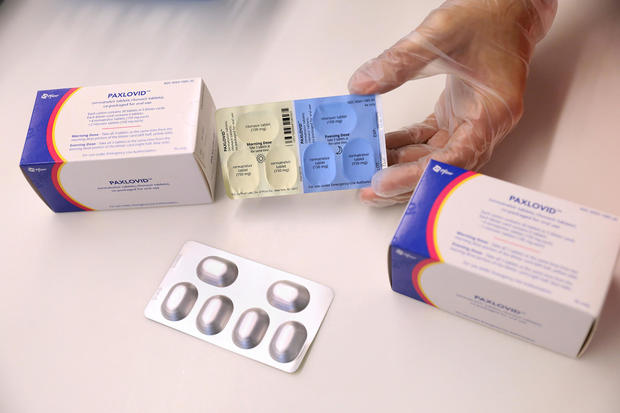
The commercials make it sound so simple: “If it’s COVID, Paxlovid.”
But the slogan, catchy though it may be, belies a harsher reality that some public health and elected officials have long acknowledged and worked to rectify: For many, getting access to the therapeutic should be much easier than it has been.
The issue is not one of scarcity, as the antiviral is widely abundant. Nor is pricing a major barrier, as Paxlovid is cheap or even free for many. Nor even is it an issue of how well it works, as studies have shown it to be highly effective.
The drug’s biggest impediment has been, and remains, the simple fact that a number of doctors are still declining to prescribe it.
Some healthcare providers hinge their reluctance on outdated arguments, such as the idea of “Paxlovid rebound” — the chance that people who take the drug have a chance of developing COVID symptoms again, generally about two to eight days after they recover.
As it turns out, anyone who gets COVID-19 has a similar rare chance of rebound.
COVID “rebound can occur with or without [Paxlovid] treatment,” scientists with the Food and Drug Administration wrote in a study published in December. “Viral RNA rebound was not restricted to [Paxlovid] recipients, and rebound rates were generally similar to those in placebo recipients.”
When told about one patient who was declined a prescription to Paxlovid because of concern about “Paxlovid rebound,” UC San Francisco infectious-diseases expert Dr. Peter Chin-Hong groaned.
“Oh my God, that’s so, like, bogus,” Chin-Hong said. “Clinicians having this weird idea about rebounds, it’s just dumb.”
Data indicate that most people don’t get COVID rebound, Chin-Hong said. And while rebound can occur, the possibility should not dissuade people “who might really need it” from taking an antiviral.
Even if COVID rebound happens, and symptoms do occur, “they tend to be mild and do not require repeating the treatment,” according to the California Department of Public Health.
Officials at both the federal and state level have implored healthcare providers to properly prescribe Paxlovid and other antivirals when indicated.
“Antivirals are underused,” the Centers for Disease Control and Prevention said in a statement Thursday. “Don’t wait for symptoms to worsen.”
In its own advisory, the California Department of Public Health said, “Most adults and some children with symptomatic COVID-19 are eligible for treatments … Providers should have a low threshold for prescribing COVID-19 therapeutics.”
Aside from Paxlovid, one alternative oral antiviral treatment is known as molnupiravir. There’s also remdesivir, which is administered intravenously.
The CDC says Paxlovid and remdesivir are the preferred treatments for eligible COVID-19 patients.
“Don’t delay: Treatment must be started within five to seven days of when you first develop symptoms,” the CDC says.
A reference to Paxlovid and other antivirals is even in a musical radio ad from California health authorities that has been broadcast throughout the state: “Test it. Treat it. You can beat it,” with the ditty later continuing: “Medication is key / To slow the virus in your body.”
Yet there is wide documentation of the low frequency of prescribing Paxlovid and other antivirals, and that can have significant consequences for higher-risk COVID-19 patients. A report published by the CDC Thursday reviewed 110 COVID-19 patients considered high-risk and found that 80% of them were not offered antiviral treatment.
A big reason given by the patients’ providers, all of whom were under the Veterans Health Administration, was that their patient’s COVID symptoms were mild.
But as officials note, that’s exactly what antivirals are for.
“There is strong scientific evidence that antiviral treatment of persons with mild-to-moderate illness, who are at risk for severe COVID-19, reduces their risk of hospitalization and death,” the CDC says.
Risk factors for severe COVID-19 include being age 50 and up; not being current on COVID vaccinations; and a wide array of medical conditions, such as diabetes, asthma, kidney disease, heart disease, having anxiety or depression, and being overweight. Other factors that influence health, such as limited access to healthcare and having a low income, can also heighten someone’s risk.
Another reason providers may cite to not prescribe COVID antivirals, California officials said, is the chance of serious side effects. But that fear is largely erroneous, as “most people have little-to-no side effects,” the California Department of Public Health says. Some of the more common side effects after taking Paxlovid are developing a temporary metallic taste in the mouth, which occurs in about 6% of recipients, and diarrhea (3%).
However, some people who do take Paxlovid may need to have other medications adjusted, according to the agency.
The other antiviral pill option, molnupiravir, “has very few side effects, but you cannot take it if you are pregnant,” the state agency said.
Clinicians may also be reluctant to prescribe Paxlovid for younger adults, “not because it causes harm, but because it in some studies doesn’t show as much benefit,” Chin-Hong said. Younger, healthy people are generally unlikely to die from COVID or become ill enough to require hospitalization even without antiviral treatment.
But some data do suggest that patients who take Paxlovid clear out coronavirus from their bodies faster.
“What we’re finding is that people are turning negative very quickly with Paxlovid,” Chin-Hong said.
And one report, published in the journal Emerging Infectious Diseases, suggests widespread use of Paxlovid “would not only improve outcomes in treated patients but also … reduce risks of onward transmission.”
So if an initial clinician turns you down for a Paxlovid prescription, and you think you qualify, what other options are there?
One possibility is reaching out to another healthcare provider who might be either more knowledgeable about Paxlovid and other antiviral medications or more open to prescribing them.
Los Angeles County residents can call the county’s public health info line, (833) 540-0473, to discuss treatment options with a health provider.
Californians who don’t have insurance or have a hard time getting anti-COVID-19 medication can schedule a free telehealth appointment by calling (833) 686-5051 or visiting sesamecare.com/covidca. Medication costs may be subject to a copay, depending on your insurance.
A program funded by the National Institutes of Health, featured at test2treat.org, gives adults who test positive for COVID-19 or flu free access to telehealth care and treatment.
[ad_2]
Rong-Gong Lin II
Source link