[ad_1]
ST. PETERSBURG, Fla. — When it comes to organ donations and those in need of a transplant, numbers show there are some serious racial disparities.
It’s a gap in life-saving health care that experts say, many times, is rooted in mistrust and misinformation, and it’s affecting the Black community in record numbers.
Some local donor advocates are sharing their stories to encourage more people to consider life-saving and life-changing options.
Jacquez Welch, 18, was the picture of perfect health, until he wasn’t.
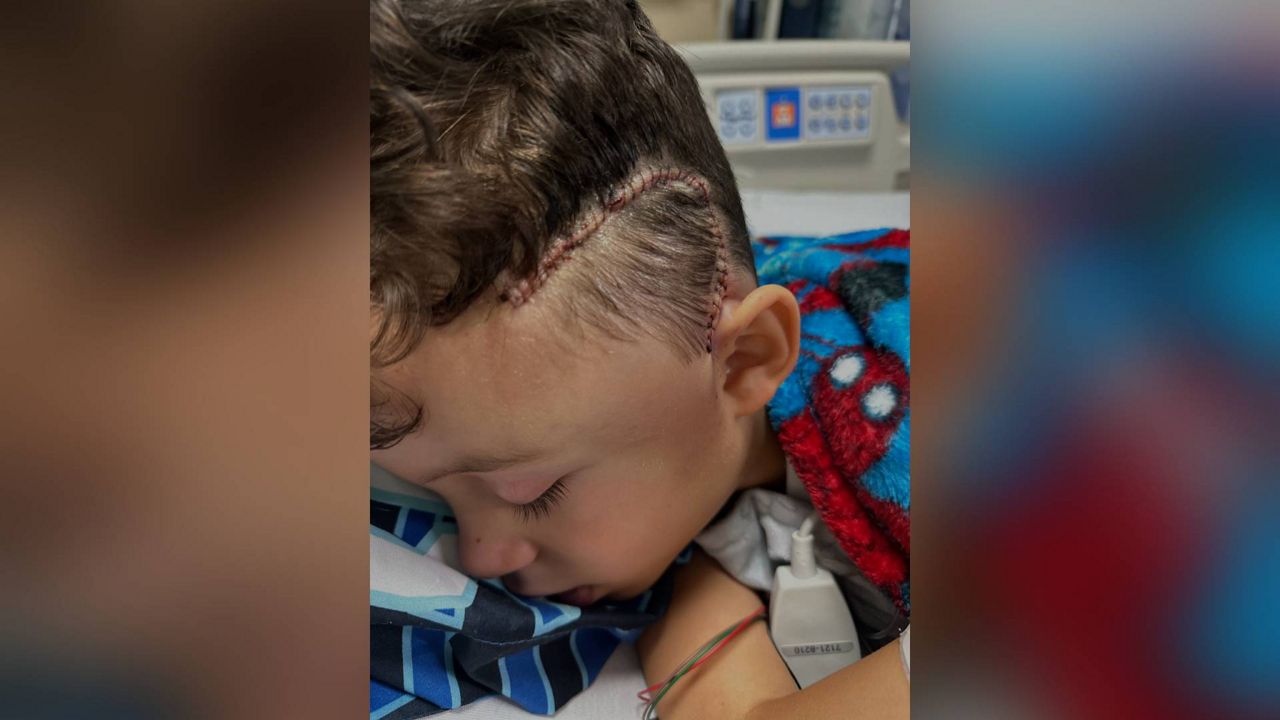
“Perfectly healthy. No health issues,” his mother, Marcia, said. “One day at a football game, Friday night lights, he collapsed on the field, and he had a stroke. Got him to the hospital, did tests and found out he had AVM.”
It was an arteriovenous malformation, a tangled web of blood vessels in the brain that can burst without warning. Marcia said her son was in good health his entire life. So when she watched him collapse at the game, she was shocked. She said there were no warning signs.
“Me, I thought he was just cramping because a lot of time he cramps. But when he didn’t get up and the coach signaled me down, I knew it was serious then,” she said.
She learned the condition could’ve taken her son’s life at any time.
“It’s basically veins in your brain that develops when you’re born and then they tangle up and then they burst and have a stroke,” she said. “What he has is not genetic. It’s not genetic at all. That was my first thing. What if my other kids have it because they all played football? Even my girls. They say it’s nothing genetic. It’s just something that happened while he developed in my stomach while I was pregnant.”
Marcia said she got educated quickly about her son’s condition. After a few days on life support and learning there was no chance of survival, she had to make a difficult decision. She is grateful Jaquez had already made his wishes clear.
“We decided to donate his organs when he was 16,” she said. “We went to the DMV to get his driver’s license. And they asked him, and he looked at me and was like, ‘Mom, what does that mean?’ I said that means when you’re gone, you pass away, and somebody takes your organs you can’t use anyway.
“And he looked at me and said, ‘Sure, why not.’”
Marcia lost her son, but she says he was able to save the lives of four people and donate tissue to more than 70 patients.
“He gave his heart, liver, both of his kidneys, pancreas,” she said. “I know it was seven organs.”
It’s the kind of giving people like the Rev. Kenny Irby are counting on. He has a genetic disorder that he learned he was living with years ago, and over time he learned how it affected his family for decades.
“I was diagnosed with polycystic kidneys,” Irby said. “My family migrated from Newberry, South Carolina, to Washington D.C. because my grandmother had what was called then, the disease. And the doctors in South Carolina told my great grandmother, ‘You have to get her to the north. The hospitals here can’t treat her.’”
Reverand Ibry is known for his work with the nonprofit, Men in the Making, and his work as the Faith in Community Justice Liaison with the city of St. Pete. He’s also the former pastor of one of the area’s oldest Black churches. But even that couldn’t prepare him for this.
“I was diagnosed in 2022 with prostate cancer,” he said. “My wife had breast cancer in 2023, and so we went through 2024, and as soon as we got through that, I got the diagnosis on the renal failure.”
Irby said the chemo from his prostate cancer treatment worsened his kidney condition. Now, the man of faith, known for his giving, is in need of a gift himself. He needs a kidney donation.
“I actually did have two brothers that I’ve worked with over the years that said, I’d give you a kidney, but I’ve only got one. Because folks don’t even realize at that level you can live a functional and healthy life,” he said.
But finding a match can be harder, especially for Black patients.
According to the U.S. Department of Health and Human Services, Black Americans make up 27% of candidates on the transplant waiting list, and only about 13% of organ donors are Black. It’s a gap that has widened over time, leading to longer wait times.
Experts say a more diverse donor pool can help when it comes to finding the right match.
“It’s not that the donor and the recipient have to be the same race or the same ethnicity. But by having genetic variables in common, it helps to increase compatibility,” said LifeLink Florida Associate Medical Director and Recovery Surgeon, Dr. Jacentha Buggs.
LifeLink is an organ procurement organization.
“Our team here at LifeLink can’t even approach a family to talk to them about organ donation until one of two things have happened. The patient has been legally declared brain dead, or their injuries are so severe that they’re having conversations about withdrawal of care,” Buggs said.
She agrees that a history and hesitation to even be listed as an organ donor has created barriers for the Black community.
“There are valid reasons that people of color would distrust the medical system. Especially when you think about things that happened with the Tuskegee experiment and so forth. But what I think we have to do is meet people where they are,” she said.
Dr. Buggs said education and building trust are key to saving more lives.
For Reverend Irby, it’s going to take those efforts and a whole lot of faith.
“Certainly at the metaphysical level, when you think about it, when you’re gone, you’re not gonna need it. And if you can be a blessing and your organs and tissues can be a blessing to individuals and medical research, then I think you want to do that as a part of your legacy,” Irby said.
It’s a plan Marcia’s son made long before she learned to find purpose through her pain.
“Imagine your child needing a heart, a liver, imagine if it was your parent, a grandparent. Imagine you losing a child and all you have left is to give something to someone else,” Marcia said.
[ad_2]
Saundra Weathers
Source link